Infections
World still “grossly underprepared” for infectious disease outbreaks
The world remains “grossly underprepared” for outbreaks of infectious disease, which are likely to become more frequent in the coming decades, warn a team of international experts in The BMJ today.
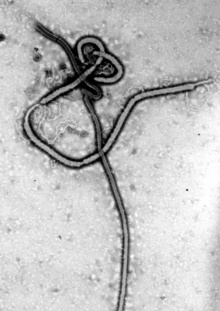
They reviewed reports on the recent Ebola virus outbreak in West Africa and say better preparedness and a faster, more coordinated response could have prevented most of the 11,000 deaths directly attributed to Ebola and also the broader economic, social, and health crises that ensued.
In August 2014, the World Health Organization (WHO) declared the Ebola outbreak in West Africa a Public Health Emergency of International Concern (PHEIC), and the world scrambled to respond.
In the aftermath, a number of reports were published reviewing what went wrong and how we should better manage infectious disease outbreaks. However, the main priorities emerging from these reports and the extent to which action has been taken on the proposed reforms is unclear.
So a research team, led by Suerie Moon at the Graduate Institute of International and Development Studies in Geneva, synthesized seven major post-Ebola reports and laid out the key problems and recommendations they highlighted.
They also assessed progress to date and identified the biggest gaps between recommendations and action in each area of reform.
They found that, while the reports differed in scope and emphasis, their diagnosis of the key problems and recommendations for action converged in three critical areas: strengthening compliance with the International Health Regulations (IHR); improving outbreak-related research and knowledge sharing; and reforming the World Health Organization (WHO) and broader humanitarian response system.
They found significant efforts beginning to address these issues, but that progress has been mixed with many critical issues largely unaddressed.
For example, they point out that investments in country capacity building have been inadequate and difficult to track, arrangements for fair and timely sharing of patient samples remain weak, and reform efforts at WHO have focused on operational issues but have neglected to address deeper institutional shortcomings.
As the WHO Executive Board gathers this week to shortlist candidates in the running for the 2017 WHO Director-General election, the authors point out that "spearheading institutional reforms is likely to fall to the next director general."
“We found remarkable consensus on what went wrong with the Ebola response and what we need to do to address the deficiencies. Yet not nearly enough has been done,” write the authors.
“Ebola, and more recently Zika and yellow fever, have demonstrated that we do not yet have a reliable or robust global system for preventing, detecting, and responding to disease outbreaks,” they add.
And they urge the global community “to mobilize greater resources and put in place monitoring and accountability mechanisms to ensure we are better prepared for the next pandemic.”
“We will not be ready for the next outbreak without deeper and more comprehensive change,” they conclude.
Source: BMJ press release
02.02.2017