All in one: Hybrid imaging with MR/PET
Although like a conventional MR scanner the unassuming exterior is misleading. The casing houses a powerful interior. This is the new Siemens Biograph mMR, a hybrid that contains a specially developed PET component fully protected against magnetic field interference.
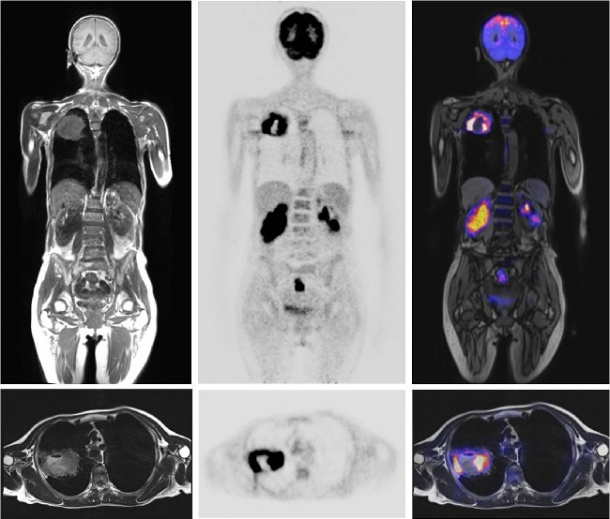
The first clinical installation of the MR/PET was completed in Munich last November. Five others have followed – four in Germany, one in Boston, Mass.
The technical evaluation of the system is taking place at the Department of MR Imaging at the Institute of Medical Physics at Friedrich-Alexander University Erlangen-Nuremburg, supervised by physicist, engineer and head of the department Professor Harald Quick. Speaking with European Hospital, he outlined the expectations and challenges of the MR/PET technology.
In April 2010, the Siemens MR/PET equipment was installed at the Institute of Medical Physics (IMP) in Erlangen-Nuremburg, giving its team an early start for clinical studies to evaluate the method. ‘We began with a group of 50 patients who underwent a standard PET-CT examination, followed by an MR/PET scan,’ explained Professor Harald Quick. ‘The participants were exposed to neither increased radiation nor increased dose. Since the radio tracer was injected only once, the activity was slightly reduced by the time the participants were ready to undergo the MR/PET scan, but we compensated this fact by simply doubling the PET examination time.
‘The device can obtain PET and MR images simultaneously rather than subsequently which significantly reduces examination times. PET data are acquired in the background. We aimed at performing a whole body scan with all sequences, from head to knees, in 30 minutes. Certainly specific localised examinations can be performed more quickly, or they can be added to the whole body protocol.
Evaluation questions
‘We looked at very different aspects,’ the professor points out. ‘Do we see the same as in PET or do we see more, or less? Are the MR and PET data fused correctly?
‘We therefore performed many technical experiments prior to the actual study. For example, we tested the method first with phantoms whose structures were known. But the crucial question was obviously whether the method as such works. For me, as a physicist and engineer, it was particularly interesting to see how well PET fares in the “physically hostile” MR environment. Can it provide results that are comparable to PET-CT without deviations or disturbances? Thus far we can tell that the integration of MR and PET components was successful.
The team is now in the process of analysing the data. ‘We focused our research on oncological issues. Possibly soft tissue tumours or metastases can be visualised much better in MR/PET than in PET-CT. This would mean that we can reliably detect lesions in organs such as the liver or brain, but also in high contrast bones, which do not show significant soft tissue contrast in PET-CT imaging.
‘Moreover MR/PET offers the ability to monitor breathing and heartbeat during the scan. Currently, we are trying to implement motion corrections in PET using MR data. They will allow us to visualise lesions precisely. We could also determine the exact quantity of tracer that accumulates in the lesion, which we cannot do if the lesion moves during the scan -- and we cannot do this in PET-CT because we must not expose the patient to longer CT radiation only to detect motion patterns.
Acquisition
‘Since every patient has an individual breathing pattern which changes during the examination, we will register this pattern in real-time or with a breathing belt. This information can be recorded at any time, let’s say within a time span of three minutes. Later on, we reconstruct the three-dimensional PET data that were thus acquired. Consequently, we do not have a static image but a dynamic one, which allows us to observe the lesion’s motion during breathing. That requires enormous computing power. We already have the necessary data and it’s now the task of the developers to fine-tune the application.
Will MR/PET replace PET/CT in the long run? ‘No, PET-CT is here to stay,’ he believes ‘Above all in the beginning, factors such as speed, availability and costs will play a major role. Since MR/PET is a time and cost intensive modality, patient selection should be done very carefully and only those patients who benefit most from MT/PET should be scanned. Furthermore, for thorax and lungs we’ll continue to need PET-CT to visualise small lung cancer tumours and lesions. Not to forget that PET-CT can be used for patients who currently cannot undergo an MR/PET examination, for example those who have a pacer implant. Nonetheless, MR/PET will surely become a fixture as an additional diagnostic imaging modality in oncology, cardiology and neurology. In research it is already established.’
Details: www.imp.uni-erlangen.de/mri
26.10.2011
- imaging (1667)
- medical technology (1569)
- MRI (845)
- PET/CT (189)
- PET/MR (77)
- radiation protection (187)
- thorax (76)