Source: German Roentgen Society/Vogel-Claussen
Article • Chest specialists
COVID-19 imaging: radiologists share practical advice
As radiologists worldwide continue to share their knowledge of COVID-19 to help fight the pandemic, two chest experts from France and Spain talked about their country perspectives and the practical experience at their hospital in a dedicated online session organized by the European Society of Radiology (ESR).
Report: Mélisande Rouger
A French radiography
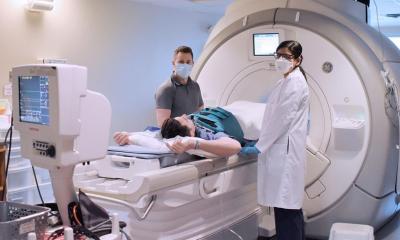
Marie-Pierre Revel, a professor of radiology and chest radiologist at Cochin Hospital in Paris, presented France’s experience in relation to practical imaging equipment issues and addressed considerations on how to maintain radiology services for non-COVID-19 patients during the ESR Connect Special Report.
Talking about her experience at Cochin Hospital, Revel insisted on the importance of being efficient and minimizing contamination risk during the pandemic. “To face this situation, we try to be as efficient as possible and minimize cross-contamination risks for non- COVID patients and for staff,” she said.
As of April 8th, Cochin Hospital had treated around 500 COVID patients since the beginning of the pandemic and had around 100 currently hospitalized patients, with nearly 70 in the ICU. The number of beds in this unit has tripled over the past weeks, and that increase has been reflected in a major increase in bedside chest x-ray examinations. “These patients are very unstable, it is not possible to send them to the CT unit. We had to talk to our CT colleagues to avoid bedside chest x-ray being systematically prescribed and reduce their use. Last weekend, we performed 63 such scans, as opposed to 150 the week before,” she said.
Revel and her colleagues have dedicated mobile x-ray machines that are located in each ICU. She said it is important to optimize this number because of the time required to perform the examination, which usually takes 20 minutes. “We had to double the number of technologists for this task and organized for them to go to the ICU at fixed times, twice a day,” she said.
Cochin Hospital consists of several buildings, with six different ICUs and dedicated CT equipment that is located close to the emergency room for Covid-19 patients - either suspected or confirmed. “We avoid mixing different categories of patients. That allows us to concentrate the protective equipment to a single location,” she said.
The team also has a dedicated phone line, to avoid waiting time before and after the CT acquisition, with an accompanying staff who wait until the examination is completed.
Revel recommends having just one technologist in the room close to the patient. “We have reasonable activity in our emergency room - only 90 patients per day. Of these, only those with respiratory symptoms are sent for CT. Very severe patients are hospitalized anyway and when they are unstable they don't have a CT examination,” she explained.
Recommended article
Interview • Chest X-ray, CT and more
Imaging the coronavirus disease COVID-19
Chest X-ray is the first imaging method to diagnose COVID-19 coronavirus infection in Spain, but in the light of new evidence this may change soon, according to Milagros Martí de Gracia, Vice President of the Spanish Society of Radiology (SERAM) and head of the emergency radiology unit at La Paz Hospital in Madrid, one of the hot spots for viral re-production of COVID-19.
One reason for having so few patients in the emergency room is because France recommended patients with few symptoms to stay at home. Some apps (Covidom) and websites (Maladiecoronavirus.fr) have been launched that allow self-surveillance, reporting and advice.
Another key point, she added, is to maintain radiology services for non- COVID patients and prioritize oncology and other emergencies. At Cochin Hospital, this activity is performed in other CT units. “For the coming weeks, we have kept all radiological examination requests related to initial staging, follow-up treatment and suspicion of recurrence. But we decided to postpone things like systematic evaluation after remission. We have kept all procedures related to oncology, and have a dedicated phone line for emergencies other than COVID,” she said.
Regarding staff organization, secretaries and radiologists are allowed to work remotely to limit the number of persons on-site. All connections were activated rapidly, with procedures sent to staff members. Multidisciplinary meetings have been maintained, both online for the internal medical department and face-to-face for thoracic oncology and general oncology.
