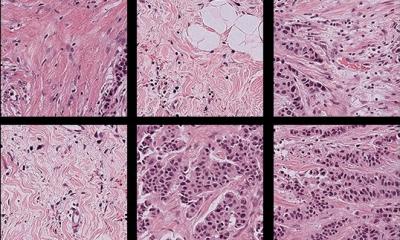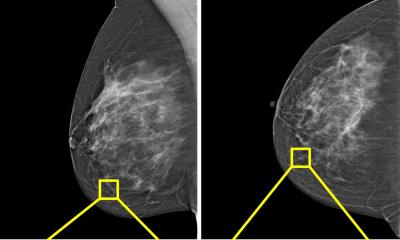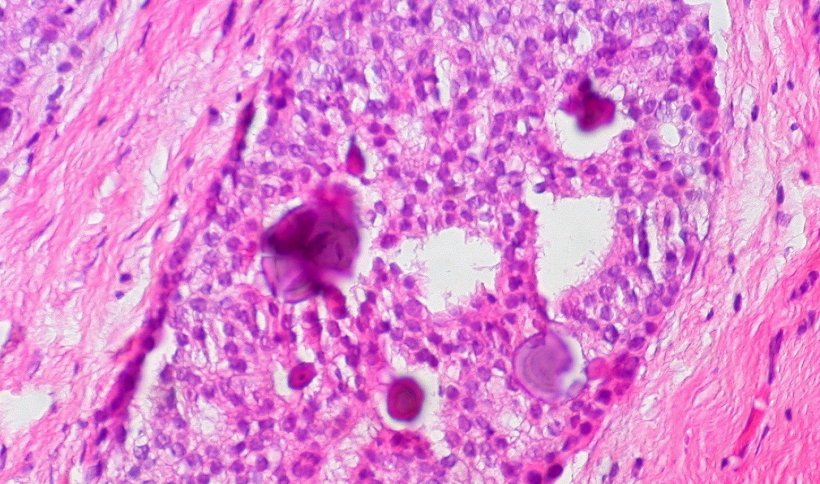
Image source: Ed Uthman from Houston, TX, USA, Breast Ductal Carcinoma in Situ With Calcifications (5436471236), CC BY 2.0
News • Histological grading assistance
AI improves precision in breast cancer diagnosis
Researchers at Karolinska Institutet have developed an AI-based tool that improves the diagnosis of breast cancer tumours and the ability to predict the risk of recurrence.
The greater diagnostic precision can lead to more personalised treatment for the large group of breast cancer patients with intermediate risk tumours. The results are published in the scientific journal Annals of Oncology.
Every year, around two million women globally develop breast cancer. In the diagnostic procedure, tissue samples of the tumour are analysed and graded by a pathologist and categorised by risk as low (grade 1), medium (grade 2) or high (grade 3). This helps the doctor determine the most suitable treatment for the patient.

Image source: Karolinska Institutet/Photo: Stefan Zimmerman
“Roughly half of breast cancer patients have a grade 2 tumour, which unfortunately gives no clear guidance on how the patient is to be treated,” says the study’s first author Yinxi Wang, doctoral student at the Department of Medical Epidemiology and Biostatistics, Karolinska Institutet. “Consequently, some of the patients are over-treated with chemotherapy while others risk being under-treated. It’s this problem that we’ve tried to resolve.”
Hospitals have recently started to make limited use of molecular diagnostics to improve the precision of breast cancer risk assessment, but these methods are often costly and time-consuming. The researchers at Karolinska Institutet have now developed and evaluated an AI (artificial intelligence)-based method for tissue analysis. The study shows that the AI-based method can further divide the patients with grade 2 tumours into two sub-groups, one high-risk and one low-risk, that are clearly distinguishable in terms of the recurrence risk.

Image source: Karolinska Institutet/Photo: Stefan Zimmerman
“One big advantage of the method is that it’s cost-effective and fast, since it’s based on microscope images of dyed tissue samples, which is already part of hospital procedure,” says co-last author Johan Hartman, professor of pathology at the Department of Oncology-Pathology, Karolinska Institutet, and pathologist at the Karolinska University Hospital. “It enables us to offer this type of diagnosis to more people and improves our ability to give the right treatment to any one patient.”
The AI model has been trained to recognise characteristics of high-resolution microscopic images from patients classified with grade 1 and grade 3 tumours. The study is based on an extensive microscopic image bank of 2,800 tumours.

Image source: Karolinska Institutet/Photo: Stefan Zimmerman
“It’s fantastic that deep learning can help us develop models that don’t just reproduce what specialist doctors do today, but also enable us to extract information beyond the scope of the human eye,” says co-last author Mattias Rantalainen, associate professor and research group leader at the Department of Medical Epidemiology and Biostatistics, Karolinska Institutet.
The method is not yet ready for clinical application, but a regulatorily approved product is under development by a newly started company, Stratipath AB, which is supported by KI Innovations. The researchers will now be further evaluating the method with the aim to have a product out on the market by 2022.
The study was financed by the Swedish Research Council, the Swedish Cancer Society, Karolinska Institutet, ERA PerMed, the European Research Council, MedTechLabs, Swedish e-science Research Centre (SeRC), Region Stockholm, the Cancer Society in Stockholm and the Swedish Breast Cancer Association.
Source: Karolinska Institutet
01.10.2021