ECR delivers new findings and key updates on DBT's potential
By Rob Skelding
Delegates at the 2009 European Congress of Radiology (ECR) saw a series of presentations Friday unveiling new findings and key updates on digital breast tomosynthesis (DBT). As the body of research builds in this relatively unexplored field, the advantages and limitations of DBT compared with conventional full-field digital mammography (FFDM) and other modalities are becoming better defined.
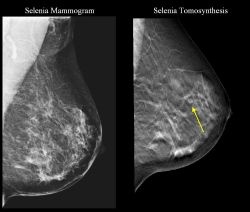
In the first of three key studies comparing the clinical performance of the two technologies, plus ultrasound (U/S), Daniel Förnvik of [where?] discussed a study that assessed their comparative performance in measuring breast cancer size.
In theory, DBT would overcome the limitations of conventional 2D FFDM which suffers from anatomical noise created by superimposed breast structures, thereby obscuring a tumor line.
In the study, FFDM was performed using CC and MLO views while a prototype DBT system generated the 3D (DBT) data. The work was a collaborative effort with Siemens Medical Systems.
Patients comprised 65 women identified by FFDM as having subtle but suspicious signs of breast cancer, or were symptomatic with subtle or negative findings on FFDM but suspicious lesions on U/S.
Experienced radiologists without knowledge of the pathology results measured mass sizes using DBT, FFDM and U/S independently, using scatter plots and linear regression to produce predictive R2 statistics.
Results showed that tumor outline could be determined in significantly more cases with DBT (84%) and U/S (83%) than FFDM (51%). DBT also had the highest correlation with pathology (R2 = 0.66, versus 0.49 for U/S and 0.47 for FFDM), and performed better when sizing smaller tumors.
“It was much easier to outline the tumor using DBT than FFDM, and is therefore superior in the appropriate staging of breast cancer,” said researcher Förnvik. “DBT also had the highest proportion of measurable tumors, though it can be considered as complimentary to U/S.”
Certain tumors were measurable only with DBT, and other only with U/S. In conclusion, Förnvik suggested that due to the increasing use of breast-conserving surgery DBT’s superior cancer sizing capability could improve diagnosis and care in the clinic.
In a major update to ongoing work, Gisella Genaro, of the Oncological Institute of Veneto (IRCCS), Italy, presented her latest research on 200 patients from a blinded multi-reader (six radiologists) study of 2-view FFDM versus 1-view DBT. At ECR 2008, she presented preliminary findings on 50 patients, from three radiologists.
The expanded data set, which included women with breast lesions classified by mammography and/or U/S as doubtful or suspicious. Six experienced radiologists reviewed left and right breasts of each patient individually, with clinical assessments from each reader compared against conclusive pathology results.
Findings were identified, localized and rated according to the ACR 7-step BI-RADS scale. MRMC ROC analysis was applied to data on a total of 371 breasts, with areas under the ROC curves across radiologists for FFDM and DBT compared.
There was slightly lower variability with DBT than FFDM, however it was not significant at 95% confidence intervals. Areas under ROC curves (AUCs) for detecting breasts with malignant lesions were 0.884 (DBT) versus 0.852 (FFDM). Similar results were obtained for breasts with benign lesions (0.857 versus 0.845).
“We found that the overall clinical performance of tomosynthesis in 1-view was not significantly different from FFDM in 2-views,” Gernaro concluded. “We can say that in this study population, tomosynthesis in 1-view was shown to be non-inferior.”
The DBT prototype used was an enhancement of a standard FFDM unit, GE Healthcare’s Senographe DS), modified to acquire multiple projections over a limited arc. In this case, it produced 15 projections over a 40-degree arc.
Genaro commented that doses given were in accordance with European guidelines, directing acceptance limits as a function of breast density.
In a third presentation on developments in DBT, Andrew Smith, director of imaging science at Hologic (Bedford, MA), brought fresh findings from his work assessing radiologist performance variability with DBT (combined 3D+2D data) versus FFDM (2D data alone).
In this study, 27 radiologists used BI-RADS and probability of malignancy (POM) metrics to assess 310 cases, taken from 1,000 patients. The sample comprised normals, recalls (women recalled after screening but subsequently dismissed), women with benign lesions identified with biopsy, plus 51 cancers.
Performance was measured using ROC curves and recall rates for screening cases – variability for AUCs and recall rates was studies separately for 2D and then 2D+3D. This analysis was performed for all images and subsets involving masses and calcifications.
The 27 readers were experienced in reading FFDM images but undertook a training course in DBT. “Superficially, these images look quite like mammograms but there is a certain expertise needed to read them efficiently,” Smith noted.
Results showed that all readers had an improvement using 2D+3D data versus 2D alone. However, the variance (or standard deviation) under the ROC curve for 2D+3D was 72% vs 2D alone, which was not statistically significant (p=0.11). In a subgroup with calcifications, there was no significant improvement in 2D+3D vs 2D alone.
In a group without calcifications – but where lesions and architectural distortions were present – variance for 2D+3D was a statistically significant 62% (p=0.02).
On decisions to recall in non-cancer cases, Smith found that 71% of radiologists agreed using 2D (FFDM) alone compared with 79% using 2D+3D data. Therefore, there was a statistically significant in radiologists agreeing what was ‘normal’.
“So we can prove that radiologists are more accurate, as measured by area under the curve, and more confident, as measured by variance, using 2D+3D versus 2D alone, Smith said. “The main goal is pre-cancer detection and this (2D+3D) shows great potential. It’s certainly conceivable and likely that 3D imaging (DBT) will become the standard of care long term”.
07.03.2009