Image source: Unsplash/Danilo Alvesd
Article • Drug dose optimisation
Antibiotics: no more ‘dosing in the dark’
Antibiotics are essential for keeping bacterial infections in check, but finding the right dose is akin to a Goldilocks problem: give too little, and the infection will persist; too much, and side-effects will override the benefits of the therapy. To get it “just right”, Prof Dr Birgit Koch will talk about dosing optimisation in the clinical setting at this year’s ECCMID in Lisbon. We spoke with the Clinical Pharmacologist from Erasmus MC, Rotterdam, ahead of the congress about the shortcomings of current methods and the benefits of patient-tailored dosing.
Report: Wolfgang Behrends
‘The concept of “a lot helps a lot” clearly does not apply,’ the expert points out: ‘The higher the dose is, the more the toxicity of a drug becomes an issue.’ Furthermore, incorrect dosage encourages resistance-building in pathogens, and excessive prescription is not a sustainable, cost-effective practice. ‘This is why dose optimisation is so important.’

Image source: private
But getting the dosage of antibiotics right is a challenging matter, Prof Koch says: ‘There is a range of factors that play a role. As a rule of thumb, anything that affects a patient’s metabolic function should be considered, so the most important parameters are age, gender, and renal function.’ Albumin levels in the blood are also relevant, as are pre-existing conditions and medication. ‘Some antibiotics are metabolised by the kidneys, others by the liver – this is important when a patient is under nephrotoxic medication, for example.’ Lastly, the type of targeted microorganism should be considered, as some antibiotics are more effective against certain bacteria than others.
Models in need of greater diversity
Limited knowledge about a drug’s pharmacokinetic (PK) and pharmacodynamic (PD) properties can add another layer of difficulty: ‘Unfortunately, no PK/PD models exist for most drugs developed before 1995,’ Koch reports. This includes antibiotics that are still in widespread use, such as amoxicillin. But even for newer drugs, PK/PD models often lack heterogeneity in patient data. ‘A lot of times, references are only based on effects in young male persons – which is obviously not the primary patient group to receive these drugs in real life.’
We hope that we will see more model informed precision dosing arrive in the clinical practice in the future
Birgit Koch
These shortcomings often lead to every patient receiving the same antibiotic dosage – regardless of individual risk factors. ‘We have discovered that for some beta-lactam antibiotics, most patients receive the same dose, but only 60% achieve site exposure,’ the pharmacologist states. In other words, the drug does not reach its target area in the intended quantity.
To establish more nuanced dosage models, researchers at Erasmus MC took a closer look at the blood of patients in the centre’s ICU. By thoroughly analysing the samples, the team gained insights into how drugs were metabolised by different patient groups. ‘We were able to relate certain factors to positive or negative outcomes,’ Koch reports. ‘For example, impairment of renal function – due to advanced age or disease – affects the rate in which a drug is cleared from the blood. We identified several of these risk factors for target non-attainment, so patients with these risk factors need to receive an adjusted antibiotic dose.’
AI to create more detailed connections
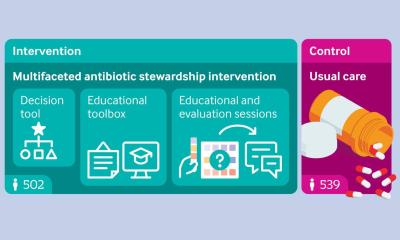
While the benefits of individualised drug dosing might seem rather self-evident, scientific evaluation of the concept is surprisingly sparse. The recently completed DOLPHIN trial is an effort to provide evidence and encourage clinical application of patient-tailored dose models, the expert says. In the Dutch multicentre, prospective, randomised study, outcomes were compared between critically ill patients whose medication dose was monitored and adjusted to reflect individual factors and patients who received the standard dosage. ‘We hope that we will see more model informed precision dosing arrive in the clinical practice in the future,’ says Prof Koch, who will present the findings of the trial at the ECCMID congress.
The expert also regards AI as a key technology to create increasingly complex and sophisticated models. ‘What is especially promising is that algorithms are not biased the way humans are. Because the AI will only process the raw data without knowing the context, it may establish correlations and identify risk factors that a human would have missed.’ This can also help finding new therapeutic options for patients who do not respond to treatment as predicted. Prof Koch also advertises the practice of infection site measurement, which should replace current blood analysis to ensure more targeted results. ‘We still have a lot of work to do,’ she concludes, ‘but getting the right drug in the right dose to the right patient could solve a lot of our current problems, so it’s clearly worth the effort.’
Profile:
Prof Dr Birgit Koch is a Clinical Pharmacologist and Full Professor of Clinical Pharmacometrics at the Erasmus University Medical Center, Rotterdam, the Netherlands. She focuses on Therapeutic Drug Monitoring (TDM), PK/PD and Toxicology and is also part of the management team of the pharmacy. The laboratory covers more than 70.000 TDM/toxicology samples per year and more than 100 assays, both in clinical care and in research. She authored more than 150 publications on PK/PD, TDM and toxicology and is the principal investigator of several studies on model-based dosing, TDM and PK in antibiotics and antipsychotics. Since January 2020, Prof Koch is head of Research & Teaching of Pharmacy Erasmus MC.
23.04.2022