Recommended article

News • Coping with Covid-19
How France handles the coronavirus pandemic
The first case of the new coronavirus infection was reported on the 24th January. The strategy taken by the French to stem the spread of the virus and relieve the pressure on the health service may seem draconian to some, but many feel that it is either not strong enough and/or too long in coming because it is only recently that the borders have finally been closed.
The Spanish view
Marcelo Sanchez Gonzalez, a professor of radiology and chest radiologist at Clinic Hospital in Barcelona, also shared his experience in Spain, one of the countries most hit by the pandemic.
As of April 8th, 945 in-patients had been admitted in different facilities of Clinic Hospital, and the number of COVID patients had been increasing weekly. 98 patients were in the ICU and 25 in intermediate care as Sanchez gave his talk.
The recommendations issued by the Spanish Society of Radiology (SERAM) mention the importance of imaging COVID patients with chest x-ray. At Clinic Hospital, these are performed with mobile equipment at bedside and three new mobile machines have been acquired to cover the rising needs, Sanchez explained. “We have had to increase the number of technologists to perform mobile x-ray acquisitions and the number of radiologists reporting those studies. Today, radiologists from every section are reporting chest x-ray films,” he said.
Clinic Hospital has allocated specific equipment, including CT, MRI and ultrasound, exclusively for COVID patients. The team uses specific chest x-ray equipment for COVID outpatients coming from primary care and who are hospitalized at home.
The number of portable radiographs has increased significantly, with up to 180 x-ray scans performed per day, while the number of non-portable chest x-rays, mainly from emergency departments, has been decreasing over the past few days.
Radiologists at Clinic Hospital perform CT in patients with a clinical suspicion, negative CPR or negative or inconclusive x-ray, but also to evaluate torpid cause of disease or rule out pulmonary embolism. “We have a high incidence of pulmonary embolism, which affects 30% of patients in the first 100 CT angiograms. Besides, we perform CT in case of urgent surgery that cannot be delayed and when PCR is not available,” he said.
Sanchez and his colleagues have reduced their regular workload by 70-80%, depending on the area, and postponed scheduled studies until April 30th. All requests are reviewed to decide whether they should be maintained or rescheduled, and are ranked with a three-level priority scale. Oncological patients; non-delayable studies based on clinical criteria; emergency patients; and other interventional procedures that cannot be delayed are maintained.
As a consequence, the hospital has registered a significant decrease in the emergency department of non-Covid patients, including trauma, stroke and cardiac patients, as many other institutions across Spain. Much of the service is working remotely and all multidisciplinary meetings are held remotely.
Recommended article

Article • Corona consequences in Spain
COVID-19 fears put interventional cardiology on lockdown
The number of primary angioplasties – the main treatment for heart attack – has dropped by 40% in Spain since the beginning of the coronavirus lockdown. Other key diagnostic and therapeutic procedures have also considerably diminished. Spanish cardiologists are urging the population to call the emergency medical systems whenever symptoms of myocardial infarction occur, in spite of fears…
Inside the radiology department, the personnel are segregated to minimize risks of transmission, he explained. “We have created four independent, separate groups to cover the emergency service, and have increased the staff in this service from three to four radiologists on-site. In each section, one radiologist is working on-site per day and the rest of the staff is working from home. For vascular and interventional procedures, we have created segregated groups of radiologists to avoid contact and contamination, so if one group becomes contaminated, the other can carry out its functions. We also segregate technologists and nurses for CT, MRI and ultrasound, with a weekly rotation,” he explained.
Regarding protection, Sanchez advised, that all patients in the radiology department must wear a mask and technologists wear a surgical or FFP2 mask. CT equipment used for non-Co COVID vid patients should be cleaned every hour with sodium hypochlorite solution, while CT equipment used for COVID imaging should be cleaned after each patient. The protection protocol is the same for stroke patients treated in the interventional suite.
16.04.2020