Article • Getting personal(ised)
Pathology: Moving us towards precision medicine
The European Society of Pathology (ESP) holds its European Congress of Pathology (ECP) at different venues annually. This year, in Spain, 3,448 delegates from 87 countries attended. There, ESP president Dina Tiniakos spoke about the increasing role of pathology in precision medicine including challenges linked to digitisation.
Report: Mélisande Rouger

‘Precision medicine is the centre-point for cancer management, but also important for non-neoplastic diseases,’ Tiniakos explained. ‘Oncologists need the correct histological diagnosis and information on underlying gene mutations to offer the right personalised medication. Pathologists play a key role in this respect, because they make the diagnosis and also offer information about the mutations present in a tumour. Pathologists make the conventional diagnosis using glass slides and diagnose the presence and expression of certain proteins using immunohistochemistry. We also perform molecular pathology testing on tissue samples taken from the tumour, and can give a combined report in addition to the traditional histology used several years ago.
For breast cancer, for example, pathologists can give information about oestrogen and progesterone receptors status and HER2 protein expression status. Patients whose tumour has over-expressed HER2 protein due to underlying gene amplification can be treated with anti-HER2 monoclonal antibodies. Pathologists have a nodal role in guiding patient management. Therefore, the only path to precision medicine is through pathology.’
Digital benefits
‘With digital slides, we can work directly on our computer screen and slides are digitally stored. Collaboration and consultation are easier – slides can be shared from anywhere. When I’m in Athens, I can assess the slides I stored at Newcastle University, for example. Digital pathology is still not being used routinely in most labs, but it’s the future – where we are going. We need to ensure all remaining issues are properly tackled. A major drawback: a large digital storage space is needed. Digital slides are huge. Labs that want to go digital need to apply to clouds and rethink their information technology (IT) strategy, to find appropriate solutions.
‘Pathologists don’t work as fast as they’d like, because it takes more time to interpret digital slides than glass slides. I still prefer to look at glass. Digital evaluation requires a long learning curve, and time to change the way our brain works looking at slides. Young pathologists have an easier time because their brain is more adapted to working with the screen. It will become easier for everyone else as well. Studies show there are no significant differences between glass and digital slides. Most importantly, the pathologist needs to be well trained to interpret both glass and digital histological slides. The FDA doesn’t approve of histological assessment with digital slides in a clinical trial setting yet. There isn’t enough evidence regarding the agreement on histological scoring between glass and digital slides.’
IT solutions in clinical practice
A number of issues remain to be tackled, including using patient data to train the machine, even if data is anonymised
Dina Tiniakos
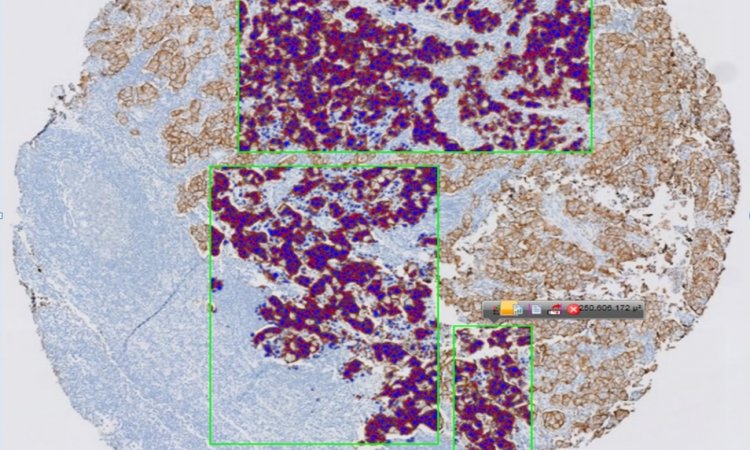
‘We use tools that help us objectively to evaluate immunohistochemical stains for scoring, for example presence of oestrogen and progesterone receptors in breast carcinoma, or Ki67 proliferation index in neuroendocrine tumours. Dedicated software can measure cell numbers with nuclear immuno-sustaining indicating the presence of receptor expression or cell proliferation, instead of manually counting cells. In Athens we use a commercially available system, but it’s also possible to develop a simple “home-made” solution, with local IT colleagues. IT tools are good companions in our traditional pathology diagnosis; they can save time.
‘AI is a very interesting development for pathologists. Machine learning may help routine diagnosis using algorithms that can pinpoint areas of interest in a section, or classify simple benign cases as such, for example. These tools may help us decide if a certain feature is present or not. In liver pathology, it’s still experimental, but there are platforms that can identify the extent of steatosis, i.e. fat in liver. Pathologists have to train the machine – a lot of work, but this will become a great tool. It’s only the beginning and something pathologists should look positively upon. A number of issues remain to be tackled, including using patient data to train the machine, even if data is anonymised. The controversy surrounding the deal between an AI start-up and the Memorial Sloan Kettering Cancer Center recently showed the delicacy of this issue.

Challenges
‘We need to be well trained to use these tools properly. The ESP has an IT technology working group, which organises congress sessions. There was a dedicated symposium on this at the ECP. No special guidance is issued but training pathologists in effectively using IT is among our aims. The ESP educational portal enables members to access all educational material recently collected throughout our courses. ESP courses are run by experts for residents and consultant pathologists across Europe. For young pathologists the ESP funds specialised 1-3-month training in centres of excellence, with all expenses covered (Giordano Fellowship).
At the ECP 2018 free access and over 150 grants were awarded, with travel and accommodation funding for young pathologists who submitted an abstract accepted for presentation at the congress. In five years, about €200,000 grants and fellowships were awarded.'
Profile:
Dina Tiniakos, President of the European Society of Pathology (2017-19), is Associate Professor at the Medical School in the National & Kapodistrian University of Athens, Greece, and Senior Lecturer at the Institute of Cellular Medicine, at Newcastle University, UK. A specialist in hepatobiliary pathology, she researches fatty liver disease and hepatocarcinogenesis. She is also the author or co-author of around 130 peer-reviewed scientific articles and chapters in liver pathology and histology, and is on Editorial Boards of several scientific journals and is an external assessor for various European research grants bodies.
14.01.2019