Image source: Shutterstock/nednapa
Article • Seeking an ideal lab life
New and old challenges in laboratory medicine
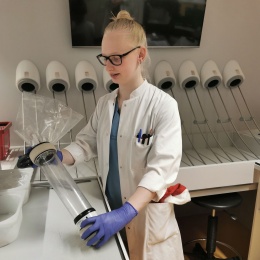
The Central Laboratory at the Medical University Hanover, Germany, is prepared to handle virtually any clinical chemistry task, from a routine test to the most complex analysis.
Report: Daniela Zimmermann
Equipped with state-of-the-art technology and thanks to a high degree of automation, the team can process more than 3,000 specimens, mostly blood and urine, in a single day. Professor Ralf Lichtinghagen, European Specialist in Laboratory Medicine, and Head Clinician in Hanover, and Dr Martin Christmann, European Specialist in Laboratory Medicine at the Central Lab, in Hanover, explain the challenges a lab of that size is facing today.

‘The German healthcare system poses a very specific problem regarding who is allowed to perform and invoice which tasks in a medical lab,’ Professor Ralf Lichtinghagen explains. ‘The guidelines on evidence-based medicine (EBM) and the German medical schedule for physicians (GOÄ) prescribe that, under normal circumstances, special lab medical services must be provided personally and invoiced by a laboratory physician, particularly services rendered by a specialist lab in a hospital.
Whilst other non-physician medical specialists, such as clinical chemists or those in human genetics are usually able to provide the same kinds of services, the hospital is not allowed to invoice for the services they render. In view of the scarcity of lab physicians this requirement creates a real problem. ‘Currently, hospitals can only invoice certain lab services if they were performed by a laboratory physician,’ Lichtinghagen points out. Thus invoicing specialist lab services is a real issue – because it is actually illegal for a physician to place an order for lab services for her- or himself.
The German Society for Laboratory Medicine (DGKL) is exploring possible solutions to this problem. To provide the necessary medical element one idea being discussed is additional training in a master program in laboratory medicine aimed at chemists, biochemists, biologists and comparable professionals. As yet the stakeholders, i.e. the affected professional associations, have failed to agree to recognise the state certification such a program would entail. Lichtinghagen is convinced that a certified program can effectively dissolve the bottleneck because, he believes, ‘there are plenty of scientists who are extremely interested in the clinical aspects, such as pathologies and the reading of findings’.
Potential of savings is overestimated

Labs are faced with another staff-related problem: lab managers’ expectation that an additional lab line will allow a significant staff reduction is clearly unrealistic. The new technologies and procedures, which are highly complex, require specially trained teams. Moreover, the extensive range of tasks in a modern lab means that not all staff members can be equally well-versed in all areas. In everyday lab life non-specialist staff thus increasingly dread night and weekend duty because they don’t feel sufficiently prepared to bear the responsibility, particularly regarding tasks they do not routinely perform. ‘Many team members are far beyond their acceptable stress level, which carries the risk that the entire system collapses,’ Lichtinghagen points out.
Ideally, each lab has a core team that is sufficiently large and underwent comprehensive training in all relevant areas. But, with automation being the current buzzword, many decision makers in the labs do not wish to acknowledge that more and better trained staff is needed. Quite the contrary, as Christmann adds, ‘further staff reductions are expected’.
The role of AI in the lab
Artificial intelligence (AI) is another fashion, permeating all professional symposia. In reality, however, AI as yet has little relevance for the everyday lab workload. This lack of relevance is particularly true, as Christmann points out, for ‘AI in the sense of machine learning processes that enable a system to develop by itself based on data or algorithms’. He does acknowledge AI’s potential regarding detection of rare diseases: every clinician is familiar with the standard characteristics of the most frequent diseases in the ER, in endocrinology and paediatrics. However, rare diseases, i.e. those a physician faces perhaps once in twenty years, are not on the mental radar screen. In such a case, the computer can provide the crucial pointer towards a specific disease. ‘This is a useful field for AI and would help patients who have run the entire diagnostic gamut without clear results.’ Christmann is convinced that, in clinical chemistry and in the lab, there will always be a team of people who are experts in the basics, even if AI could gain ground in the lab.
LOINC as a 'common language'
Lab procedures are neither standardised to any meaningful extent, nor is there an organisation that pushes for a common framework, mandatory data and binding criteria. In Germany, the DIMDI (German Institute of Medical Documentation and Information) currently manages standard interfaces, i.e. HL7 to communicate findings and orders and ASTM for communication between devices.
However, the standards are helpful only to a certain degree. The moment a lab has to read and analyse data from different sites, e.g. values established in Hanover and Göttingen, unambiguous allocation is difficult. A specific ‘language’ such as LOINC (Logical Observation Identifiers Names and Codes) might offer a solution. ‘Take the measurement of electrolytes for example. For systems to be able to communicate with each other the value called ‘serum sodium’ in one lab and ‘sodium in serum’ in another lab needs to have the same code,’ Christmann explains. The same holds true for the different measuring methods of lab parameters, such as creatinine: enzyme measurement on the one hand, and the Jaffe method on the other, use different reference scales – a fact LOINC would have to consider. In turn, this poses a problem for the patient’s electronic health record (EHR), since the laboratory values a GP gets from lab partners are established using methods that are different from those used in a hospital where in-patient samples are processed in a central lab.
The consequence is painful: to exclude possible misinterpretations, the GP data and the hospital data must be entered seperately within the EHR.
ISO standard to harmonise colour codes
A seemingly small item in the lab poses another big challenge: each manufacturer uses different colour codes for their blood collection tube caps, thus creating a major source of error. A new ISO standard aims to harmonise the colours worldwide. In Germany, this caused an uproar: too much work, too problematic, too error-prone. But harmonisation is indeed urgently needed: while there is a cross-check to ascertain that tube content matches the cap colour jive, the use of two different colour codes can throw a spanner in the automated systems. ‘Nobody knows how this will end. There were a decision and a recommendation, but it remains to be seen whether they will be implemented.’ If Sarstedt, a manufacturer of lab and medical technology devices, can deliver next year, all labs across Germany will change colour codes on a set date. This means all devices that check cap colours need to be reprogrammed.
2-D barcodes still in the pipeline
‘In pre-analytics peak times 500 to 1,000 samples need to be processed in one hour,’ says Lichtinghagen. ‘The bulk loader by Sarstedt is the ideal system to handle this volume, since it pre-sorts the samples and automatically places them on the processing track.’ To do this manually would be much too time-consuming.
The higher the degree of automation the more important are precisely placed barcodes. If the barcode is wrong or damaged, the system cannot recognize it and the entire process is stopped instantaneously. In order to register the sample it has to pass the barcode scanner – a task that can be done either manually by the lab staff or automatically by the system which also documents the barcode. If the tubes are sent by a pneumatic system, the sample might end up in the inbox without being further processed for hours. Sarstedt is in the process of developing RFID barcodes that are inside the tube and read by sensors. Thus the tubes can be tracked faster and more precisely which will no doubt positively affect sample and analytics quality.
Profiles:
Professor Ralf Lichtinghagen is Deputy Director of the Institute for Clinical Chemistry and Director of the MTLA-School at Hanover Medical University, Germany. His main research is on the molecular diagnosis of malignant diseases, liver fibrosis, MS and stroke. He is a member of the DGKL.
Biologist and clinical chemist Martin Christmann works at the Institute for Clinical Chemistry at Hanover Medical School. He is a member of the German Society for Clinical Chemistry and Laboratory Medicine (DGKL).
23.04.2020