Towards customised treatment of breast cancer
Breast cancer can develop very differently in different women. Researchers in Norway are improving breast cancer diagnostics and treatment by identifying the various tumour types. The objective is to find out as much as possible about the various tumour types so that each patient can receive precisely the right treatment at the right time.
Women respond differently to available treatments. At Oslo University Hospital and the Norwegian University of Science and Technology (NTNU) in Trondheim, researchers are capturing the complexities of breast cancer tumours. Their projects receive funding under the Research Council’s National Programme for Research in Functional Genomics in Norway (FUGE).
Breast cancer is the most common type of cancer in women. This extremely complex disease is attacking more and more women, and both the way it develops and its outcome can vary greatly from case to case.
Women also respond differently to available treatments. At Oslo University Hospital and the Norwegian University of Science and Technology (NTNU) in Trondheim, researchers are capturing the complexities of breast cancer tumours. Their projects receive funding under the Research Council’s National Programme for Research in Functional Genomics in Norway (FUGE).
Different tumours, same treatment
“For breast cancer patients, we currently have only a few different treatment principles from which to choose,” explains Professor Gunhild M. Mælandsmo. “This means that many patients receive the same treatment even though their tumours may be very different. Our objective is to find out as much as possible about the various tumour types so that each patient can receive precisely the right treatment at the right time. There are still many people who die from breast cancer – which plainly shows we are not yet able to treat everyone effectively.”
“One of our objectives is to figure out how to identify the patients with the most serious prognoses,” says Professor Ingrid Gribbestad. “Can we tell, for example, from the molecular structure of the tumours? If so, then new medicines that are particularly effective against certain structures can be developed.”
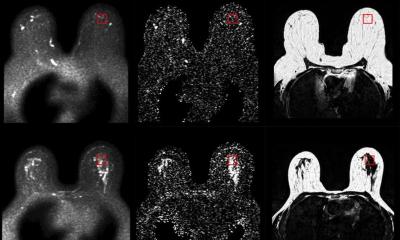
Professor Gribbestad heads a breast cancer research project in Trondheim, while Professor Mælandsmo and Therese Sørlie are heading projects in Oslo. They have all entered into a cooperation agreement in order to make use of each other’s methods and findings. Whereas the Trondheim researchers are using magnetic resonance (MR) tomography to characterise tumours, the Oslo researchers are focusing on molecular changes. MR is a medical imaging technique for detailed visualisation of internal human and animal tissue.
Testing on animal models
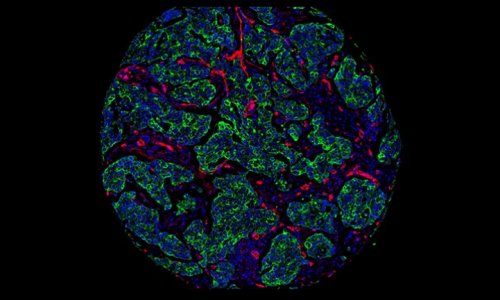
“Cancer develops when the genes in a cell are damaged,” explains Professor Anne-Lise Børresen-Dale, who works on the project with Professor Sørlie. “This is why research on genetic material is so crucial for our understanding of cancers.”
The Oslo researchers study the genetic background of breast cancer patients as well as the DNA, RNA and proteins of their tumours. Then, for comparison, they test out various treatments on animals that have received implanted tumours with various genetic profiles and severity from the patients. After some treatment time, the animal subjects are shipped to Trondheim, where they undergo MR scanning.
“We can see whether the MR signals are different for genetically different tumours,” adds Professor Gribbestad, “and if so, whether there are any distinctive characteristics to use when we analyse patients’ MR images. Certain characteristics, for instance, may suggest that the patient’s tumour is especially difficult to treat.”
Up to 15 subtypes
Professor Gribbestad and her colleagues have also developed a new method called metabolomics. A specialised magnetic resonance machine enables them to study biochemical processes of patients’ tissue samples. Do different processes occur in a benign tumour compared to a malignant one?
“By identifying these biochemical processes,” says Professor Gribbestad, “we may be able to develop medicines that can stop the processes that lead to harmful progression in certain breast cancer patients. This method is unique in that it allows us to quickly identify the processes without destroying the tumour tissue, so that the tissue can be used again in future studies.”
In 2000 the scientific journal Nature presented the work of Sørlie and Børresen-Dale in identifying five subtypes of breast cancer. The researchers believe, moreover, that once they refine their identification of tumours in individual patients, they may discover that there are as many as 15 subtypes.
New treatment principles
The goal is customised treatments targeted at each tumour subtype. Current treatment alternatives include surgery, chemotherapy, radiation, and hormonal (anti-oestrogen) therapy. The researchers are seeking new treatment possibilities through activities such as patient trials to test the antibody drug Avastin.
Avastin is designed to choke off the blood supply to a tumour by blocking the formation of new blood vessels. Women with locally advanced breast cancer who are undergoing treatment at Oslo University Hospital are now offered chemotherapy in combination with Avastin. Samples of their tissue, blood and bone marrow are collected for future analysis.
“We intend to find out which kinds of proteins and genes are expressed in the patients who respond to treatment versus those who don’t,” says Professor Mælandsmo. “This would enable us to customise Avastin treatment based on a patient’s genetic profile.”
“Large-scale studies on this type of treatment are underway,” says Professor Børresen-Dale, “but they are not doing molecular profiles. So they may determine that a substance works, but not for whom and why.”
01.03.2011