Article • Radiology approach
Watch your back! Spinal imaging in trauma
Spinal trauma imaging is considered one of the most challenging areas radiologists face as they seek to assess the extent of injuries to patients under high pressure. The issue was tackled in detail at the British Institute of Radiology virtual congress by Professor Elizabeth Dick. The spinal imaging specialist focused on different approaches and protocols for a range of levels of spinal injury and discussed how best to assess and image them, which modalities to use, and the key factors to consider.
Report: Mark Nicholls

In her presentation “Watch your back! – an approach to spinal imaging in trauma,” Professor Dick explored imaging of thoraco-lumbar and cervical spine injuries. One of the major challenges, she said, was assessment of the spine’s stability, a crucial prerequisite for safe removal of the cervical collar. Misjudging stability can result in severe consequences, such as progression of skeletal deformation or neurological deficits.
Generally, spinal imaging should be performed on patients who have undergone a relatively high-energy mechanism of injury, Professor Dick said. ‘But there is also a need to be cautious if there is another injury or altered level of consciousness. It is important to get the patient to CT as quickly as possible, ideally within half an hour of arriving in the emergency department.’ She stressed the importance of this timeframe since delays often result in a higher risk of neurological injury.
Number of affected columns as a predictor of stability
To determine spinal stability in thoraco-lumbar injuries, several classification systems may be applied. For many clinicians, the Denis system is the preferred option, based on its division of the vertical body into anterior, middle, and posterior columns. ‘Put simply, if two columns are injured, it is quite likely the patient has an unstable spine,’ Professor Dick said.
Another aspect that has gained relevance in recent years is the posterior ligamentous complex. Consisting of the posterior bony ring and adjacent soft tissues, the structure acts like a tension band which holds the whole spine together, the expert explained. For this reason, injury to the ligamentous complex is associated with a high risk of spinal instability.
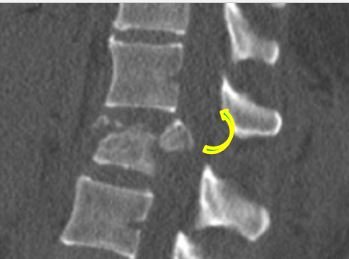
The four thoracolumbar spinal injury patterns are:
- compression fracture;
- burst fracture, which may be a 2 or 3 column injury, with or without retropulsion and neurological damage;
- flexion-distraction or Chance injury, an unstable three-column injury which may have an associated abdominal injury, and usually needs intervention; and
- fracture dislocation, such as from someone falling from height, with unstable spine and a high likelihood of neurological deficit.
Professor Dick added: ‘Burst fractures can be stable or unstable. If a patient has a neurological deficit, that would indicate the need for surgery. The radiologist can help by identifying various signs on CT, such as severe loss of height of the vertical body, retropulsion, kyphosis and rotational malalignment.'
The ‘golden rules’ of spinal MRI
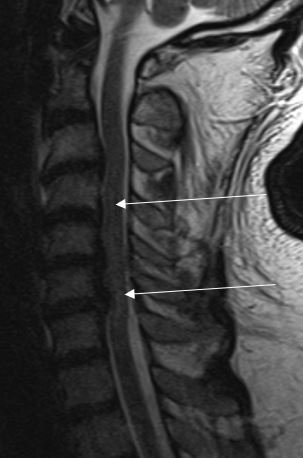
For MR imaging, the expert also gave two “golden rules”: the importance of a T2 fat saturated imaging sequence, and imaging of the whole spine; ‘because if someone has one spinal fracture, they are likely to have a second one as well, so it is important to make sure all of the injuries are detected,’ she stressed. These rules are especially important since patients with severe injuries are difficult to get into the scanner in the first place, so any scan should be performed properly the first time.
Professor Dick also outlined the TLICS (Thoraco-Lumbar Injury Classification and Severity) score for determinants of injury covering fracture morphology, integrity of posterior ligamentous complex and the neurological status of the patient. ‘It is useful to be aware of this as two out of the three components are based on radiology,’ she added. Furthermore, she stressed the importance of early imaging for patients with thoraco-lumbar spine injuries, with CT being the primary modality, followed by MR whole spine imaging.
For children, different rules apply
For patients with cervical spine injuries, Professor Dick advised moving from the anterior to posterior during the examination. Additionally, routine CT in major trauma should be chosen over plain film, with imaging of the entire cervical spine in all planes being of great importance as well. ‘In major trauma in general, a routine whole-body protocol should be performed to image the entire patient each time,’ she said. ‘That way, all the injuries will be included, and the image can be reviewed in a very structured and disciplined fashion, to maximise chances of picking up every injury.’ She concluded that promptly and thoroughly executed whole body CT has in important role in improving patient survival. The use of CT angiograms may also be considered to identify injury of the vertebral artery early, so patients can be anticoagulated to decrease the risk of stroke.
However, the aforementioned guidelines only apply for adult patients, Professor Dick cautioned, as the rules on imaging the spine in children are very different: if possible, CT imaging should be avoided because of the long-term radiation risk and should only be considered if there is a strong suspicion of injury.
Profile:
Professor Elizabeth Dick is a consultant radiologist and Professor of Practice at Imperial College NHS Healthcare Trust with expertise in body MRI, emergency, trauma, and musculoskeletal radiology. At Imperial College Healthcare she was Head of Trauma radiology and is Associate Director of Medical Education. She is past-President of the European Society of Emergency Radiology and of the British Society of Emergency Radiology. Her research interests include trauma imaging, medical education, and digital learning.
29.11.2021