Article • Detecting bladder tumours
Photodynamic diagnosis locates the smallest tumours
Bladder cancer (BC) is the most common malignancy involving the urinary system and the ninth most common malignancy worldwide.
Report: Anja Behringer
About one in 25 western men (the seventh most common cancer) and one in 80 women (17th position) will be diagnosed some time in life. Transitional cell or urothelial carcinoma is the most common type of BC, accounting for more than 90% of all cases. Urothelial carcinomas are clinically classified as non-muscle-invasive (NMIBC) and muscle-invasive bladder cancer (MIBC). NMIBC is confined to the bladder mucosa and submucosa and has not infiltrated the muscular wall. 70% of BC cases are NMIBC at diagnosis. NMIBC includes the subtypes Ta (70%), T1 (20%) and CIS (10%). MIBC has invaded the muscular wall of the bladder and/or spread to nearby organs and/or lymph nodes. 30% of BC cases are MIBC at diagnosis (T2 to T4).
Prevalence and mortality
The worldwide age-standardised incidence rate (ASR) is 10.1 per 100,000 for males and 2.5 per 100,000 for females. The prevalence of bladder cancer is the highest of all urological malignancies. Each year, approximately 110,500 men and 70,000 women are diagnosed with new cases and 38,200 patients in the European Union and 17,000 US patients die from BC. Therefore, the economic impact is important, because it is among the most expensive cancers to manage. The total cost has recently been estimated to be €4.9 billion in 2012, with healthcare accounting for €2.9 billion (59%) and representing 5% of the total cancer-related healthcare costs across the EU (Leal et al., Eur Urol. 2015). The management of early stage bladder cancer therefore represents a potential target for major healthcare savings. The risk of developing bladder cancer increases with age and the median age at diagnosis is 70 years. Women are diagnosed less often than men, but tend to have more advanced disease at diagnosis because bladder cancer is less often suspected. The main symptom for NMIBC is painless haematuria. In patients with CIS, haematuria may be accompanied by irritative voiding symptoms such as urinary frequency, urgency, and dysuria. Physical examination does not reveal NMIBC.
The diagnosis of bladder cancer is made by cystoscopic examination of the bladder including biopsy (an invasive examination method) and histological evaluation of the resected tissue. Urine cytology is a non-invasive method for detecting bladder cancer by identifying abnormal urothelial cells in the voided urine or bladder washes. Although urine cytology remains the gold standard test, many new urinary biomarkers have been identified in recent years. Imaging examinations include conventional intravenous or computed tomography urography (X-ray examination with contrast agent) and ultrasound (can show tissue changes, tumours, hydronephrosis).
A transurethral resection (TURB) is the standard treatment for bladder tumours. The aim of the initial TURB is to remove all visible tumours and obtain tissue for accurate histological diagnosis. An important factor that influences the outcome of the initial TURB is the visibility of tumours. Hexaminolevulinate hydrochloride (HAL)-guided blue-light cystoscopy improves visualisation of tumours during TURB, helps the urologist to identify tumour margins and confirms complete clearance of lesions. The guidelines recommend the use of fluorescence-guided resection as being more sensitive than conventional white-light cystoscopy to detect tumours.
Optimised photodynamic diagnosis

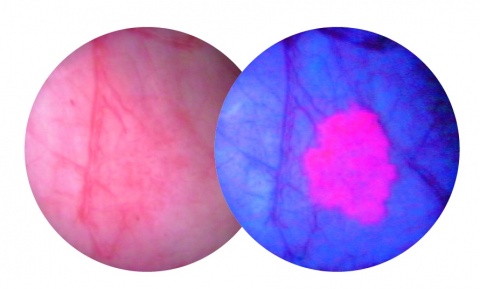
At the 31st Annual Congress of the European Association of Urology Professor Thorsten Bach of the Asklepios Hospital in Hamburg reported on his experiences with PDD (photodynamic diagnosis)-assisted cystoscopy using Hexvix (HAL). ‘The malicious thing with bladder cancer is the high risk of recurrences. Therefore, it’s so important to remove even the smallest tumours without lesions, as in between a third to half of all cases, new ones occur after six weeks.’
To detect them more reliably and at an earlier stage than is possible with the conventional white light cystoscopy the photoactive, fluorescent substance Hexvix colours existing tumours pink, against a blue background. ‘This allows the discovery of 7% more tumours as proven by a study from Denmark and real-life experience from the UK last year.’ When EH asked about the costs involved, Bach explained that Hexvix has been covered by the DRG system since 2014. ‘The additional costs pay off through reduced costs spent on intervention, as proven by the Danish study.’ The improved pharmacokinetic characteristics of the only currently licensed medication for PDD have been described in the new S3 guideline on bladder cancer, published in May.
Profile:
Professor Thorsten Bach heads the Department of Urology at the Asklepios Hospital, Harburg, in Hamburg. In 2008, he was a Fellow of the Endourological Society, specialising in endourology and minimally invasive urology. Laser enucleation of the prostate, among others, is another specialty, utilising a Thulium laser – he has performed and published the fundamental research on this laser tool, which have gained him national and international awards. He is a member of the German Working Group on Urolithiasis as well as the EAU Section of Urolithiasis (EULIS) and EAU Section of Urotechnology (ESUT), and also a member of the EAU Guideline panel on Male LUTS, plus a Chairman for the EAU Patient Information Project (http://patients.uroweb.org/).
06.11.2016