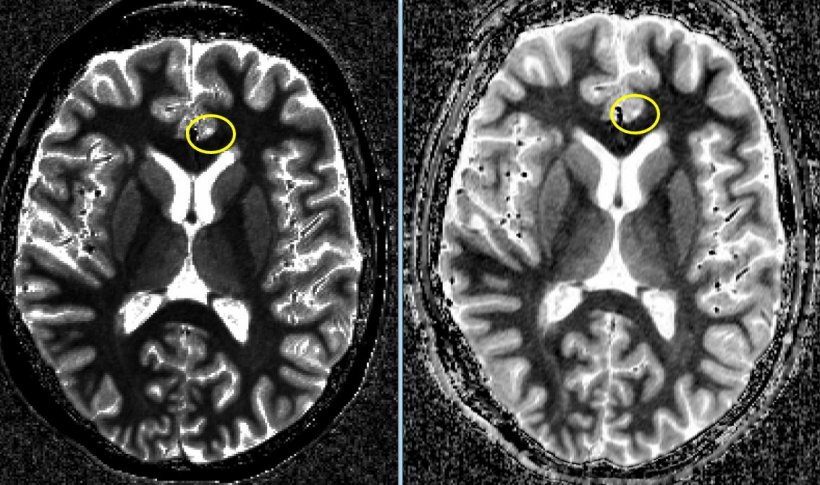
Source: Tallantyre et al, J Magn Reson Imaging 2010; Filippi et al, Neurology, 2010; Calabrese et al, Neurology 2009, Kilsdonk et al, Brain 2013, Harrison et al, JAMA Neurol 2015
Article • Maps of the brain
7-Tesla MR enters clinical routine
Ultra-high-field magnetic resonance tomography with field strength of seven-Tesla is slowly but surely entering clinical routine.

‘Thanks to very high spatial and spectral resolution, ultra-high-field MR permits detailed views of the human anatomy and can show precisely the metabolic processes such as those in the brain,’ emphasised Professor Siegfried Trattnig, head of the Excellence Centre for High-Field MR at Vienna’s Medical University. The most important application is neurological illnesses such as epilepsy or multiple sclerosis. Due to the combination of better signal-noise ratios, stronger tissue contrast and higher spatial resolution, things can be seen with 7-Tesla (7-T) that cannot be seen with 3-Tesla (3-T).
Hence many patients in whom lesional focal epilepsy is suspected exhibit inconspicuous findings under 3-T, despite a firm epilepsy protocol. 23 percent of the focal cortical dysplasias — the focal disturbances in the development of the cerebral cortex, often combined with epilepsy — identified using 7-T MR cannot be detected using 3-T-MR. ‘Today the suspicion of lesional focal epilepsy demands a 7-T MR — because, in the case of epilepsy, every lesion counts,’ Trattnig emphasised. With temporal lobe epilepsy, the most common epilepsy syndrome among adults, the neuron loss in the relevant sub-regions can be made visible, a pathological classification performed and even a prognosis of post-operative outcome made.
MRI for multiple sclerosis
MR examinations with 7-T can also better visualise the plaque in grey brain matter that correlates to clinical diagnosis in cases of multiple sclerosis (MS). Furthermore there are cortical MS lesions that can be seen under 7-T but not under 3-T. ‘That’s why it’s so important to correlate these cortical lesions with the clinical symptoms and the progression,’ the professor explained. Beyond that, they are extremely helpful for differential diagnosis: it is uncommon to find cortical lesions in certain illnesses that are easily confused with MS (‘MS mimics’) — such as neuromyelitis optica.
Around 40 percent of MS patients have brain lesions surrounded by iron rings. These are ferrous macrophage seams that surround some inflammation centres. However, only a third of these iron rings, visible with 7-T, can also be detected using 3-T. In Vienna it has been shown that the MS plaques that have an iron ring are slow-growing lesions, signalling progressive MS. ‘The 7-T MR examination offers a chance to evaluate the effectiveness of newly developed medications against chronic progressive MS using imaging,’ Trattnig pointed out. In this case the susceptibility weighted imaging (SWI) with 7-T is used.
