Image: University of Leeds
News • Prototype
This new, cheaper endoscope could redefine cancer screening
Engineers have developed a prototype endoscope which they say could cut the cost of manufacture from £80,000 to just £40. The redesigned device has the potential to revolutionise cancer screening in low-to-middle income countries where the cost of equipment makes screening prohibitively expensive.
The endoscope is designed to see inside the upper part of the digestive tract for signs of oesophageal or stomach cancer. Not only is the redesigned endoscope cheaper to make, it is more intuitive to operate and does not need sterilising between patients. That part of the device that passes into the gut is discarded after each procedure. The engineers say the disposable components will cost no more than £2 per patient. The international consortium behind the prototype is being led by the University of Leeds. Project leader Pietro Valdastri, Professor of Robotics and Autonomous Systems at Leeds, said they had had totally redesigned the endoscope which had remained largely unchanged for the last 60-plus years.
Simplifying the system
The new device is designed for use in locations where healthcare facilities are more basic, perhaps outside of a hospital setting
Pietro Valdastri
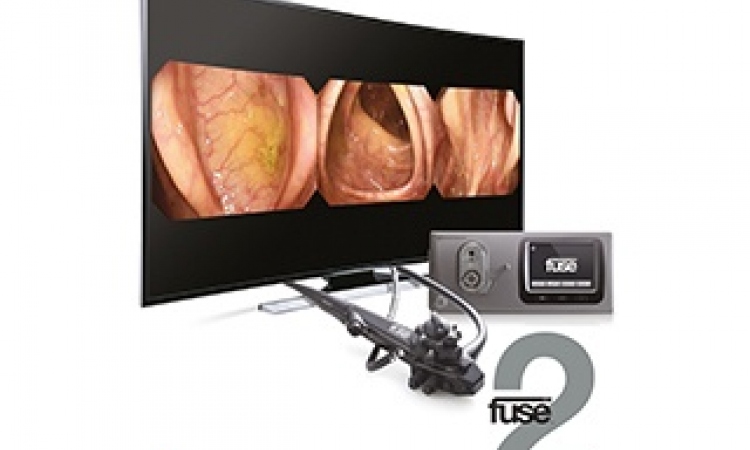
Instead of a complex mechanical system of cables and cogs, the prototype is pneumatically operated. It is made up of the hand-held control column and a disposable section comprising a narrow silicone tube and a tiny capsule housing the camera – dubbed the pill camera because of its size, which the engineers are aiming to get down to 8mm. At the end of each procedure, the silicone tubing and camera housing are disposed of.
Professor Pietro Valdastri said: “By radically re-thinking the way the device works, is manufactured and operated - we have come up with a solution that is a fraction of the cost of conventional endoscopes. Based on the prototype, we estimate the device could be manufactured for around £40. Currently, conventional endoscopes cost roughly £80,000. Cancer of the stomach and oesophagus have the highest global mortality rates. Screening programmes in many low-to-middle income countries are non-existent or ineffective because endoscope facilities are few-and-far between. Conventional endoscopes require cleaning between patients and that requires a dedicated sterilisation suite adding to the costs of the procedure. The new device is designed for use in locations where healthcare facilities are more basic, perhaps outside of a hospital setting.”
The next stage for the research team is to trial the effectiveness of the low-cost device against conventional endoscopes.
Recommended article

News • Microscopy in the body
The next generation of endoscopy technology
Biotechnologists, physicists, and medical researchers at FAU have developed technology for microscopic imaging in living organisms. A miniaturised multi-photon microscope, which could be used in an endoscope in future, excites the body’s own molecules to illuminate and enables cells and tissue structures to be imaged without the use of synthetic contrast agents. The findings have now been…
Work to develop the low-cost endoscope has been funded by the Global Challenges Research Fund (GCRF), UK aid money designed to use the best of British science to tackle big problems facing the world.
Philippa Hemmings, Head of Healthcare Technologies at the Engineering and Physical Sciences Research Council, said: “The work, led by the University of Leeds through the EPSRC GCRF award, demonstrates the benefits of international, multidisciplinary teams working on an intractable problem. This project demonstrates the key role engineering and physical sciences have in supporting the health of the global population.”
Professor Valdastri says the technology could have a big impact in China where in 2015 more than one million people were diagnosed with gastric and oesophageal cancers. Screening programmes have been difficult to implement in rural China because of a shortage of doctors. He said: “Screening is effective at picking up the early signs of these cancers and there is an urgent need to develop technology which opens up these crucial checks to poorer populations.”
Unlike more expensive endoscopes, the device cannot take biopsies. It is also smaller, reducing the need for patients to be sedated and because it is made of silicone, it is less likely to cause damage to the tissues in the upper digestive tract. Professor Valdastri hopes to have the device in use within four years.
Source: University of Leeds
17.04.2019