What´s new in breast MRI, tomosynthesis and elastography?
MRI: Although an area of constant debate, this is becoming a widely accepted clinical modality in Europe. However, researchers in The Netherlands have shown that performing pre-operative breast MRI in all women with invasive lobular carcinoma (ILC) can reduce the need for re-excision.
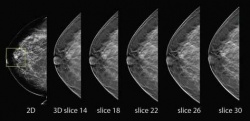
Tomosynthesis
Now gaining greater prominence, radiologists believe this technique has a bright future. Digital tomosynthesis, producing slice images using conventional X-ray systems, is a refinement of conventional geometric tomography in that it allows an arbitrary number of in-focus planes to be generated retrospectively from a sequence of projection radiographs acquired during a single motion of the X-ray tube.
Studies have also highlighted potential advantages from tomosynthesis in diagnostic accuracy for breast cancer that could also help cut the number of recalls for further examination. A team at King’s College Hospital, London, has been exploring the benefits of tomosynthesis over conventional 2-D breast screening using a machine provided by Hologic. They found an apparent advantage in diagnostic accuracy from tomosynthesis compared to 2-D imaging, both in the radiologist’s ability to diagnose cancer and either benign or normal findings.
In the last few months, tomosynthesis progress, future developments and specialist uses have been discussed at numerous radiology conferences globally. Dr Mitch Goodsitt, at the University of Michigan, said: ‘Advantages of tomosynthesis over CT are better spatial resolution in the imaging plane and lower radiation dose. A disadvantage of tomosynthesis relative to CT is poorer spatial resolution in the depth plane.’
Tomosynthesis to image the body (chest, knee and legs) received FDA approval in 2006 and as recently as September 2010, the FDA’s Radiation Device Panel voted in support of Hologic’s pre-market approval (PMA) application for their tomosynthesis breast imaging system. Promising new developments in tomosynthesis include contrast enhanced (DSA) applications and multi-modality applications such as combined tomosynthesis and automated ultrasound, combined tomosynthesis and Nuclear Medicine (SPECT) imaging and combined tomosynthesis and optical imaging. ‘The future is bright for tomosynthesis technology,’ added Dr Goodsitt.
Elastography
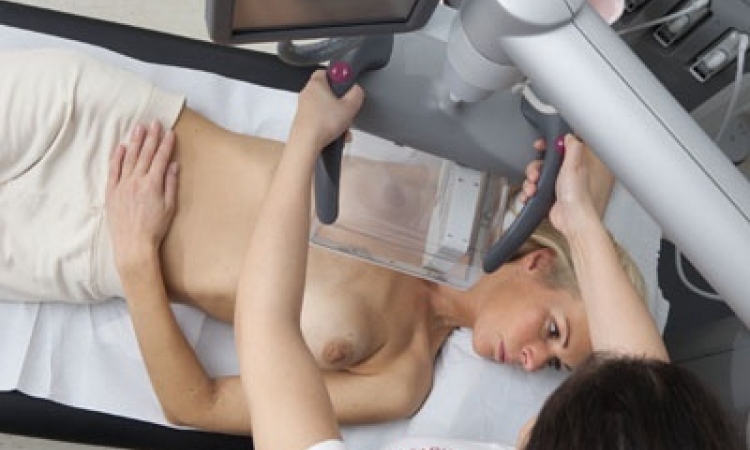
Here is another modality destined for an important future role, particularly in breast imaging with experts suggesting its potential to improve breast cancer diagnosis, reduction of false positives and fewer biopsies performed as accuracy of imaging improves further.
Elastography ultrasound measures stiffness or strain images of soft tissue to detect or classify tumours. Cancerous growth is between five and 28 times stiffer than the background of normal soft tissue so, with compression, the tumour deforms less than surrounding tissue indicating a possible cancerous growth.
Dr Bill Svensson, Reader in Breast Imaging at Imperial College London and Consultant Radiologist and Nuclear Medicine Consultant at Charing Cross Hospital, believes elastography is enabling radiologists to detect stiffer, harder areas and is a more sensitive imaging method. It provides more certainty in the image viewed and indicates what you should be getting from a biopsy result, he said. However, he remains concerned about the variability among manufacturers in the methods available for the technique and variations in readings and colour scales, which radiologists must be aware of and for which they must compensate. From basic strain imaging, elastography has evolved to utilise ShearWave and ARFI (acoustic radiation force impulse) imaging - a form of high-energy ultrasound - to provide more accuracy in estimating tissue stiffness being examined
22.02.2012