Article • Infection control
Knowledge is one thing - implementation another
Insufficient knowledge of infection control, resulting in insufficient compliance, increases the risk of hospital acquired infections (HAIs) and multiresistant pathogens that put patients at risk. At the 2019 Annual General Meeting of the German Society for Hygiene and Microbiology e.V. (DGHM) in Göttingen, Professor Frauke Mattner, Senior Consultant at the Institute of Hygiene, Kliniken der Stadt Köln GmbH (Cologne Hospitals Group), spoke of the difficulties in implementing infection prevention and control measures in daily routine.
Report: Beate Schenk
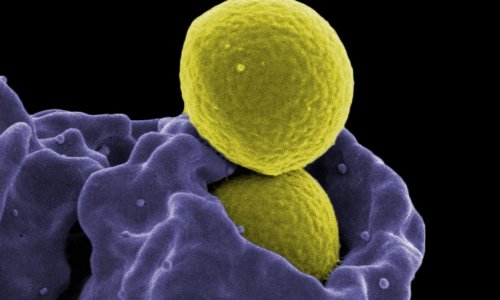
Most hospital pathogens that cause infections are already carried by patients – and mainly Staphylococcus aureus, the most dangerous among the numerous Staphylococci. These bacteria are transmitted via direct and indirect contact with those who are colonised or infected, or through contact with contaminated objects. Staphylococcus aureus is found in the nasal passages of around 30% of healthy adults. Colonisation of the skin is much less common. People whose skin is repeatedly pierced or torn have an increased risk of developing an infection caused by this bacterium. Careful hand disinfection prior to aseptic activities can therefore prevent this type of infection.
Recommended article
News • Superbug MRSA
Unlocking the secrets of Staph's immune bypass
For years, medical investigators have tried and failed to develop vaccines for a type of staph bacteria associated with the deadly superbug MRSA. But a new study by Cedars-Sinai investigators shows how staph cells evade the body’s immune system, offering a clearer picture of how a successful vaccine would work.

Hand hygiene, and specifically alcohol-based hand disinfection, is widely known as a key measure of infection prevention. Founded in 2008, the German initiative ‘Action for Clean Hands (ASH based on the World Health Organisation (WHO) initiative Clean Care is Safer Care), promotes hand hygiene on a national level. ASH is a comprehensive training programme for everyone who provides medical care. The objective is a continuous reduction of the infection rate and to steer it below the rates found in comparative reference data. The scheme has helped to significantly improve hand hygiene on many wards in numerous hospitals. However, although knowledge of basic hygiene has improved in German hospitals, the implementation still leaves much to be desired. ‘The implementation of hygiene measures is problematic,’ Professor Frauke Mattner underlines. ‘We know that the new hygiene measures are sound and correct. We also know how to implement them. The difficulty lies in encouraging hospital staff and patients to carry out certain procedures regularly, on a day to day basis, because it means changing their behaviour.’
Recommended article

Article • Antimicrobial resistance
What to do when antibiotics are taken like candy?
The need to do more to combat resistance in Germany was keenly emphasised by delegates at the VDGH (The German Diagnostics Industry Association) event held in Berlin this May. Only the answer, or at least the common will, is missing to bring this threat under control via a concerted concept.
Behavioural change via education
With all the different tasks in daily hospital routine we are still having difficulties with staff awareness around hygiene measures and requirements
Frauke Mattner
Educating patients has also proved problematic. ‘Some are just too ill and not able to understand this to become actively involved in infection prevention,’ Mattner points out. "Nurses must have sufficient time to educate all these patients as to the correct implementation of hygiene procedures.’ The implementation is hampered by a lack of standardisation of patients and diseases. With clearly defined diseases, it would be possible to prepare staff appropriately and integrate hygiene measures into a patient’s daily hospital routine. However, Mattner observes, ‘There is a lack of research and data on how best to integrate patients into the process of infection prevention and on the potential of this patient-focused infection prevention.’
Hygiene instructions should be tracked by doctors and nurses. However, this proves difficult when nursing teams are short-staffed. Preventing the transmission of pathogens from patient to patient via contact with staff members’ hands means that nurses and doctors must carry out disinfection measures in designated areas prior to carrying out aseptic activities. ‘With all the different tasks in daily hospital routine we are still having difficulties with staff awareness around hygiene measures and requirements,’ Mattner explains. But the rules of basic hygiene also offer some relief. ‘Hand disinfection is not required all the time, but specifically where it can prevent the transmission of pathogens and infections.’
The most recent prevalence study from 2016 provides current figures on the extent of HAIs in Germany. ‘Unfortunately we don't know which patients have purely endogenous infections and which have infections caused by transmission through hospital staff.’
The Commission for Hospital Hygiene and Infection Prevention (KRINKO) makes recommendations to prevent nosocomial infections as well as for operational/organisational and structural/functional hygiene measures in hospitals and other medical facilities, all based on the Protection against Infection Act (IfSG). It stipulates that there should be one hospital hygiene specialist for every 400 hospital beds. ‘This is reality for only around 400 hospitals in Germany with access to only just under 70 specialists in hygiene and environmental medicine. Germany has a lack of hygiene specialists due to the very small number of training places. Only seven out of the 35 medical faculties in this country have an independent chair for Infection Prevention, providing training to meet a high demand for specialists. Preventing endogenous infections through basic hygiene remains a big challenge.’
Profile:
Professor Frauke Mattner is Senior Consultant at the Institute of Hygiene at the Kliniken der Stadt Köln GmbH, Universitätsklinikum Witten-Herdecke, Campus Köln-Merheim and Vice President of the German Society for Hygiene and Microbiology (DGHM). She teaches hygiene curricula at the North Rhine Academy of Continuing Medical Education and chairs the Committee for the Prevention of Norovirus Infections at the German Association for the Control of Virus Diseases (DVV). The professor is also a member of the Expert Advisory Board on Influenza at the Robert-Koch-Institute (RKI), and a member of several associations and working groups, including the working group ‘QS NRW’ of the North Rhine Medical Association, the ‘Infection Prevention Initiative’ (IPI) of the German Coalition for Patient Safety, as well as of the European Committee on Infection Control (EUCIC) of the European Society of Clinical Microbiology and Infectious Diseases (ESCMID).
13.04.2019