Sensors facilitate rehabilitation at home
European doctors and scientists are working on the StrokeBack project, a medical system aimed at supporting stroke patients in their rehabilitation. Modern technology helps affected patients to practise their mobility at home.
The telemedical system records the training units and saves them in an electronic patient file, and a therapist monitors the data and gives the patient personal advice on how they can train more effectively. Report: Susanne Werner
Every year more than two million people in Europe suffer a stroke. Those affected lose part of their physical and cognitive abilities – at least temporarily. Although around two thirds of patients will be able to return to their normal lives, many will be left with partial disabilities and often lose some quality of life. Some projections calculate that the number of stroke patients will triple over coming decades. Result: Healthcare systems across Europe should prepare for the provision of adequate care and the most effective use of funds. So, what might future successful stroke patient rehabilitation be like?
Movements are recorded The Leibniz-Institute for Innovative Microelectronics (IHP) in Frankfurt (Oder) is currently working on a solution, with scientists developing a new telemedical care concept in cooperation with other European project partners. This solution aims to make stroke patients exercise at home rather than in a rehabilitation clinic – and without any loss of medical or treatment quality. This is made possible with the help of an IT system that monitors patients around the clock.
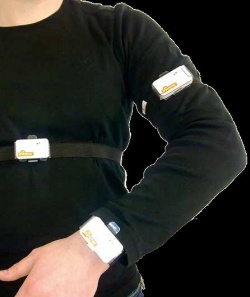
The central concept: Patients wear wireless sensors on the chest, upper arm and wrist of the affected side of the body, during their daily activities as well as during exercise. The sensors capture vital parameters and record movement sequences, which are then transmitted to a telemedical system. The personalised electronic patient file (ePA), which is part of this system, is therefore constantly fed information on a patient’s overall health status and activities. ‘StrokeBack does not replace direct contact with a therapist but fills the gaps in care, for instance the time between two out-patient appointments,’ explains Dr Steffen Ortmann, Technical Project Manager at IHP.
The project’s central building block is the telemedical prototype currently in development under the direction of the Institute. The scientists have based their work on the Microsoft Kinect camera system and they are developing the portable sensor system alongside it. The objective is the ability to record much more detailed data than is possible with the Kinect technology alone. The patient receives his instructions directly via a monitor or TouchPad. The system monitors the exercise programme and reports if activities are not carried out correctly. The time of flight camera technology creates a silhouette of the real patient and their movements.
‘Our system will facilitate very individualised training. A physiotherapist records certain exercises with the patient. The patient then practises these exercises at home and can check himself based on the existing recordings,’ Dr Ortmann explains. When the patients wear some of these sensors during their daily activities the system also records movements during daily activities. It checks range, precision and intensity of these daily movements, enabling conclusions as to the effectiveness of treatment.
Dr Ortmann: ‘The system we are aiming for will enable patients to contribute a lot more towards their rehabilitation than is currently possible, without having to miss out on instruction from therapists. Additionally, it supplies the medical experts with information on individual processes, which has previously not been available, and so contributes to a better understand-ing of the rehabilitation process, its speed and quality. We hope this will enable us to contain costs whilst increasing patients’ quality of life.’ Among the project partners is the Berlin-Brandenburg Clinic in Bernau, which annually treats more than 1,500 stroke patients, and also the United Kingdom’s University of Southampton.
Jane Burridge, Professor of Restorative Neuroscience at the university’s medical faculty, has been researching for years how to make the treatment of strokes more effective and efficient. She combines current knowledge from the world of health psychology with the findings from computer technology and signal control. For the StrokeBack project the professor is its expert on the neuroplasticity of the brain as well as on motoric control, and she contributes her knowledge of psychosocial factors in the healing process. ‘Research for Science, Art and Technology Ltd’, from Sheffield, is another United Kingdom project partner involved in the technology development. Last spring, the UK partners visited the clinic in Bernau to record the first test series with patients.
Another project partner in Brandenburg is MEYTEC Informationssysteme in Werneuchen, a firm specialised in the development of telemedical systems. Intracom Telecom, a Greek company, is tasked with the development of a personalised electronic patient file based on the specifications provided. The IHP also cooperates with the University of Pannonia in Hungary, which has extensive experience in the development of virtual user interfaces. Total funding is €4.3 million, €3 million of which has been provided by the EU, and the research project is scheduled for completion in Semptember 2014.
12.11.2012