123
Earlier detection of Down’s syndrome
Down’s syndrome (also referred to as trisomy 21) is a genetic disorder caused by the presence of all or part of an extra copy of chromosome 21 in a person’s DNA. Current screening for Down’s syndrome and other trisomy conditions includes a combined test done between the 11th and 13th weeks of pregnancy.
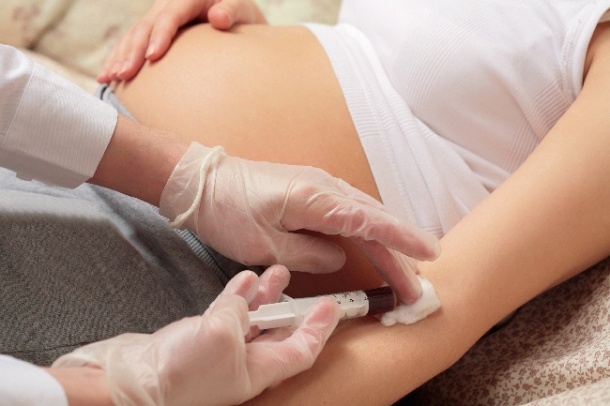
This involves an ultrasound screen and hormonal analysis of the pregnant woman’s blood. Methods such as chorionic villus sampling (CVS), which involves taking cell samples from the placenta, and amniocentesis (sampling amniotic fluid), are also used to detect abnormalities but both are invasive and carry a risk of miscarriage.
Led by Kypros Nicolaides, Professor of Foetal Medicine, researchers from King’s College London and King’s College Hospital have developed a new test that they report can be given earlier in pregnancy and is more accurate than current checks. Their findings have been published in two papers in the journal Ultrasound in Obstetrics & Gynaecology.
Several studies have shown that non-invasive prenatal diagnosis for trisomy syndromes using foetal cell free (cf) DNA from a pregnant woman’s blood is highly sensitive and specific, making it a potentially reliable alternative that can be done earlier than the current screening for the condition. With colleagues, the King’s researchers have now demonstrated the feasibility of routine screening for trisomies 21, 18, and 13 by cfDNA testing.
Testing done in 1,005 pregnancies at 10 weeks had a lower false positive rate and higher sensitivity for foetal trisomy than the combined test done at 12 weeks. Both cfDNA and combined testing detected all trisomies, but the estimated falsepositive rates were 0.1% and 3.4%, respectively. Professor Nicolaides: ‘This study has shown that the main advantage of cfDNA testing, compared with the combined test, is the substantial reduction in false positive rate. ‘Another major advantage of cfDNA testing is the reporting of results as very high or very low risk, which makes it easier for parents to decide in favour of, or against, invasive testing.’ A second Ultrasound in Obstetrics & Gynaecology study by the group, which included pregnancies screening at three UK hospitals between March 2006 and May 2012, found that effective first-trimester screening for Down’s syndrome could be achieved by cfDNA testing contingent on the results of the combined test done at 11 to 13 weeks. The strategy detected 98% of cases, and invasive testing was needed for confirmation in less than 0.5% of cases.
The research team concluded that screening for trisomy 21 by cfDNA testing contingent on the results of an expanded combined test would retain the advantages of the current method of screening, but with a simultaneous major increase in detection rate and decrease in the rate of invasive testing.
Profile:
Kypros Nicolaides is Professor of Foetal Medicine at King’s College London. His research interests are on foetal medicine with special reference to haematology, and on pre-term diagnosis of chromosome abnormalities. At King’s College Hospital, Prof. Nicolaides also heads the Harris Birthright Research Centre for Foetal Medicine, a leading clinical unit and research centre for the assessment and treatment of unborn babies, caring for more than 10,000 patients annually.
19.12.2013