Image source: Unsplash/Erik Mclean
Article • Corona demographics
Why Covid-19 registries for cancer patients are so important
Due to compromised immune systems cancer patients are at higher risk of contracting infections. How does cancer impact on patients who also contract Covid-19? To collect this data, four cancer registries, one in the EU, one in the UK, two in the USA, have been established.
Report: Cynthia E. Keen
The first large, multi-institution study of the impact of Covid-19 was conducted in Wuhan, China, and presented at the virtual American Association for Cancer Research (AACR) Annual Meeting 2020 in April. The study included 105 cancer patients and 536 age-matched patients without cancer, and showed that Covid-19 patients with cancer had higher risk in intensive care unit (ICU) admissions and mortality. However, at the same conference, researchers from Gustave Roussy Cancer Campus in Villejuif, France, reported that 137 cancer patients diagnosed with the coronavirus in March did not have more lethal or aggressive disease than patients without cancer in the global population. Such conflicting reports supported the urgent need to acquire long-term global data.
Recommended article
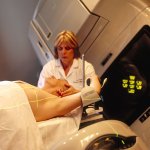
News • Radiation therapy
Call for action: Ensuring cancer treatment in times of COVID-19
The COVID-19 pandemic has affected virtually every aspect of healthcare provision - cancer care is no exception. In fact, during the pandemic, patients with cancer represent a high-risk group. Recent studies estimate that delays in cancer diagnosis and treatment will increase the indirect death toll of COVID-19 by several thousands in the coming years.
The UK Coronavirus Cancer Monitoring Project
The UK Coronavirus Cancer Monitoring Project (UKCCMP), established in mid-March 2020, was the first Covid-19 clinical registry to enable near real-time reports to frontline physicians about the effects of Covid-19 on cancer patients. Its objective is to monitor the impact of Covid-19 and enable oncologists to gain crucial insights and inform clinical- and infrastructure-based decision making. A live clinical data dissemination system provides a daily update to an interactive website; weekly reports are sent to individual UK cancer centres and clinicians.

In its first five weeks of operation, the UKCCMP accrued the largest prospective database of symptomatic and asymptomatic Covid-19 cancer patients globally. Approximately 80% of UK adult and 100% of paediatric cancer treatment centres are currently participating. As of mid-August, the cases of 2,314 adult and 61 paediatric cancer patients were enrolled in the database. ‘Our objective is to identify and learn from every case of Covid-19 in cancer patients in the UK,’ said Leonard Y W Lee MD PhD., an honorary research fellow of the Institute of Cancer and Genomic Studies of University Hospitals Birmingham and an executive lead of the project. ‘The number of cancer patients with Covid-19 in the UK is relatively small. But approximately 2.5 million individuals live with or have a history of cancer in the UK, with an estimated 1,000 new diagnoses each day. A substantial number of new cases require, are undergoing, or are recovering from surgery and complex treatments. One of the things we want to determine is if specific cancer treatments may differentially contribute to the risk of developing Covid-19.’
Results of a Covid-19 mortality study of 800 cancer patients who contracted Covid-19 between 18 March and 26 April revealed that patients receiving or who had received chemotherapy and/or radiotherapy within the past 30 days were not at greater risk of dying when compared with other cancer patients. However, age and comorbidities were significantly associated with Covid-19 related death of 28% of these patients, the researchers reported. ‘We also determined that cancer patients were at increased risk from Covid-19,’ Lee told Healthcare in Europe. ‘Globally, a mortality rate of 20-35% is being reported. It’s important for patients to undergo regular rapid Covid-19 testing, especially prior to each cycle of chemotherapy. Oncologists need to take decisive and active steps, such as screening regularly for Covid-19, to prevent infection while administering effective anti-cancer treatments for patients who have a rapidly progressive tumour.’
Recommended article
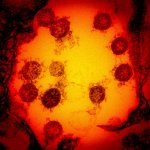
News • Caught in the loop
How COVID-19 leads the immune system astray
Contrary to what has been generally assumed so far, a severe course of COVID-19 does not solely result in a strong immune reaction – rather, the immune response is caught in a continuous loop of activation and inhibition.
The Covid-19 and Cancer Consortium (CCC19)
The Covid-19 and Cancer Consortium (CCC19), also established in mid-March, is collecting data to study the characteristics and course of illness among patients age 18 and older diagnosed with Covid-19 and a current or past diagnosis of invasive solid or haematologic malignancy. Currently, 120 institutions are participating, of which 11 are located outside the USA. The 11-member steering committee includes Professor Solange Peters MD PhD, head of the Medical Oncology Service of the University Hospital Lausanne, and the current president of the European Society for Medical Oncology (ESMO).
