A clever(t) fusion for prostate diagnosis
Contrast-enhanced transrectal ultrasound and MRI
Statistically speaking every fourth older German man suffers from prostate cancer with the mortality rate being 60,000 patients annually

So what‘s more obvious than trying to improve diagnostics by combining the different modalities, asks Dr Dirk-André Clevert, ultrasound expert and Director of the Interdisciplinary Centre at the Institute of Clinical Radiology, Munich University Hospital.
In his opinion the combination of contrast-enhanced transrectal ultrasound and MRI offers many advantages. Nevertheless, he adds, there is room for improvement in image fusion and he urges industry to take up the challenge. There is always a certain risk that a prostate tumour remains undetected since certain areas of the gland are very difficult to image. MRI and ultrasound, the most frequently used imaging methods, have advantages as well as drawbacks. However, using the strengths of both technologies, Dr Dirk-André Clevert emphasises, can spell progress: ‘The advantages of contrast-enhanced ultrasound or even elastography pair excellently with high-resolution MRI.’
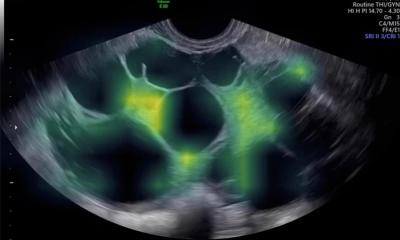
So far, the good news; now comes the bad. There are not enough suitable high-resolution transrectal transducers that can be used for image fusion. Moreover, medical imaging lacks target-specific contrast agents, i.e. micro-bubbles. These agents, which are currently under clinical development, dock only onto VEGF-2 receptors that are overexpressed in tumour vessels, such as prostate carcinoma. The target-specific contrast medium attaches via the receptors on the vessel walls where its characteristic luminescence makes it easily visible.
The receptors, as such, are not tumour-specific but, due to increased angiogenesis, the high receptor density in the tumour makes the diagnosis with micro-bubbles unambiguous. ‘It’s like flicking the light switch and suddenly some corners are illuminated,’ Dr Clevert explains. The method allows detection of several lesions in one go. Not surprisingly these advantages help with a decision immensely. ‘Most men who are given the choice between having a contrast medium injected and a prostate biopsy,’ he points out, ‘will opt for the contrast medium. Obviously a biopsy is required if the contrast-enhanced ultrasound yields a positive finding. Nevertheless, we can avoid a very unpleasant exam for many patients.’
There is indeed hope that current studies will show that fusion imaging can entirely avoid false-positive findings, which would mean near-100-percent diagnostic accuracy.
Several renowned manufacturers are exploring the market and have launched products; Bracco’s research lab in Geneva, for example, is at work on micro-bubbles. ‘As far as I’m concerned,’ Dr Clevert concludes, ‘optimising prostate cancer diagnostics is a useful and overdue objective because particularly this organ has remained a major challenge,’
* Based on an article in ‘RöKo HEUTE 2013’, the official publication of the German Radiology Congress
PROFILE
Private docent Dr Dirk-André Clevert began his medical career at the MRT-Diagnostik-Institut Westend in Berlin and the Department for Internal Medicine at Waldkrankenhaus Gransee. After a three-year residency in the Radiology Department at Passau Hospital, in 2003 the Berliner moved to Munich, heading the Interdisciplinary Ultrasound Centre – the focal point of all ultrasound activities in Munich University Hospital in Grosshadern – since the centre’s opening in 2004. Dr Clevert has designed, organised and taught many national and international ultrasound training courses. He is also Vice President of the European Society for Clinical Haemorheology and Microcirculation.
01.07.2013