Image source: Adobe Stock/koya979
News • ‘European Cancer Pulse’
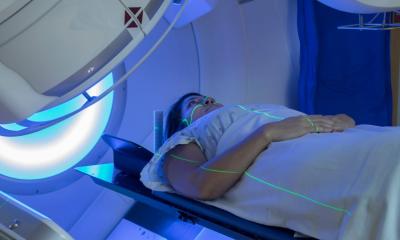
New online tool reveals vast cancer care inequalities in Europe
A new online ‘European Cancer Pulse’ tool, created to compare cancer data across Europe, has highlighted that only 12 of the 27 EU Member States have an up-to-date national cancer control plan.
The research has been published in the Lancet Oncology journal and was led by Professor Mark Lawler, Professor of Digital Health at Queen’s University Belfast, European Cancer Organisation (ECO) board member and Scientific Lead of the European Cancer Pulse project.
The new user-friendly tool features more than 120 data measurements – from 34 countries throughout the European Union, and beyond. It allows anyone to quickly and easily discover cancer care disparities between countries. For example, the inequality in relation to workforce issues: how Germany has 1,395 nurses per 100,000 inhabitants, whereas for the UK that number drops to 778.
Commenting on the results, Professor Lawler said: “How can you ever improve cancer care in a country that lacks an up-to-date national cancer plan? The European Cancer Pulse shines a critical light on which countries are falling behind on cancer care – and specifically how. It empowers us to use data intelligence to identify the problems, but more importantly to do something about them.”
Recommended article

News • Oncology forecast
Is Europe facing a 'cancer epidemic' in the next decade?
With an estimated one million cancer diagnoses missed across Europe in the last two years, the impact of the Covid-19 pandemic is predicted to set back European cancer outcomes by almost a decade.
The new tool complements the existing European Commission’s Cancer Inequalities Registry, pulling together key additional facts and figures from many more European countries: How much is a country spending on cancer research? How many CT or PET scanners does it have? What percentage of citizens know about cancer risks and symptoms? How is the level of cancer care received influenced by a person’s income, gender, age, education, and other social factors?
In the United Kingdom, the Pulse specifically reveals that the cancer incidence and obesity rates are among the ten highest in Europe, while it has Europe’s second lowest numbers of CT scanners, MRI units and radiologists, thereby creating great risk of severe diagnostic and treatment delays.
Our data intelligence indicates that solving these health and cancer disparities must be prioritised at a political level, both Europe wide and nationally, in order to improve the lives of those European citizens affected by cancer
Mark Lawler
The issue extends past diagnosis, as the UK also has significant workforce shortages, particularly in relation to cancer nurses, and is also among the most severely under-resourced among Western and Northern Europe for radiation therapy equipment. Meanwhile, the United Kingdom performs relatively well on ensuring timely access to innovative cancer medicines, as these take under nine months to be included in public reimbursement, compared to over 18 months on average in the European Union.
In Ireland, the Pulse specifically reveals that it takes on average over 20 months for new cancer medicines to be included in public reimbursement, making it among the longest in Western and Northern European countries, compared to four months in Germany for instance. Ireland also has challenges in relation to screening for colorectal cancer, with just 1 in 3 persons above 50 reporting having undertaken a test in the last three years, as compared to over 75% in Denmark. Meanwhile, Ireland is relatively well-equipped in terms of cancer workforce, being 37% and 45% over the European average for oncologists and nurse numbers, respectively.
ECO President Andreas Charalambous said: “The European Cancer Pulse is a new home for new data, bringing together the excellent work done by the European cancer community. Improving cancer care requires measuring and highlighting what each country is doing and comparing it to other countries. Where are we ahead? Where are we lagging – and why?”
Additional data is being added to the European Cancer Pulse regularly, helping to reflect the full scope of cancer research and care in Europe and to monitor improvements – or lack thereof. This includes ongoing research on cancer workforce capacity limits and social inequities affecting marginalised populations in cancer.
Emerging evidence shows that there is still a long way to go before equitable access to cancer prevention, research and care is achieved across Europe. Aside from existing inequities, persistent issues such as the health workforce crisis represent significant risks for deteriorating outcomes in the coming years.
The influence of the Covid pandemic is also critical. Professor Lawler adds: “Our data intelligence indicates that solving these health and cancer disparities must be prioritised at a political level, both Europe wide and nationally, in order to improve the lives of those European citizens affected by cancer. The European Cancer Pulse represents a crucial asset that we must deploy effectively in our fight against cancer.”
Source: Queen's University Belfast
05.05.2023