
Credit: Ember et al., doi 10.1117/1.JBO.27.2.025002
News • Machine learning
Using Raman spectroscopy and AI for SARS-CoV-2 detection
Researchers in Canada have developed a noninvasive and reagent-free technique for the efficient detection of COVID-19.
The novel coronavirus, or SARS-CoV-2, which causes the highly contagious COVID-19, has infected millions of people worldwide. The global spread of this deadly pandemic has triggered widespread research on infection control. However, controlling the spread of COVID-19 is challenging for many reasons.
Some patients show a variety of nonspecific symptoms ranging from headaches to a cough. However, many patients with COVID-19 remain symptom-free even after getting infected, but still may have the potential to infect others. This makes initial triage and diagnosis difficult. And while reverse transcription polymerase chain reaction (RT-PCR) techniques are currently the gold standard, they have certain limitations.
RT-PCR involves the transportation of samples to a clinical laboratory for testing, which poses logistical difficulties. It also requires the use of reagents, which could be in short supply and may be less effective when the virus mutates. Moreover, RT-PCR tests can be time-consuming and less sensitive in asymptomatic individuals, rendering them unfeasible for widespread rapid screening.
Thus, biomedical researchers are trying to devise novel methods for better detection of COVID-19 infections in point-of-care settings, without the need to send away samples for testing. Recently, researchers from Canada developed one such technique using saliva samples. Unlike nasopharyngeal swabs, saliva sampling is safer and noninvasive. In their article published in the Journal of Biomedical Optics, they describe a new reagent-free detection technique that is based on machine learning (ML) and laser-based Raman spectroscopy.
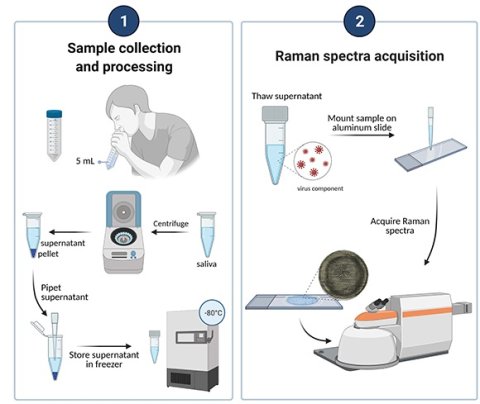
Raman spectroscopy is routinely used by researchers to determine the molecular composition of samples. Put simply, molecules scatter incident photons (particles of light) in a unique manner that is dependent on underlying chemical structures and bonding. Researchers can sense and identify molecules based on their characteristic Raman "fingerprint" or spectrum, which is obtained by shining light at samples and measuring the scattered light.
COVID-19 can cause chemical changes in the composition of saliva. Based on this knowledge, the research team analyzed 33 COVID-19-positive samples clinically matched with a subset of a total 513 COVID-19-negative saliva samples collected from the Pointe-Saint-Charles COVID-19 testing clinic in Quebec, Canada. The Raman spectra they obtained were then trained on multiple-instance learning models, instead of conventional ones.
Senior author Frédéric Leblond, with appointments at Polytechnique Montréal, Centre de recherche du Centre hospitalier de l'Université de Montréal, and Institut du cancer de Montréal, Canada, explains this more simply: "Our machine learning method uses information from each individual Raman spectrum. It does not use averaged data, and so it can integrate more information from the saliva samples to give a highly accurate output."
The results from this method indicate an accuracy of about 80 percent, and the researchers found that taking sex at birth into consideration was important in achieving this accuracy. Although saliva composition is affected by time of day as well as the age of the test subject and other underlying health conditions, this technique can still prove to be a great candidate for real-world COVID-19 detection.
Katherine Ember, a postdoctoral researcher at Polytechnique Montréal, Canada, and first author of the study, sums up, "Our label-free approach overcomes many limitations of RT-PCR testing. We are working to commercialize this as a faster, robust, and low-cost system, with potentially higher accuracy. This could be easily integrated with current viral detection workflows, adapted to new viruses and bacterial infections, as well as accounting for confounding variables through new machine learning approaches. In parallel, we are working on reducing the testing time further by using nanostructured metallic surfaces for containing the saliva sample."
These findings can facilitate better COVID-19 detection in addition to paving the way for new tools for other infectious diseases.
Source: SPIE--International Society for Optics and Photonics
10.02.2022





