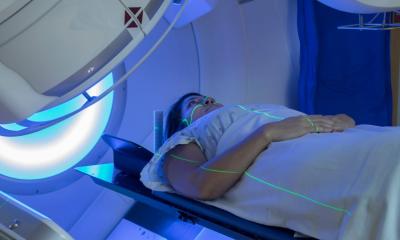
Image source: Adobe Stock/Andrii Zastrozhnov
News • Inequalities in diagnostics, treatments and care
Cancer care in Europe: alarming gaps remain
To mark World Cancer Day on 4 February, Ulrika Årehed Kågström, President-elect of the Union for International Cancer Control (UICC), and former UICC Board Members Nick Grant and Cristiana Fonseca offer their insights and solutions to the widening gaps in preventing and surviving cancer for people living in Sweden, the UK, Portugal and Europe more widely.
The World Cancer Day 2024 Equity Report can be accessed here.1
Europe accounts for about 20% of the global cancer incidence and mortality, with about four million new cancer cases recorded in 2020 and an estimated 1.9 million people who died from cancer.2
Yet even in countries in Europe, such as Sweden, the UK and Portugal, which have a tradition of robust healthcare, disparities exist in the risks of developing cancer, having it detected early and successfully treated. These disparities are a result of inequitable access to reliable information, screening, diagnostics, treatment and care services due to where people live, their economic status, level of education, ethnicity, age, physical and mental capabilities, age, gender and gender norms, sexual orientation and other socioeconomic factors.

Image source: Cancerfonden; photo: Klas Sjöberg
Ulrika Årehed Kågström, Secretary-General of the Swedish Cancer Society and President-elect of UICC, explains: “For people with low socioeconomic status, the risk of dying from cancer in Sweden is notably higher compared to those who belong to more privileged groups.3 People with higher education generally spend more time with healthcare professionals to ask questions when seeking care than those with only primary school education, who are more likely to refrain from care-seeking in the first place. Socioeconomic status can also influence the degree to which a cancer patient is likely to follow through on treatment.”
Nick Grant, Executive Director of Strategy and Philanthropy at Cancer Research UK and former UICC Board Member, says that, in the UK, limited progress has been made in addressing inequities in the past ten years. These have even worsened since the Covid-19 pandemic. “Life expectancy has stalled, and the gaps in life expectancy between the most and least underprivileged areas has widened. Many of the causes lie not in the health system itself, but in the broader environment – which makes it harder for some groups to live a healthy life. Smoking accounts for half the difference in life expectancy between the lowest and highest income groups in England. Bold action to reduce smoking rates – such as the legislation proposed by the UK Government to raise the age of sale of tobacco products – can help create a healthier society for all,” says Nick Grant.
Where you live, how much money you make, your age, your health, your gender, who you love or the colour of your skin shouldn’t dictate whether you have access to cancer care. But the sad reality is, it does
Cary Adams
Cristiana Fonseca, Health Education and Capacity Building Head of Department at the Portuguese League Against Cancer - Northern Branch, says about the situation in her country that “while there are national screening programmes for various cancers, their implementation and attendance rates vary across regions, and investment in research and treatment has improved cancer prognosis, but disparities persist in resource distribution and management practices in different regions and institutions.” Ms Fonseca also highlights inconsistencies in strategies to address environmental and other risk factors for cancer.
As modifiable behavioural factors contribute to over 40% of all cancer deaths,4 UICC’s World Cancer Day 2024 Equity Report emphasises overall that implementing cost-efficient and evidence-based prevention measures, such as limiting the marketing, sales and consumption of tobacco, alcohol and unhealthy foods that can lead to overweight and obesity, are crucial to reducing health inequity and the cancer burden.
Cristiana Fonseca further recommends “multisectoral policies targeting modifiable determinants of cancer, prioritise equitable access to treatments, and continuously monitor and reduce inequalities, especially for specific groups such as migrants and those not fluent in the country’s official language.”
Screening programmes, the early detection of cancer and access to timely treatment and care for people who develop cancer – regardless of their ability to pay – are also vital. The chances of treating cancer successfully are generally higher the earlier it is diagnosed.
Ulrika Kågström and Nick Grant offer several recommendations directed at national policymakers, which are applicable in many other countries in Europe:
- Improve the collection of consistent data about cancer prevention, cancer patients and those engaging with cancer services.
- Establish national measurable goals for how the socioeconomic and geographical differences in cancer care are to be reduced.
- Mobilise different government departments beyond health to reduce broader health inequity.
- Implement lessons learned and proven methods to improve health in the groups where it is the lowest.
- Reduce barriers to accessing early diagnosis and screening programmes, actively encouraging help-seeking and screening participation in unrepresented groups.
- Commit to reduce inequities in smoking prevalence, with a target prevalence of 5% across all socioeconomic groups by 2040.
Dr Cary Adams, CEO of UICC, says, “Where you live, how much money you make, your age, your health, your gender, who you love or the colour of your skin shouldn’t dictate whether you have access to cancer care. But the sad reality is, it does. That’s why UICC’s Equity Report is so crucial – it shines a light on the obstacles people face in getting the care they need, and suggests strategies to help overcome them.”
References:
- World Cancer Day 2024 Equity Report; UICC
- Cancer in Europe: 5 things the data tells us; European Commission, Jan 13, 2022
- Cancerfondsrapporten 2018 (Swedish Cancer Society Report, in Swedish); Cancerfonden, 2018
- GBD 2019 Cancer Risk Factors Collaborators: The global burden of cancer attributable to risk factors, 2010–19: a systematic analysis for the Global Burden of Disease Study 2019; The Lancet 2019
Source: Union for International Cancer Control
31.01.2024