News • Lumacaftor-ivacaftor
Cystic fibrosis patients benefit from drug combination, but...

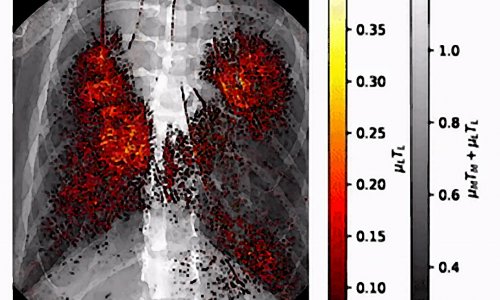
Credit: ATS
In adolescent and adult patients with cystic fibrosis taking lumacaftor-ivacaftor (trade name Orkambi), the combination drug appears to improve lung function and body weight and reduce the need for intravenous antibiotic treatment, according to a French study published online in the American Thoracic Society’s American Journal of Respiratory and Critical Care Medicine.
However, nearly one in five patients could not tolerate treatment, most often due to adverse breathing events, during one year of follow up. The rate of discontinuation was considerably higher than previously reported in clinical trials, the authors wrote. In “Real-Life Safety and Effectiveness of Lumacaftor-Ivacaftor in Patients with Cystic Fibrosis,” Pierre-Régis Burgel MD, PhD, and colleagues report on their study of 845 patients (292 adolescents, 553 adults) who were treated at 47 cystic fibrosis centers throughout France.
Recommended article
News • Cystic Fibrosis & COPD
An experimental treatment for chronic lung disease
Researchers at Queen’s University Belfast have discovered a novel experimental treatment for chronic lung diseases that could improve the lives for people with Cystic Fibrosis (CF) and Chronic Obstructive Pulmonary Disease (COPD).
Cystic fibrosis is caused by mutations in the cystic fibrosis transmembrane conductance regulator (CFTR) gene. In 2015 the Food and Drug Administration and the European Medicines Agency approved lumacaftor-ivacaftor in treating patients who have inherited the same defective CFTR gene, known scientifically as the Phe508del mutation, from their parents. “We felt it was important to obtain real-life post-marketing data in a large population of unselected patients with CF,” said Dr. Burgel, a professor of medicine at Paris Descartes University and a physician at Cochin Hospital, Assistance Publique Hôpitaux de Paris. “Our findings provide a useful complement to randomized clinical trials in which participants were selected based on very strict criteria.”
The study found that patients who took lumacaftor-ivacaftor continuously for 12 months experienced:
- a 3.67 percent increase in their percent predicted FEV1. FEV1 is an important measure of lung function that measures how much air a person can forcefully exhale in one second after a deep breath. Percent predicted compares how well a patient did on the test to how well the same person with healthy lungs would do.
- A weight increase by approximately 2 to 3 kg (4.5-6.5 lbs.).
- A 35 percent reduction in courses of intravenous antibiotics.
The benefits and risks of new therapies cannot be extrapolated to patients who were excluded from clinical trials.”
Pierre-Régis Burgel
The researchers found that 18.2 percent of participants in the study dropped out. According to the authors, this was “markedly” higher than “pivotal clinical trials,” in which less than 5 percent of patients discontinued the combination therapy. Based on their findings, the authors believe the higher rates in the current study were likely the result of enrolling a higher proportion of patients with severe respiratory disease. However, discontinuation rates in patients with milder disease were also three times higher than in clinical trials, presumably because these patients had less stable disease, the authors said.
Nearly half the patients who discontinued treatment did so because of adverse respiratory events and more than a quarter discontinued treatment due to adverse non-respiratory events, most often digestive problems.
Other study findings:
- Patients who discontinued treatment were more likely to have experienced an exacerbation after IV antibiotics in the year before taking the combination drug.
- Adults were more likely than adolescents to discontinue treatment.
- Adults, but not adolescents, who discontinued therapy were at high risk of rapid FEV1 decline, BMI decrease and multiple respiratory exacerbations.
- The combination therapy was associated with a reduction in frequent (≥ 2) exacerbations per year.
“For patients who are able to continue lumacaftor-ivacaftor, there is clinically meaningful improvement in respiratory disease and nutritional status,” Dr. Burgel said. “However, our study found that the benefits and risks of new therapies cannot be extrapolated to patients who were excluded from clinical trials.”
Source: Assistance Publique Hôpitaux de Paris (AP-HP)/American Thoracic Society (ATS)
13.10.2019