Article • Neurology
The 3-D printed brain tumour
3-D printed tumour-like constructs will be used by a research team at Scotland’s Heriot-Watt University in Edinburgh, to raise research to a new level and successfully lead to new treatment options.
Report: Mark Nicholls
The project brings together tumour biologist Dr Nick Leslie, at Heriot-Watt University’s Institute of Biological Chemistry, Biophysics and Bioengineering, with 3-D printing expert Dr Will Shu as well as neuropathologists and neurosurgeons, engineers and clinicians.
The collaborators have developed several types of ‘brain tumour in a lab’ to study such tumours and test drugs to treat them. This has included taking brain tumour stem cells from patients, but they point out that if these cells are simply lab grown they behave very differently from how they do in a real tumour – because cell behaviour depends on its environment and the same tumour-like environments cannot be created in a lab, yet.
New research methods
With a key focus on malignant tumours, specifically glioblastoma the interdisciplinary team intends to apply the novel 3-D bio-printing technology to produce more realistic models for drug testing and research into glioma biology, whereas previously they used preclinical animal models with poor relationship to human brain tumour pathology.
Leslie explains: ‘We have two main goals: to reproduce constructs for drug testing and to reach a resolution from the 3-D technique that is good enough so that we can start to do more detailed studies of the tumour micro environment.
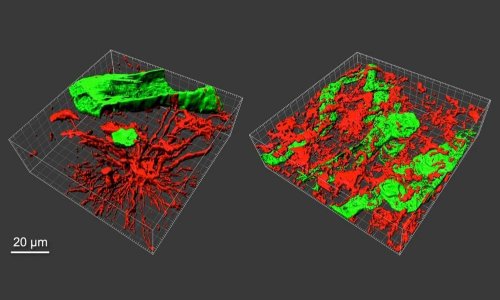
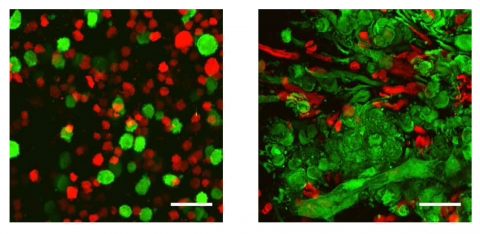
What the Heriot-Watt researchers have done is printed 3-D brain tumour (glioma) stem cells and other cell types isolated from patients’ brain tumours, using their own novel technique. This recreates tumour-like constructs with a dense mixture of matrix proteins and diverse neighbouring cells, which will continue to grow rapidly as tumours do in real life.

‘We hope to be able to provide brain tumour models for experiments that will give closer results to a real human setting and will, within 5-10 years, see drugs tested using these models in a way that will hopefully help weed out problems before they reach animal or human trials.’
* The Brain Tumour Charity, in the United Kingdom, funds malignant brain tumour research.
More than 10,600 people are diagnosed with a brain tumour annually in this country, the charity reports, and the survival prognosis is low – around 5,000 of them die every year.
Profile:
Dr Nick Leslie is Associate Professor at the Institute of Biological Chemistry, Biophysics and Bioengineering at Heriot-Watt University in Edinburgh and runs a laboratory studying how cells regulate their behaviour and how this regulation fails in cancer. His group has particularly investigated the tumour suppressor protein PTEN and why the loss of PTEN function is a common step in the development of many cancers. Having studied for a first degree in Genetics at Cambridge University, he obtained his PhD at Glasgow University.
13.11.2016