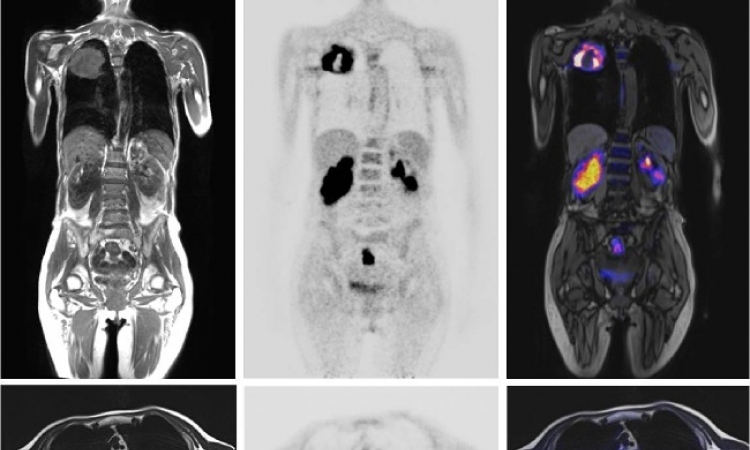
Assessing potential benefits in PET/MRI examination
In recent years, combined examination methods have increased, whereby two examination methods are used in a parallel examination, rather than performed separately. Frederik Giesel MD, Associate Professor of Radiology at the Nuclear Medicine Department, University of Heidelberg, and Philip Herold (Dipl. Econ.), Project Manager at RICT Heidelberg, report on the benefits.

Three major benefits from combined examination methods are expected: First, better exam results for diagnosis and thus increased quality in treatment; next, increased patient convenience by shortening examination time and decreasing the likelihood of poor treatment, and then, cost savings in time, human resources and material, after an initial investment. Such has been the findings in various studies.
This article proposes a comparison not only of combined examination against separate examinations but also an evaluation of the possible benefit of different combinations of examination methods.
For illustrative purposes, PET/MR is evaluated against separate examinations and PET/CT as an alternative combined examination method. The impact is analysed in the TMA staging taxonomy, i.e. lung cancer.
Better exam results
With respect to lung cancer, combined examinations basically deliver output of the same quality in terms of not overseeing lesions as stand-alone methods, such as CT/MRT, bone scan, or mediastinoscopy. Thus the results of all methods shall be treated as equally useful for follow-up examinations.
However, PET/CT has to be complemented by MRT anyway. This is, for example, the case for thorax examinations (T). Because CT cannot provide data of the same quality as MRT for morphological questions, MRT is likely to be done in addition. The best examination result is achieved by including MRT in the combination, for better data quality.
Another example is the examination of remote metastasis in the head (M). As there is a high concentration of glucose in the brain anyway, (FDG-)PET can hardly yield any results suitable for evaluation. CT results are sometimes problematic because of the bone density surrounding the area of interest. Here again, the inclusion of MRT can complement such shortcomings in terms of wider scope of the examination.
Patient convenience
Patients can also benefit from the combination of examinations by experiencing a more comfortable course of treatments, because they only have to attend one appointment, including transportation, paperwork etc. Especially for more severe cases, the number of examinations may significantly drive the overall recovery process.
Increased standardisation and routine help the staff to reduce process time and handle cases more effectively. For example, the time-intensive step of deciding on the appropriate method and eventually revising this decision can be left out. Further economies of scale may occur in the diagnosis routine, as physicians become more specialised and the output (report) naturally more standardised. This in turn also benefits the treating physician.
Cost saving
When it comes to investment decisions cost savings are examined in great detail. These are the one-off cost of investment, on-going cost per examination and equipment maintenance.
In the initial investment no synergies can be realised when switching from separate stand-alone scanners to equipment allowing for combined examinations. The opposite is the case as additional investments have to be made for integration.
However, on an on-going basis, economies of scale may be incurred in the diagnosis-routine because less staff time (human resources) is needed per examination.
Maintenance and related cost may decrease, as specialisation effects increase. This can be sourcing-related in terms of a help desk, for example. This could also be material related, for example, in terms of tracers.
For lung cancer, the German health insurance system covers PET/CT. However, in most cases additional MR examinations are conducted upon prescription by the physician in charge (M lesions above). As a result, all three methods, PET, CT and MR are employed whereas the marginal contribution of CT is rather small. This is only achieved after a lengthy and thus costly administration process between treating clinic and health-insurance. This process and the related cost could be avoided by integrating PET and MR to a standardised routine.
Conclusion: In summary, it can be observed that the combination of established examination methods is beneficial. Such integration increases patient convenience and decreases cost per examination. Most importantly, diagnostic quality can be enhanced as combined methods complement each other and provide the physician with better data.
Among the combined examination methods it turns out that PET/MR is superior to PET/CT for two reasons. First, MR and PET complement each other in a way allowing for a wider scope of examinations (M lesions above). Second, MR imaging was found to be more relevant than CT (T lesions above). These two reasons are to be traded off against the additional cost upon investment.
20.10.2011