Metabolic imaging
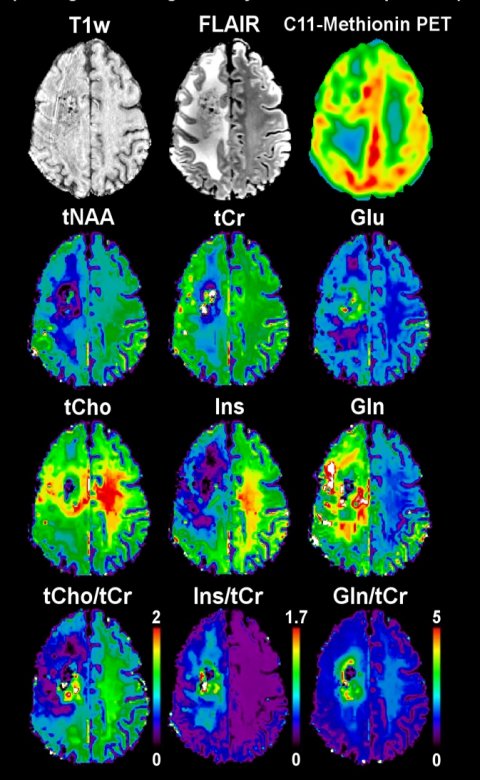
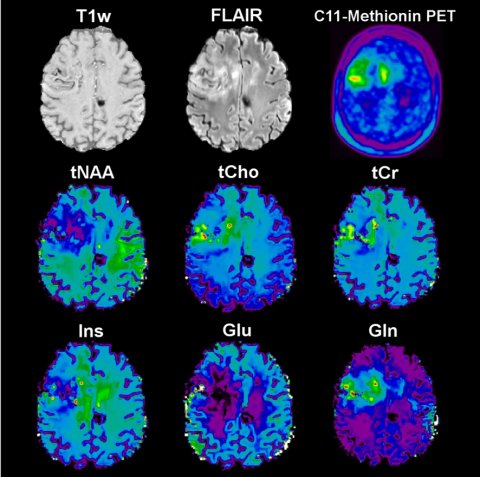
Ultra-high-field MR also permits pretty detailed metabolic imaging. ‘With a resolution less that one millimetre, we already see anatomical information in the metabolic maps,’ Trattnig said. Using so-called Patch-based Super-Resolution, the metabolic activity even inside small tumours can be rendered visible, such as with brain tumours that lie on the boundary between the cortex and core. Post-operative examination can render a good image of metabolic activities as an indicator of relapsing tumours around the resection zone, especially choline, a marker for tumour cell proliferation, as well as glutamine, which serves as a significant energy metabolite in some types of cancer. ‘Here we have a good correlation with PET maps,’ Trattnig said, ‘but the 7-T MR maps show many more structural details.’
Among other things, this is of clinical significance since, in the past years, it has been found that glutamine is an essential precursor for the metabolism of cancer cells. Using 7-T FID-MRSI (FID=free induction decay, MRSI= magnetic resonance spectroscopic imaging) it is possible to distinguish the amino acid glutamine from chemically similar glutamate—the most important neurotransmitter in the central nervous system — thanks to the higher spectral resolution of the corresponding maps. ‘Under 7-T, seven of the new metabolites in the central nervous system can be reliably mapped over the entire layer, under 3-T only three can be,’ Trattnig explained. One reason the maps, generated using FID-MRSI, are better is because they enable, among other things, a more exact tumour grading and hence a better targeted biopsy.
Profile:
Professor of Radiology Siegfried Trattnig specialises in high-field magnetic resonance use at Vienna’s Medical University. In 2000 he became medical director of the high-field MR research scanner and, since its establishment in 2003, of the high-field MR Centre (HFMRC) of MedUni Vienna. A member of more than 50 committees in international radiology, orthopaedic and MR societies, he has over 480 technical articles to his name.
26.02.2019