Article • The interdisciplinary challenge
Evaluating ICU care for cancer patients
Progressive treatments offer new chances for cancer patients, but also could result in as yet unknown complications. The number of cancer patients transferred to the ICU for cancer-specific and internal medicine related reasons is on the increase.
Caring for them on the ICU is a complex challenge, with interdisciplinary cooperation playing an essential part. Certain criteria need to be met for the admission of a cancer patient to the ICU, according to Dr Peter Schellongowski, specialist in internal medicine and intensive care specialist and senior consultant in the ICU at Vienna’s Medical University. The Austrian ICU specialises in the care of critically ill cancer patients suffering from, for instance, acute respiratory failure and infection related problems such as sepsis or toxic reaction.
Admission criteria

‘We need to consider several factors when deciding whether critically ill cancer patients should be cared for in the ICU. Apart from the patient's general condition, we must evaluate the probability of surviving acute organ failure(s) along with the expected long-term survival and therapy options after intensive care. Intensive care treatment can be very strenuous and even traumatising and can affect the remaining quality of life, which is why the admission criteria are important,’ Schellongowski explains. Patients in the early stage of a disease, which is still treatable, and whose life expectancy is likely to be more than a year; patients who should receive curative treatment, and patients in remission from their primary disease, are usually always admitted. They are given a so-called full code management, meaning that they will receive the entire range of intensive care treatments available. However, if treatment options have been exhausted or intensive care is unlikely to improve a patient's life expectancy or condition we would refrain from treatment.
For patients receiving palliative care who may have a good chance of longer-term survival due to treatment progression, admission to the ICU can also make sense. This would be the case, for instance, for patients with low-grade non-Hodgkin Lymphoma. Intensive care treatment is also offered to patients in partial remission, such as patients in partial remission from multiple myeloma or solid tumours, as a long- term prognosis can be achieved in a palliative setting.
‘The group of patients who may benefit from intensive care continuously expands due to the broad range of cancer treatments available. Oncology is continuously evolving, making the exchange of information and a close cooperation between intensive care medics and oncologists so important: it guarantees the best treatment for the patient,’ Schellongowski explains.
Close examination
Despite structured criteria and guidelines, the decision-making process on treatment and admission objectives is often very complex. ‘A minimum "one-year survival" objective obviously does not mean that a patient with an 11-months survival prognosis will immediately fall outside the scope. Each case is intensively examined under various aspects.’
That includes a conversation with the patient, though it might not always be possible. ‘In intensive care medicine, the patient's ability to communicate and make decisions is often severely impaired and, whilst living wills are helpful, they are not yet that widespread. At the same time, the window of opportunity for making decisions on treatment is often tight. In each case, we always aim to act to the best of our knowledge and in the patient's best interest. If the situation is not clear-cut,’ he added, ‘we often start a so-called ICU trial. This multi-day treatment trial examines whether the patient responds positively to the treatment. Then we decide if it makes sense to continue with intensive care.’
In some cases, previously defined, limited intensive care treatment is considered, with certain procedures such as intubation being excluded. ‘A study has confirmed that this approach also helps a large number of patients to survive, and that survivors suffer from the anticipated post intensive care syndrome (leading to anxiety, depression or post-traumatic stress syndrome) no more frequently than patients without therapy limitations.’
Frequent ICU admissions
Unfortunately, the availability of data is not optimal
Peter Schellongowski
Outside of specialist centres, cancer patients are also frequently admitted to intensive care wards. ‘Unfortunately, the availability of data is not optimal. Based on available figures, we assume that every sixth to eighth patient on a European intensive care ward is a cancer patient,’ Schellongowski points out. ‘The majority of these patients have solid tumours and are in the ICU for observation and post-operative care for a number of days. However, a significant number of patients is also admitted due to internal complications from cancer and their treatment. Three to four percent of all patients on intensive care wards have haematological cancers, such as leukaemia or lymphoma. In these cases, cancer-specific, internal complications are the most common reason for admission.’
Patients in the early stages of a cancerous disease are in particular need of intensive care. Five to six percent of cancer patients with solid tumours are admitted to the ICU for primary surgical care in the early stage of the disease. For haematological patients the number is significantly higher. Especially among patients with aggressive, haematological cancers, up to 18% require intensive medical care during the early disease stage, either because complications have led to organ dysfunction or because aggressive treatment given at the start has caused secondary complications, which ultimately also lead to organ dysfunction.
Specific treatment
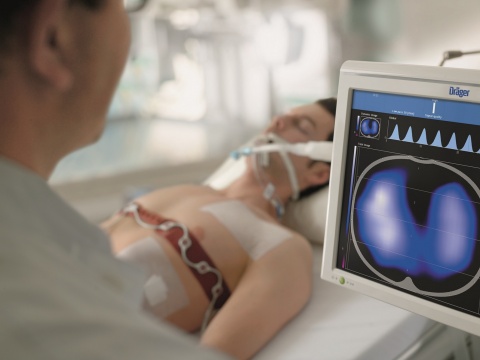
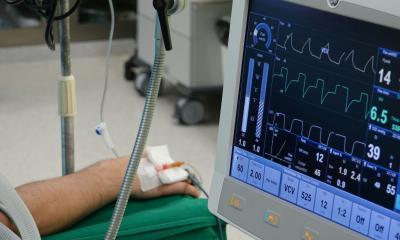
The most common cause for ICU admission is acute respiratory failure, followed by complications from sepsis. Haematological diseases in particular often lead to pulmonary complications, because infections or complications arising from leukaemia mean the lungs no longer function normally. It is essential to take the cancer background into account for diagnosis as well as empirical treatment. ‘With infectious complications arising from an aggressive cancer there is often a special range of pathogens involved. Most often we treat for several potential infectious causes, but sometimes we must simultaneously administer chemotherapy. ‘Occasionally, we cannot determine with any certainty whether pulmonary complications were caused by infection or by the disease itself. This complicates treatment, because chemotherapy can aggravate an infection. At the same time, chemotherapy cannot be suspended for too long, which is why we need to act with a lot of differentiation and need to carry out an intensive diagnostic investigation. ‘Close cooperation between haematologists and oncologists is therefore of extraordinary importance and very desirable,’ Schellongowski emphasises. ‘It’s scientifically well documented that intensive care patients with cancer, who receive intensive interdisciplinary care, have a better outcome". A German-Austrian consensus recommendation on this topic is due to be passed and published shortly.
Profile:
Associate Professor Peter Schellongowski MD PD, internal medicine and intensive care specialist and senior consultant in the ICU at Vienna’s Medical University, heads the working group on haemato-oncological intensive care medicine at the Austrian Society for Internal Medicine and General Intensive Care and Emergency Medicine (ÖGIAIN), and is deputy spokesman for the working group for intensive care medicine at the German Society of Haematology and Oncology (DGHO). He is co-founder and coordinator of the initiative Intensive Care in Haematologic and Oncologic Patients (iCHOP), and chairs the NEXT Committee of the European Society of Intensive Care Medicine (ESICM). Along with coordination of the ‘Register for Critically Ill Cancer Patients of the iCHOP Initiative’ he also heads the YELENNA Study on acute respiratory distress syndrome in cancer patients, for which he recently received the ESICM Young Investigator Award.
E-mail: peter.schellongowski@meduniwien.ac.at
15.11.2017