Image source: Anne Weston, Francis Crick Institute (via Wellcome Collection; CC BY-NC 4.0)
News • Reduced harm, reduced costs
Prostate cancer: MRI and blood test improve screening
The combination of a novel blood test and magnetic resonance imaging (MRI) can reduce overdiagnosis of low-risk cancers as well as societal costs in prostate cancer screening, according to a cost-effectiveness study from Karolinska Institutet.
The results, which were published in the journal European Urology, provide support for organised prostate cancer testing in Sweden, researchers say.
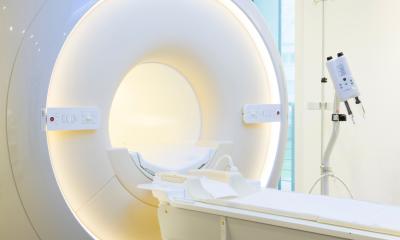
A barrier to the introduction of nationwide prostate cancer screening has been that PSA (prostate-specific antigen) tests combined with traditional biopsies result in the detection of numerous minor low-risk tumours. MRI has been shown to reduce this overdiagnosis but presents a challenge due to limited health resources. The STHLM3MRI trial has previously shown that a blood test called Stockholm3, developed by researchers at Karolinska Institutet, can reduce the number of MRIs by a third for a single screening occasion. Now, the same research group reports that this combination is also considered cost-effective in Sweden compared with both no screening and PSA test in MRI-based screening.
Recommended article

Article • Over-detection and biopsies
New procedures for prostate cancer screening
Organised screening enabling early detection and treatment of prostate cancer can reduce death by an impressive 20%, based on 16 years of findings of over 160,000 men participating in the landmark European Randomised Study of Screening for Prostate Cancer (ERSPC).

Image source: Karolinska Institutet; photo: Gunilla Sonnebring
“Our latest results show that using Stockholm3 reduces the number of MRIs over a lifetime by 60 per cent. This also avoids unnecessary biopsies by 9 per cent, which reduces the overdiagnosis of low-risk cancers,” says Mark Clements, associate professor at the Department of Medical Epidemiology and Biostatistics, Karolinska Institutet, who is responsible for the cost-effectiveness study.
The analysis predicted that MRI-based screening combined with PSA or Stockholm3 would reduce prostate cancer-related deaths by 7–9 per cent over a lifetime compared with no screening at all. The health economic evaluation showed that, compared with no screening, screening with PSA followed by Stockholm3 and MRI in high-risk individuals is classified as a moderate cost per quality-adjusted life-years (QALY) gained as defined by the Swedish National Board of Health and Welfare. Furthermore, PSA combined with MRI is classified as a very high cost per QALY gained compared with Stockholm3 combined with MRI.

Image source: Karolinska Institutet; photo: Stefan Zimmerman
“This new combination with Stockholm3 can save healthcare resources and reduce societal costs while maintaining the health benefits from early detection of prostate cancer. This presents an interesting option for prostate cancer screening in Sweden,” says Shuang Hao, PhD student at the Department of Medical Epidemiology and Biostatistics, Karolinska Institutet and the first author of the study.
Several regions in Sweden have started to plan and implement pilot projects for organised prostate cancer testing (OPT) through the regional cancer centres. The National OPT Working Group has recommended that the OPT pilots investigate the use of different strategies for prostate cancer screening.

Image source: Karolinska Institutet; photo: Stefan Zimmerman
“Our evidence provides support for using Stockholm3 as an additional test in MRI-based screening, which could be evaluated through one of the OPT pilots,” says Tobias Nordström, associate professor of urology at the Department of Clinical Sciences, Danderyd Hospital at Karolinska Institutet, who is the principal investigator for the STHLM3MRI trial and a co-author of the cost-effectiveness study.
The current health economic evaluation is specific to Sweden, but the simulation model used in this study is open source and can be readily adapted to assess the use of Stockholm3 and MRI in other countries. The Stockholm3 test is available for clinical use in Sweden, Norway, Denmark, Finland, Spain and Germany, and will be made available in additional European countries in 2022.
Source: Karolinska Institutet
31.01.2022