Article • Diverse benefits
Experts present CEUS insights
In April 2016 CEUS received the USA’s FDA approval. This year‘s RSNA Samsung Symposium ‘Contrast-Enhanced Ultrasound (CEUS): Innovations and a Problem-Solving Tool in Clinical Practice’ provided an opportunity to take stock. For European Hospital, Professor André Clevert, Director of the Interdisciplinary Centre for Ultrasound at University Hospital Munich, Germany, describes the current state of affairs and ventures a guess regarding the future of this technology.

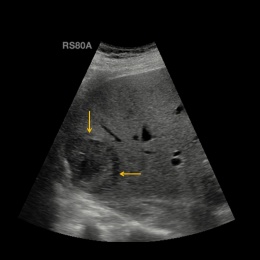
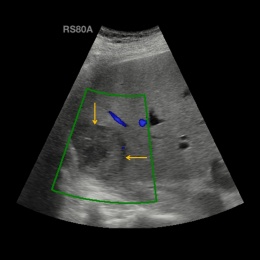
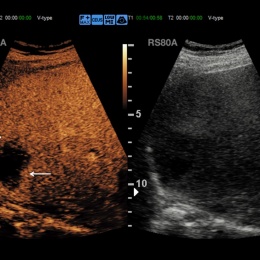
‘Today, it’s safe to say, the advantages of CEUS, particularly in paediatrics, are obvious, as Paul Sidhu, Professor of Imaging Sciences at King’s College London and President of the British Medical Ultrasound Society, clearly showed in his presentation. Since April 2016, when microbubbles were approved for liver diagnostics in children, the range of diagnostic options has broadened,’ Professor Clevert points out. CEUS is important in trauma diagnostics to detect liver injuries or liver haemorrhage; moreover it facilitates the precise description of liver lesions.
The second presentation, by Professor Stephanie Wilson, Clinical Professor of Radiology at the University of Calgary and member of the Diagnostic Imaging Department at Foothills Medical Centre, focused on benign lesions and their changes over time.
‘She was able to show in case studies that contrast-enhanced imaging as an additional diagnostic tool offers reliable and fast results,’ says Clevert, who adds, ‘With CEUS waiting times can be reduced and patients can undergo further diagnostic procedures right after abdominal sonography.’
Deep insights
The final presentation on CEUS advantages examined ‘the different forms of hepatocellular carcinoma (HCC), from rather rare lesions in the non-cirrhotic liver to mixed HCCs, such as cholangiocarcinoma (CCC), plus HCC. Whilst a CCC, as such, cannot yet be differentiated in ultrasound, a biopsy will tell whether a bile duct carcinoma is present, or a CCC plus HCC,’ Professor Clevert explains.
However, CEUS does not only play an important role in HCC diagnosis; it is also extremely helpful in evaluating treatment response, as Professor Clevert points out: ‘There are several intervention options for HCC – from transarterial embolisation (TAE) and transarterial chemoembolisation (TACE) to radiofrequency ablation and microwave ablation. All these therapies need adequate follow-up and assessment whether a vital residual tumour is present post-surgery. This is easy to ascertain with CEUS.’
A very rare variant of HCC, the fibrolamellar hepatocellular carcinoma, can occur in young women without coexistent liver disease. This is, as Professor Clevert explains, ‘a tumour originating in the liver in younger patients without liver cirrhosis. The tumour usually remains a singular mass in the liver but metastasises to the lymph nodes. The origins of these tumours have not yet been fully researched; genetic disposition cannot be excluded.’
Above and beyond the liver
Today, plaque evaluation is done by CT, which, however, cannot confirm vascularisation of plaque. This is where CEUS might come in.
Professor Dirk-André Clevert
At the RSNA symposium, Professor Vito Cantisani from Policlinico Umberto I, Sapienza University in Rome, Italy, looked at CEUS fields of application beyond the liver, such as the evaluation of plaques. ‘Today,’ Clevert explains, ‘plaque evaluation is done by CT, which, however, cannot confirm vascularisation of plaque. This is where CEUS might come in.’ ‘Other presenters at the symposium shared their CEUS experience in terms of vessels, kidneys, and other organs.
A crucial advantage of CEUS is the fact that, in many cases, changes can only be made visible by administering contrast agents. For example, when an aortic stent has been placed, conventional techniques carry a 30 percent risk that endoleaks are not detected. As far as kidneys are concerned, the diagnosis of kidney cysts is so complex that only contrast media allow precise and fast confirmation of carcinoma or cyst,’ Clevert points out.
CEUS – the future
A lot of work remains to be done!
Professor Dirk-André Clevert
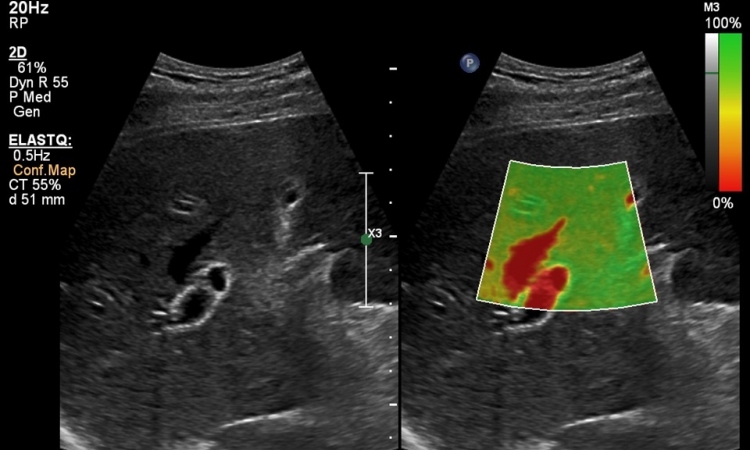
‘No doubt, we’ll see an expansion of ultrasound diagnostics and a clear focus on multiparametric imaging,’ Clevert predicts. ‘A major item on our wish list is the display of numeric values in multiparametric imaging for us to be able to detect temporary changes early on and initiate targeted treatment,’
Artificial Intelligence and Machine Learning, major issues at this year’s RSNA, present particular challenges for ultrasound, as Clevert knows. ‘Sonography generates huge data volumes since we are dealing with moving images rather than stills. Consequently, in a first step, an image documentation standard has to be defined for the system to be able to learn anything at all. Furthermore the tumour classifications “benign” and “malignant” will not be sufficient to obtain valid results. A lot of work remains to be done!’
Profile
Professor Dirk-André Clevert began his career at the MRI Diagnostics Institute Westend in the city of his birth, Berlin, Germany, and in the Department for Internal Medicine at the Waldkrankenhaus Gransee. He then worked as a specialist registrar in the Department of Radiology at Passau Hospital for three years. In 2003, he moved to Munich to join the newly founded (2004) Interdisciplinary Centre for Ultrasound at the Grosshadern Campus, University Hospital Munich. The centre coordinates all ultrasound activities in the hospital. As course director and congress president, he organises numerous national and international ultrasound courses and congresses. On the 80th founding anniversary of the Medical Faculty of Tbilisi State Medical University, as head of the Interdisciplinary Ultrasound Centre, the professor was awarded an honorary doctorate.
29.01.2018