News • Rare lung disease
FDA approval for scleroderma treatment
The U.S. Food and Drug Administration approved Ofev (nintedanib) capsules to slow the rate of decline in pulmonary function in adults with interstitial lung disease associated with systemic sclerosis or scleroderma, called SSc-ILD.
It is the first FDA-approved treatment for this rare lung condition. “Patients suffering from scleroderma need effective therapies, and the FDA supports the efforts of drug companies that are designing and conducting the clinical trials necessary to bring treatment options to scleroderma patients,” said Nikolay Nikolov, M.D., associate director for Rheumatology of the Division of Pulmonary, Allergy, and Rheumatology Products in the FDA’s Center for Drug Evaluation and Research. “Nintedanib is now a treatment option to slow the rate of decline in pulmonary function in patients who have interstitial lung disease from scleroderma.”
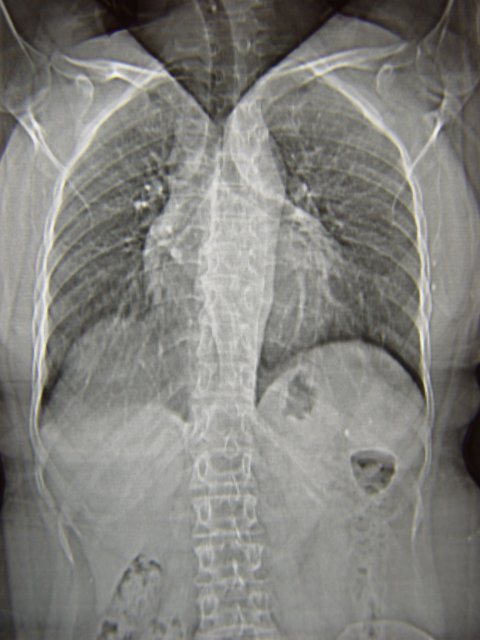
Image source: Nevit Dilmen, Systemic sclerosis case 11 pic 08, CC BY-SA 3.0
Scleroderma is a rare disease that causes tissue throughout the body, including the lungs and other organs, to thicken and scar. Interstitial lung disease or ILD is a condition affecting the interstitium, which is part of the lung’s structure, and is one of the most common disease manifestations of sclerderma. SSc-ILD is a progressive lung disease in which lung function declines over time, and it can be debilitating and life-threatening. ILD is the leading cause of death among people with scleroderma, typically resulting from a loss of pulmonary function that occurs when the lungs cannot supply enough oxygen to the heart. Approximately 100,000 individuals in the United States have scleroderma, and approximately half of scleroderma patients have SSc-ILD.
The effectiveness of Ofev to treat SSc-ILD was studied in a randomized, double-blind, placebo-controlled trial of 576 patients ages 20-79 with the disease. Patients received treatment for 52 weeks, with some patients treated up to 100 weeks. The primary test for efficacy measured the forced vital capacity, or FVC, which is a measure of lung function, defined as the amount of air that can be forcibly exhaled from the lungs after taking the deepest breath possible. Those who took Ofev had less lung function decline compared to those on placebo.
The overall safety profile observed in the Ofev treatment group was consistent with the known safety profile of the therapy. The most frequent serious adverse event reported in patients treated with Ofev was pneumonia (2.8% Ofev vs. 0.3% placebo). Adverse reactions leading to permanent dose reductions were reported in 34% of Ofev-treated patients compared to 4% of placebo-treated patients. Diarrhea was the most frequent adverse reaction that led to permanent dose reduction in patients treated with Ofev.
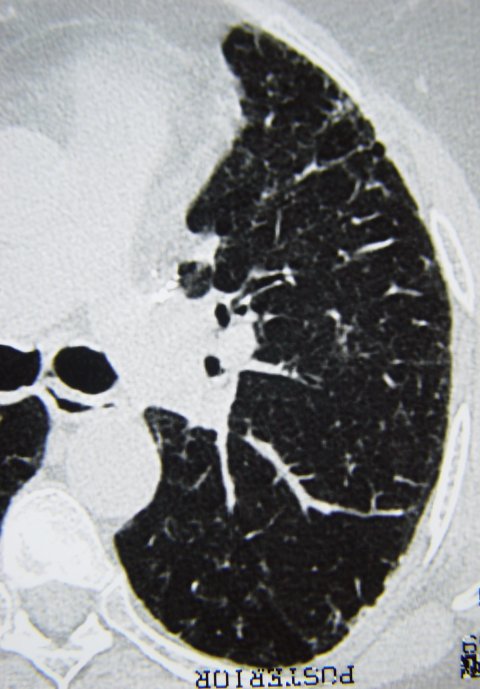
Image source: Nevit Dilmen, Systemic sclerosis case 03 pic 18 cr, CC BY-SA 3.0
The prescribing information for Ofev includes warnings for patients with moderate or severe hepatic (liver) impairment, those with elevated liver enzymes and drug-induced liver injury and patients with gastrointestinal disorders. Ofev may also cause embryo-fetal toxicity that can result in fetal harm, arterial thromboembolic events (blood clots), bleeding and gastrointestinal perforation. P-gp and CYP3A4 inhibitors may increase nintedanib exposure, and patients taking these inhibitors should be closely monitored for tolerability of Ofev. Common side effects noted with Ofev include diarrhea, nausea, abdominal pain, vomiting, liver enzyme elevation, decreased appetite, headache, weight loss and hypertension (high blood pressure).
Ofev was originally approved in 2014 for adult patients with idiopathic pulmonary fibrosis (IPF), which is another interstitial lung condition. Ofev received Priority Review designation, under which the FDA’s goal is to take action on an application within six months where the agency determines that the drug, if approved, would significantly improve the safety or effectiveness of treating, diagnosing or preventing a serious condition. Ofev also received Orphan Drug designation, which provides incentives to assist and encourage the development of drugs for rare diseases.
The FDA granted the approval of Ofev to treat SSc-ILD to Boehringer Ingelheim Pharmaceuticals Inc.
Source: U.S. Food and Drug Administration (FDA)
09.09.2019