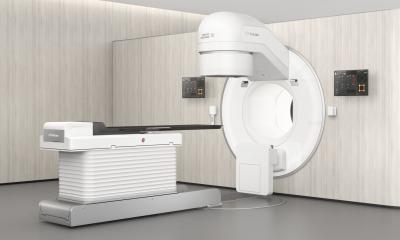
News • Radiation therapy
Call for action: Ensuring cancer treatment in times of COVID-19
The COVID-19 pandemic has affected virtually every aspect of healthcare provision - cancer care is no exception. In fact, during the pandemic, patients with cancer represent a high-risk group.
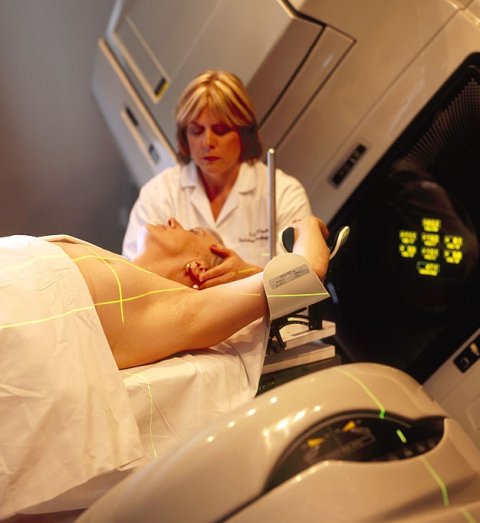
Image source: National Cancer Institute (NCI)/Rhoda Baer
Recent studies estimate that delays in cancer diagnosis and treatment will increase the indirect death toll1,2 of COVID-19 by several thousands in the coming years. Cancer care providers need to be able to provide less-demanding treatments, with less side effects and the potential for improved outcomes at lower costs. Radiation therapy is one of the few treatment modalities able to meet these demands.
Radiotherapy is required in the treatment of 50 percent of cancer patients and is involved in 40 percent of cancer cures3 but is often in the shadow of other treatments. Yet during the pandemic - with surgery, chemotherapy and immunotherapy often postponed or even cancelled - radiotherapy is becoming a preferred treatment option. Leading cancer institutions are reporting that radiotherapy has proved the most appropriate and safest treatment option during the COVID-19 pandemic.4
There are four reasons for prioritising radiotherapy for some cancer treatments:
- In contrast to most systemic therapies, the majority of radiotherapy regimens are only moderately immunosuppressive. This particularly applies to the so-called ‘hypofractionated’ radiotherapy schedules.5 (Hypofractionation means that the treatment can be delivered in fewer sessions.)
- As hypofractionation requires fewer sessions, patients’ total travel time for treatment is also significantly reduced.
- Radiotherapy does not usually compete for in-demand resources, such as respirators or intensive care unit beds. It is mostly conducted in an outpatient setting and can, and thus should, continue to be accessible.
- When clinically indicated and agreed with by the patient, radiotherapy can be used as an alternative to surgery.6
For the radiotherapy community, this pandemic must serve as a driver for the more rapid uptake of technology and techniques, enabling shorter treatments. Online practices such as remote treatment planning must be supported in order to deal with the current situation, to address the backlog of untreated patients and to be prepared for future crises.
Recommended article
Video • Coronavirus structured reporting
Radiology and COVID-19: How to establish safe workflows
Radiology experts from Norway and Germany highlighted the role of structured reporting in communicating clear results to the rest of the team, to improve patient and staff safety during the pandemic. They also related Germany’s experience of the crisis and what lies ahead in an online conference organized by the European Society of Radiology (ESR) last week.
To ensure that cancer patients have access to modern radiotherapy both during and after the pandemic, it is imperative that EU Member States strengthen their radiotherapy infrastructure. Even before the COVID-19 outbreak, more than one in four cancer patients in the EU did not receive the radiotherapy they needed.
There are several challenges to overcome:
- Many hospitals have reduced radiotherapy treatment and/or sent staff to support COVID-19 departments.
- There is a lack of personal protective equipment available for radiotherapy healthcare teams.
- The IT infrastructure can be inadequate and often cannot support remote planning and telemedicine.
