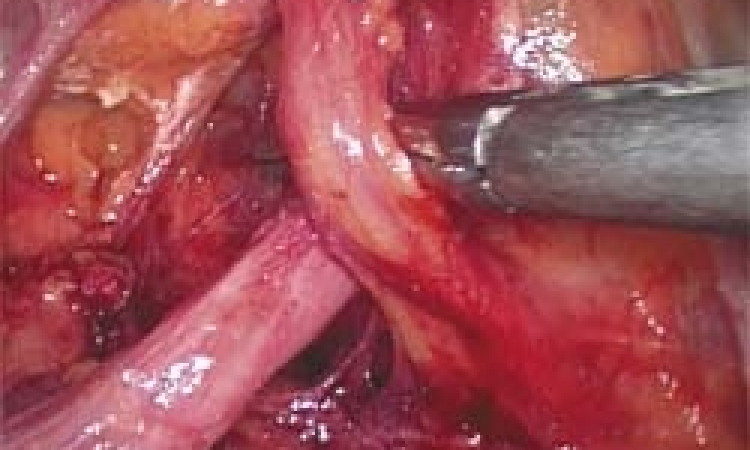
Robot-assisted prostatectomy in practical use
At the Medizin Innovativ 2008 congress (9-10 July, Nuremburg, Germany) Professor Jens-Uwe Stolzenburg MD (right), Director of the Urology Clinic and Polyclinic at the University Hospital Leipzig, talked about his experiences with the da Vinci robot. Used by surgeons at University Hospital Leipzig since last October 2007, they performed 40 operations in the first two months.

The da Vinci technology has been under development since 1995. Over the last three or four years, robot-assisted surgery has replaced the open retropubic prostatectomy as standard surgical procedure for prostate cancer in the USA. In 2007, 68% of all radical prostatectomies in the US were performed using da Vinci. This percentage has been increasing and is expected to rise even further.
The da Vinci technology, which is a significant further development of laparoscopy, offers a number of advantages. From a workstation, the surgeon controls the laparoscopy instruments in the patient body via three-dimensional optics. Patient-side sterile procedures are no longer necessary and the ergonomically designed workstation reduces the physical stress for the surgeon. The instruments of the da Vinci robot can be moved in six increments. Thus, the movement of the surgeon’s fingers are directly transferred to the instruments and possible tremors are avoided.
It is above all the 3-D optics that allow ideal orientation in the operative field, a significant advantage over traditional laparoscopy, which requires orientation in a two-dimensional space – a fact which poses problems for many, particularly inexperienced, surgeons. In short, the da Vinci technology combines the advantages of laparoscopic access (minimally invasive) with those of open procedures (3-D view, intuitive movements, dexterity).
Robot-assisted surgery, however, requires substantial initial investments and the operating costs are comparatively steep. A system comes with a price tag of around e1.3 to 1.5 million. The annual maintenance costs will amount to approx. e50,000 plus approx. e1,000 to 1,500 per procedure for the instruments. Costs are thus one reason why da Vinci robots are not yet being used widely.
From October 2007 to December 2007 we performed radical prostatectomies in 40 patients using the da Vinci system. The average patient age was 66 years, the average PSA was 11.6 ng/ml. Average OR time, including docking times, was 188 minutes, no transfusions were required. No patient required a conversion (open surgical procedure), no major complications, such as injuries of the rectum, were recorded. Histological analyses had found a pT2 tumour in 31 patients (77.5%) and a pT3 tumour in 9 patients (22.5%). Positive margins were detected in 6.5% (2/31) of the pT2 tumours and 33.3% (3/9) of the pT3 tumours. Catheters were placed on average for 6.1 days.
After three months 77.5% of the patients were fully continent, after six months the rate had increased to 90%. Short-term oncological and functional results are thus highly promising and comparable to the results achieved with endoscopic, extraperitoneal radical prostatectomy (EERPE) which we perform routinely in our hospital.
It remains to be seen whether the da Vinci prostatectomy will yield better long-term results. So far, the international literature does not indicate the advantages of robot-assisted surgery to have long-term impacts on the ‘quality indicators’ of radical prostatectomy such as complications, tumour control, continence or potency.
01.09.2008