CCC19 is actively analysing and reporting findings from its registry, including a cohort study on the clinical impact of Covid-19, published open access in The Lancet (28 May 2020), and a study on the utilization of Covid-19 treatments and clinical outcomes among cancer patients, published open access (22 July) in Cancer Discovery.
The clinical impact study included 928 invasive cancer patients from Canada, USA and Spain who received treatment for Covid-19 between 17 March and 16 April 2020. The study’s primary endpoint was all-cause mortality within 30 days of Covid-19 diagnosis. This is an ongoing clinical trial (NCT04354701) with an accrual goal of 10,000 patients.
Patients ranged in age from18 to 90 years, with a median age of 66. The cohort had 20 different types of cancer in all stages, with 32% stable or responding to treatment, and 45% in remission or presumed cured. Three percent had surgical treatment within 30 days of contracting Covid-19, and 39% had received anticancer treatment in this time frame. The majority had two or more comorbidities; 51% had no smoking history. Thirteen percent died from Covid-19 within 30 days of contracting it. This highly detailed, early report suggested that cancer patients appear to be at increased risk of mortality and severe illness.
The treatment utilisation study included 2,186 adults, with a median age of 67, of whom 47% had mild, 40% moderate, and 12% severe baseline Covid-19 severity. Patient demographic and cancer characteristics, Covid-19 treatments received, and outcomes are discussed in detail. Sixteen percent died from Covid-19 within 30 days of contracting it, again reinforcing the vulnerability of cancer patients to the novel coronavirus.
ASCO Covid-19 and Cancer Registry

The American Society of Clinical Oncology (ASCO) launched the ASCO Survey on Covid-19 in Oncology Registry in early April, inviting oncology practices across the USA to share information about patients. ASCO established this registry to collect both baseline and longitudinal data on how the virus impacts on cancer care and cancer patient outcomes during the Covid-19 pandemic and into 2021. Data being collected includes characteristics of cancer patients most impacted by Covid-19, estimates of disease severity, treatment modifications or delays, implementation of telemedicine in the cancer treatment setting and clinical outcomes related to both Covid-19 and cancer.
Richard L Schilsky MD, ASCO executive vice president and chief medical officer, explained that whilst the ASCO Registry and CCC19 Registry have very similar objectives, the ASCO Registry collects more information on cancer treatment and outcomes, whereas CCC19 collects more data on Covid-19 treatments. Data is also updated on different schedules, with ASCO requesting that practices update their patients' Covid-19 status on a weekly basis and cancer status on a monthly basis. CCC19 is requesting 30- and 90-day outcomes. ‘As of mid-August, 45 oncology practices and cancer treatment centres have submitted data about 300 patients with 33 different types of cancer,’ Schilsky said. ‘ASCO is interested in collaborating with other Covid-19 and cancer registries to extend our findings and maximise our learning from data collection on the impact of Covid-19 on people with cancer.’
ESMO-CoCARE Registry
Launched on 29 April, the ESMO-CoCARE Registry provides Covid-19 data to cancer centres and organisations internationally (but not North America). With the most diverse geographic enrolment in the world, it is led by a steering committee of nine oncology experts from France, Germany, Portugal, Switzerland, the UK and USA. As of mid-August, participation of cancer treatment centres was
- Europe: 111,
- Middle East: 23,
- Africa: 8,
- Asia: 48, and
- Oceania: 5
To increase global data collection, ESMO Co-Care also partnered with the CCC19 Consortium, which covers North America,
The Registry’s demographic data includes age, sex, place of residence, ethnicity, and nationality. Clinical history data includes prevalence of major comorbidities and the parameters defining a patient’s malignancy, including histology, stage, organ dysfunction, and molecular features. Antineoplastic therapies administered within two months from Covid-19 infection, including chemotherapy, immune check point inhibitors and targeted therapies, surgery, and radiotherapy are being recorded.
Profiles:
Leonard Y W Lee MD PhD., is an honorary research fellow of the Institute of Cancer and Genomic Studies of University Hospitals Birmingham and an executive lead of the UK Coronavirus Cancer Monitoring Project.
Richard L Schilsky MD, is executive vice president and chief medical officer of the American Society of Clinical Oncology (ASCO).
27.08.2020





