Robot navigates catheter to correct atrial fibrillation
Italy - A remotely-controlled catheter device guided by magnetic fields provides a safe and practical method for delivering radio frequency ablation treatment in the hearts of patients with atrial fibrillation, according to a new study (Pub: Journal of the American College of Cardiology. 4/4/06).

‘A new era in interventional electrophysiology is beginning as magnetic, very soft catheters can be navigated in the heart more precisely and safely than manual catheters without risk of major complications, even in less experienced centres,’ said Carlo Pappone MD PhD, of the Department of Electrophysiology, San Raffaele University Hospital in Milan, Italy.
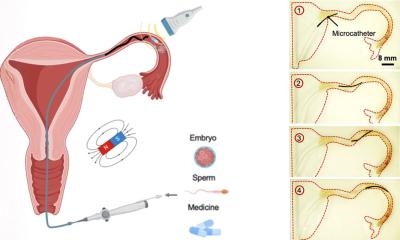
Radio frequency ablation to correct atrial uses a high-energy pulse to destroy a small area of heart muscle cells, to prevent them from conducting nerve signals that trigger fibrillation. Typically the radio frequency pulse is emitted by from a catheter tip, threaded through blood vessels into the heart until it is positioned next to the target area. Conventional catheters are somewhat stiff, so they can be pushed and pulled through blood vessels, and the tips curled and pointed by an operator standing next to the patient.
The device tested in this trial uses a very soft, limp tip with a magnet on the end. Rather than manually pointing the catheter tip, the operator uses a computer to control a magnetic field that robotically steers the catheter tip to a target visualized on 3-D scans of the patient’s heart.
‘Catheter ablation for atrial fibrillation is now an important treatment for this common disorder, but the current strategy of manual catheter manipulation is highly operator-dependent, with a long and variable learning curve and a great potential for both inefficacy and complications in inexperienced hands. Robotic navigation may increase the ability of inexperienced operators to perform this procedure easily and safely, as it is most dependent on a well-trained team rather than on a single operator,’ said Dr Pappone.
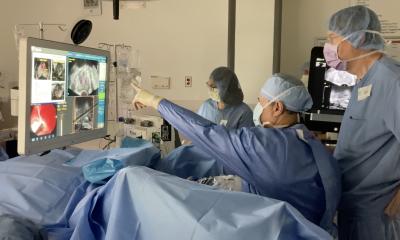
Since catheter procedures of this type require frequent use of X-rays to track the location of the target and catheter tip, another advantage of remote navigation is that the operator can work from a shielded control room, rather than having to stand next to a patient for several hours while wearing protective lead aprons.
This first trial of the robotic magnetic navigation system in patients with atrial fibrillation involved 40 participants whose conditions were not adequately controlled by medication. After encountering some difficulties in the first three patients, the researchers said the remaining procedures went smoothly. In all, the catheter tip was successfully guided by magnetic navigation to the target and radio frequency ablation was applied in 38 of the 40 study participants. There were no reported complications during the procedures.
‘Based on our results, we believe that incorporation of remote navigation and ablation in the electrophysiology laboratory may represent a true revolution regardless of age and experience of the operators leading to a seismic change in electrophysiologic paradigms for many laboratories worldwide. People always have had a love/hate relationship with robots, but this psychological barrier must be overcome. After performing more than 10,000 procedures with manually deflectable catheters, I have become enthusiastic for this emerging field,’ Dr Pappone said.
Mitchell N Faddis MD PhD, at the Washington University School of Medicine, St. Louis, Missouri, who was not involved with this study but helped develop the remote magnetic navigation system the researchers used added: ‘The work of Pappone et al. is extremely exciting to me as the culmination of this work, and to the cardiology community in general as a potential important technical advance in the treatment of atrial fibrillation.’ The new system should be easier to master, as well as being more precise, than conventional catheter ablation, he added. ‘Because of computer control, the efficiency of the procedure may improve. By the end of the 40 patient cohort of Pappone et al., procedures were routinely performed in less than an hour. This is likely to have an important impact on the complication rate for the procedure, which is likely to be affected by procedure duration.’
Dr. Faddis is a consultant with Stereotaxis Inc and receives research funding from the company. The study was supported by a grant from Johnson & Johnson.
Source: American College of Cardiology
01.05.2006