- The radiotherapy infrastructure varies significantly across Europe.7 While we observe a clear lack of treatment systems in many south-eastern European countries, radiotherapy systems in western Europe show an average machine-age structure that renders them inadequate for use in sophisticated radiotherapeutic options. Further, a lack of brachy therapy applications limits access to high quality cancer care, particularly in gynaecological indications, which in turn reduces the overall options for cancer patients during this crisis.8
- According to an ESTRO-HERO publication in January 2020, virtually all current reimbursement systems in the EU Member States were established around 20 years ago. This is why most of them fail to offer reimbursement opportunities for modern forms of radiotherapy. As a result, treatments with more sophisticated, up-to-date technologies are not reimbursed appropriately. This, along with a lack of funding for the required capital investments, is hindering any uptake of innovative radiotherapy technologies in the EU.9
- Radiotherapy involves multidisciplinary teams (radiation oncologists, medical physicists, radiotherapy technologists, dosimetrists). We are currently observing severe shortages in this workforce, which in part is related to education and training. In addition, while technological solutions can help make processes more efficient, their uptake is being impeded by a lack of reimbursement.10
Recommended article
News • Coronavirus collaterals
COVID-19 could cause 20% rise in cancer deaths
The COVID-19 pandemic could, over the next year, lead to a 20% rise in the number of deaths from people who have been newly diagnosed with cancer, according to research supported by DATA-CAN. The analysis is the first to focus on the impact of the emergency on mortality rates in people with cancer and uses data from the health records of over 3.5 million patients in England.
COCIR urges the European Commission and national governments to acknowledge the importance of radiotherapy, particularly during these times of COVID-19. As the European Commission is currently developing “Europe’s Beating Cancer Plan”, it is important that this plan - and those of Member States - address this inequality of patient access to radiotherapy. This applies both to the availability of access to radiotherapy overall and to the modern equipment needed to deliver the newest treatments. With the focus on ensuring that cancer patients and their needs are not left behind, it is now time to radically rethink priorities and increase investment in modernising radiotherapy capabilities.
The first short-term action must be to ensure that radiotherapy departments return to full capacity working and receive the required support to be able to do so. However, many of the challenges will require long-term sustainable solutions; to achieve these before it’s too late, it is essential to start immediately. To provide effective solutions, COCIR recommends that the relevant EU and Member State institutions should:
- Ensure the availability of personal protective equipment for radiotherapy teams.11
- Enhance the general IT infrastructure: Health care professionals need to be able to access hospital networks via their personal computers. This flexibility is essential for healthcare providers and for optimising patient safety.
- Allow remote services: Most radiotherapy systems offer the ability to enable healthcare professionals to plan treatments remotely from home without compromising confidential patient information.
- Increase access and modernise radiotherapy infrastructures:
▪ EU funds should be used to increase access to radiotherapy and to replace ageing machines that may not be able to take advantage of advanced techniques.
▪ Horizon Europe should ensure incentives for industry and researchers to further facilitate development of radiation therapy technologies.
▪ National Reimbursement systems must be revised to maximise the potential of currently-available technologies, in a way that adequately reflects the complexity of treatment, required expertise and resource utilisation. They should offer incentives to facilitate the uptake of new and innovative radiation therapy technologies and techniques.12 - Establish a pan-European multistakeholder platform (policy makers, manufacturers, patients, clinicians, academics and the scientific community) to allow for the regular exchange of best practices related to cancer radiotherapy treatment. This will ensure that there are sufficient medical professionals available to maximise the potential offered by radiation therapy technologies.
- Improve patients’ awareness of these life-saving technologies such as radiotherapy and change some of the existing negative perceptions surrounding the treatment.
References:
1 Alvina Lai, Laura Pasea, Amitava Banerjee, Spiros Denaxas et All: Estimating excess mortality in people with cancer and multimorbidity in the COVID-19 emergency
3 Marie Curie Legacy Campaign white paper
4 Dai M-Y, Liu D, Liu M, Zhou F-X, Li G-L, Chen Z, et al. Patients with Cancer Appear More Vulnerable to SARS-CoV-2: A Multi-Center Study During the COVID-19 Outbreak.
5 Wild, A. T. et al. Lymphocyte- sparing effect of stereotactic body radiation therapy in patients with unresectable pancreatic cancer. Int. J. Radiat. Oncol. Biol. Phys. 94, 571–579 (2016).
6 Marie Curie Legacy Campaign white paper
7 COCIR “RT Age Profile 2019” Report
8 For example, use of brachytherapy, despite being a cost-effective treatment with proven benefits for patients, has been on the decline in the past years in the EU. The main reasons are related to challenges in the education of radiation oncologists and the necessity to ensure adequate reimbursement systems for the use of this technology. J. Fricker, ‘Brachytherapy: halting the spiral of decline.’, Cancer World, 17 March 2019.
10 Yolande Lievens, Josep M. Borras, Cai Grau: Provision and use of radiotherapy in Europe. doi:10.1002/1878-0261.12690
11 Action Radiotherapy Flash Survey 24-27th April 2020
12 iPAAC WP 8 Report: Tackling reimbursement for radiation oncology and cancer surgery: challenges and options (expected in 2020)
04.06.2020