News • Replicas from the lab
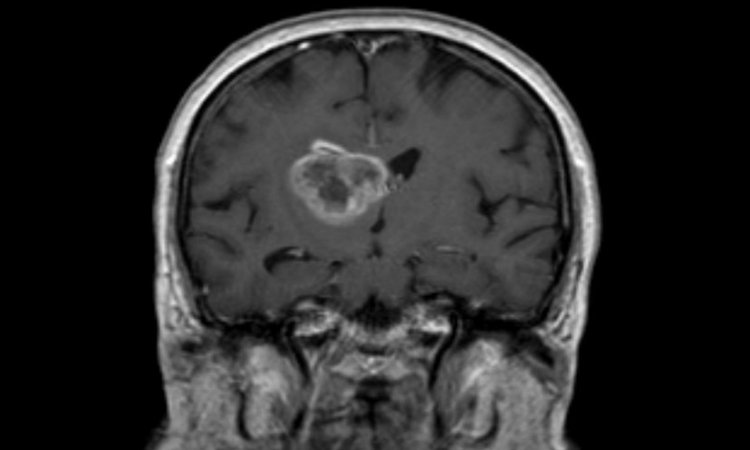
Growing 'mini tumours' to personalise drug treatment
Testing cancer drugs on miniature replicas of a patient’s tumour could help doctors tell in advance which treatments will work, a major new study reports.
The exciting new technique involves growing ‘mini tumours’ from biopsy samples – and could help end reliance on trial and error in selecting cancer treatments for patients where genetic tests are not predictive of response. Researchers at The Institute of Cancer Research, London, and The Royal Marsden NHS Foundation Trust found testing mini tumours predicted whether a drug would work between 88 per cent and 100 per cent of the time. They believe each patient could have mini tumours grown up and tested for drug sensitivity before starting treatment – allowing doctors to design them a personalised treatment regimen. The new research was carried out in bowel, stomach and other digestive system cancers, and is published in the prestigious journalScience. It was supported by the NIHR Biomedical Research Centre at The Royal Marsden and The Institute of Cancer Research (ICR), and Cancer Research UK.
96% similarity between lab-grown and original tumour
Researchers at the ICR and The Royal Marsden took biopsy samples from 71 patients with advanced bowel, gastro-oesophageal or bile duct cancers, whose tumours had spread (or metastasised) round the body, and who were enrolled in early-stage clinical trials. They took cells from these biopsy samples – taken before and after treatment from metastatic sites once the disease had progressed – and placed them inside a gel so they were free to form a 3D shape. They tested 55 established or new drugs against the mini tumours and compared the results with how the patient had responded in the clinic. Testing mini tumours was 100 per cent accurate at identifying drugs that wouldn’t work in patients, and picked out drugs that would shrink a patient’s tumour 88 per cent of the time.
Mini tumours seemed more effective at predicting drug response than analysing the DNA code of the patient’s tumour alone – with instances where a patient had been expected to respond based on the tumour’s DNA sequence, but where the mini tumour correctly predicted that they would not. Looking under the microscope, the mini tumours had a strikingly similar mix of different cell types as their parent tumours, and in depth genetic analysis showed the replicas also had the same pattern of genetic changes as those in patients. Across all the patients, the original tumours and lab-grown mini tumours were found to be 96 per cent identical across 151 cancer-related genes – with very few new mutations since being grown in a dish. This is crucial since new mutations can change the way the tumour responds to drugs.
Mini tumours grown in dishes couldn’t be used to test treatments that work by targeting the environment around the tumour, such as the drug regorafinib which restricts blood supply to the tumour. But the researchers found that when they transplanted the mini tumours into mice they then responded to treatment, and evolved over time, in the same way as the patient’s cancer.
We were able to look in incredible detail at how tumours responded to drugs
Nicola Valeri
Study leader Dr Nicola Valeri, Team Leader in Gastrointestinal Cancer Biology and Genomics at The Institute of Cancer Research, London, and a Consultant Medical Oncologist at The Royal Marsden NHS Foundation Trust, said: “Once a cancer has spread round the body and stopped responding to standard treatments, we face a race against time to find patients a drug that might slow the cancer’s progression and extend their lives. We found that recreating patients’ tumours in the laboratory using this new technique gave us an extremely promising way to predict whether a drug would work for a patient. We were able to look in incredible detail at how tumours responded to drugs – including patterns of gene activity and mutation, and even how the cancer would evolve in response to treatment. We looked at tumours from patients with cancers of the digestive system, but the technique could be applied to a wide variety of cancer types. We need to further evaluate its potential in larger clinical studies, but it has the potential to help deliver truly personalised treatment – and avoid the reliance on trial and error for many patients when clinicians give them a new cancer drug.”
Study co-author Professor Paul Workman, Chief Executive of The Institute of Cancer Research, London, said: “Cancers are highly complex and constantly adapting and evolving – so it is extremely difficult for doctors to know whether a particular drug will work for the patient on front of them. This study has shown that testing drugs on replica tumours before they are given to patients is not only possible, but predicts how a patient will respond more accurately than simply looking at the cancer’s DNA. It could predict whether a cancer will be drug resistant before a person ever receives the treatment – which is especially important for those with advanced cancers where time is so precious. The potential of mini tumours doesn’t stop there. Having a better model for how cancers may respond to treatment could help accelerate drug discovery and even reduce reliance on animal experiments.”
Study co-author Professor David Cunningham, Director of the NIHR Biomedical Research Centre at The Royal Marsden NHS Foundation Trust and The Institute of Cancer Research, London, said: “Tackling the unpredictable nature of cancer is one of the major challenges that we hope to overcome in cancer research. The same type of cancer can differ between patients, and can also adapt and evolve within that same patient and then in response to treatment. This promising research moves us forward in the field of personalised medicine, and should ultimately lead to smarter, kinder and more effective treatments for patients.”
Professor Charles Swanton, Cancer Research UK’s Chief Clinician, said: “This interesting research provides promising evidence that testing treatments on mini-replicas of a patient’s tumour could help guide the development of new drugs. This is important because predicting how effective treatments such as chemotherapy will be for an individual patient can be difficult, with very few accurate tests available for doctors. This new approach could help us test future targeted therapies before trialling them in the clinic.”
Source: The Institute of Cancer Research
26.02.2018