Personalised medicine
Computerised tailor-made retinopathy therapy
Nowadays the concept of personalised medicine is usually applied to oncology. However, there are other clinical disciplines in which therapies tailored to the individual patient are within reach, viz. ophthalmology. In the researchers’ limelight is intravitreal drug delivery since the outcomes of injections into the vitreous differ from patient to patient. Ophthalmologists in Vienna, Austria, are working on software to identify suitable therapy for each individual patient.
Report: Michael Krassnitzer
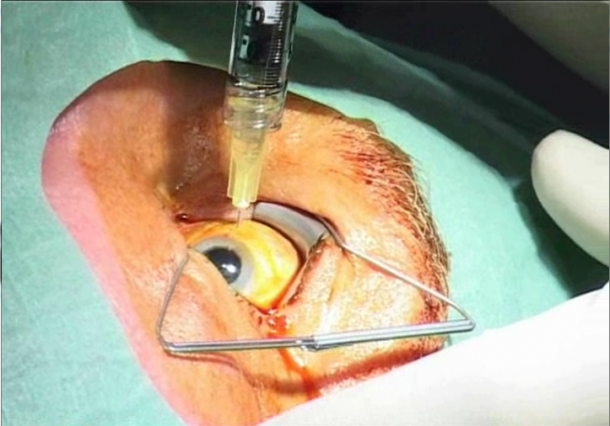

Intravitreal injections (IVI) are indicated for retinopathies such as age-related macular degeneration (AMD), diabetic macular oedema (DME) or retinal vascular occlusions. Antibodies are injected directly into the vitreous, which serves as a drug reservoir, and released to the retina over the course of a few weeks. Thus, for the first time retinal diseases can be treated directly – and successfully.
Thanks to intravitreal injections AMD is no longer the prime cause of blindness. However, there is a catch: In order to be on the safe side, the treatment must be repeated every few weeks – for life. ‘This is de facto impossible,’ says Dr Sebastian Waldstein, ophthalmologist at the Department of Ophthalmology and Optometry at the Medical University of Vienna, who is also in charge of the research focus Macular Degeneration at Vienna Reading Centre (VRC). ‘First, most patients simply cannot afford the monthly treatment financially,’ he points out, adding that it is also too stressful for the patient.’
Indeed, only a minority of patients need monthly treatment, he says. ‘For about two thirds of patients much longer intervals are entirely sufficient – in fact, some patients need only a few injections.’ Even better, ‘The course of retinal disease and the best treatment strategy can be predicted with a probability of ninety-nine percent probability’ using optical coherence tomography (OCT), a diagnostic procedure largely developed in Vienna, that has revolutionised ophthalmology within a few years. In OCT, hundreds of scans are combined to produce a 3-D image of the retina, which in turn allows reconstruction of the macula within seconds. However, the computing power behind this contactless procedure also poses a problem: the data volume generated in OCT is so huge that the ophthalmologist can no longer interpret it. To eliminate this quandary, Dr Waldstein is developing innovative computer-based methods to analyse large clinical image data sets.
To provide his research with an institutional framework, he initiated the Christian Doppler Laboratory for Ophthalmological Image Analysis, which he currently coordinates under the supervision of Professor Ursula Schmidt-Erfurth. The first results are already available: ‘The algorithms we developed need three exams to reliably predict the retinal status at the next scheduled exam and to predict whether the patient will suffer a relapse in the course of treatment,’ Dr Waldstein explains. These preliminarily tested methods must now be applied to large patient cohorts. ‘We delivered the proof of principle and expect prototypes for the large-scale evaluation to be available in one to two years.’
It may well be that the physician will not be able to comprehend the calculated results based on the algorithms. ‘The parameters that lead to the predictions might be highly complex,’ Waldstein says. ‘The analysis of big data is often a black box method. In short: the prediction is correct, but we don’t understand why.’ Dr Waldstein aims to provide software integrated into the OCT system, to offer a score or probability for the outcome that allows a physician to select the best possible treatment.
PROFILE:
Based in the Department of Ophthalmology and Optometry at the Medical University of Vienna, ophthalmologist Sebastian M Waldstein also leads research on macular degeneration at the Vienna Reading Centre (VRC). Additionally, supervised by Professor Ursula Schmidt-Erfurth, he coordinates the Christian Doppler Laboratory for Ophthalmological Image Analysis, a publicly funded, interdisciplinary research group set up to develop innovative computer-based methods to analyse large clinical image data sets. A native of Salzburg, Dr Waldstein studied medicine in Innsbruck and Vienna. Subsequently he has received prizes and awards from international professional associations such as ARVO, Max Kade Fellowship and ESASO.
28.04.2015