News • Genetic engineering
CAR-T: Landmark cancer study sheds new light on immunotherapy
Loyola University Medical Center is the only Chicago center that participated in the pivotal clinical trial of a groundbreaking cancer treatment that genetically engineers a patient's immune system to attack cancer cells.
Patrick Stiff, MD, director of Loyola's Cardinal Bernardin Cancer Center, is a co-author of the study, published in the New England Journal of Medicine. The treatment used in the study, which involves a cell therapy called CAR-T, is offered by Kite Pharma. Two other companies, Novartis and Juno Therapeutics, also are developing CAR-T cancer treatments. Dr. Stiff said Loyola is preparing to offer the treatment early next year to carefully selected lymphoma patients who have failed earlier treatments. He cautioned that while the therapy could potentially cure patients who have run out of other options, it also can cause severe side effects. The cost of the treatment is also considerable to patients. Dr. Stiff said Loyola would carefully inform patients of the pros and cons of this new therapy if it is presented as an option.
This is impressive, since most patients had exhausted all other care options
Patrick Stiff
"We are taking a very measured approach to this new therapy, which is effective, but also potentially toxic," Dr. Stiff said. "The therapy should not be considered a cure-all, since some of the patients did relapse after the therapy."
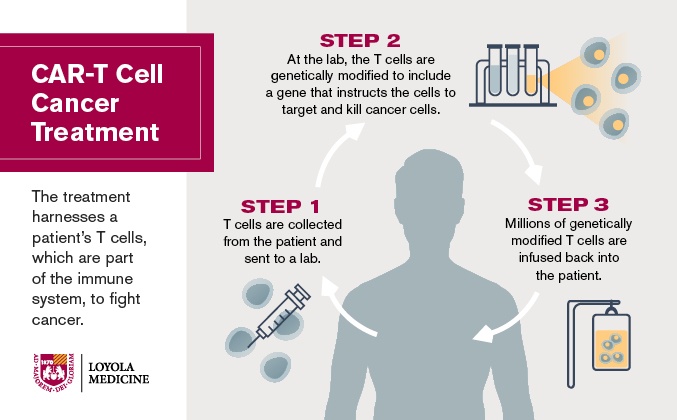
Based on results of the study, the Food and Drug Administration approved a CAR-T treatment called Yescarta. The study included 111 patients from 22 centers, including Loyola. The patients had certain types of large B-cell lymphoma and had not responded to or had relapsed after undergoing at least two other treatments, including chemotherapy and stem cell transplants. To fight the cancer, the treatment harnesses a patient's T cells (white blood cells that are part of the immune system). T cells are collected from the patient and sent to a lab. There, the cells are genetically modified to include a gene that instructs the cells to target and kill lymphoma cells. Millions of these genetically modified T cells then are infused back into the patient.
In the study, 42 percent of patients who underwent the CAR-T treatment were in complete remission after a median follow-up of 15.4 months. "This is impressive, since most patients had exhausted all other care options," Dr. Stiff said. Details in the report included that 95 percent of patients experienced at least one side effect that was severe. Thirteen percent experienced life-threatening cytokine release syndrome (CRS), which can cause high fever and flu-like symptoms, and 28 percent of patients experienced neurologic problems including encephalopathy (diseased brain), 21 percent; confused state, 9 percent; aphasia (difficulty communicating), 7 percent; and somnolence (excessive sleepiness), 7 percent. Other side effects included coma, serious infections, low blood cell counts and weakened immune systems.
The study found that the incidence of CRS and severe neurologic problems decreased over the course of the study, possibly due to the centers gaining more experience and this trend has continued. Dr. Stiff said Loyola's participation in the clinical trial, along with its extensive experience in treating patients with lymphoma and other blood cancers, will help in providing the safest possible CAR-T treatments. "We are developing a system to treat carefully selected patients who might benefit from the therapy with a maximum of benefits and a minimum of toxicities," he said.
The cure rate in the CAR-T study was similar to the approximate 45 percent cure rate from an allogeneic bone marrow transplant. In this well-established treatment, healthy stem cells obtained from a donor's bone marrow are infused into the patient. "Centers such as Loyola, which have expertise in both therapies, now will be able to offer additional treatment options to produce long-term remissions and cures in patients with advanced lymphomas," Dr. Stiff said.
Source: Loyola University Health System
11.12.2017