Image source: Shutterstock/Magic mine
News • Infrared imaging
New imaging method to detect and monitor liver disease
It’s currently difficult to screen for certain liver diseases and to monitor these conditions once they’re discovered. A team led by investigators at Massachusetts General Hospital (MGH) and the Massachusetts Institute of Technology (MIT) recently developed a non-invasive imaging method that has promising clinical potential to accomplish both goals.
The technique is described in a study published in Nature Biomedical Engineering.
Fat accumulation in the liver—called non-alcoholic fatty liver disease (NAFLD)—is a leading cause of chronic liver disease. “In Western societies, NAFLD’s prevalence is increasing in parallel with rising rates of obesity, and the condition is expected to affect nearly 1 in 2 adults in the United States by 2030,” said co-senior author Rakesh K. Jain, PhD, the Director of the E.L. Steele Laboratories for Tumor Biology at MGH and the Andrew Werk Cook Professor of Radiation Oncology at Harvard Medical School.
Recommended article

News • LITMUS vs NAFLD
Towards better diagnosis and treatment of liver disease
A pioneering European research project designed to develop new diagnostic tests to assess patients with Non-Alcoholic Fatty Liver Disease (NAFLD) has expanded giving access to more patients. Liver Investigation: Testing Marker Utility in Steatohepatitis (LITMUS) funded by the European Innovative Medicines Initiative 2 Joint undertaking, brings together clinical scientists from international…
We hope this research can be translated into the clinic for diagnosing and monitoring chronic liver disease noninvasively
Rakesh K. Jain
Usually diagnosis of chronic liver disease encompasses the removal of liver tissue through a biopsy procedure to accurately assess liver inflammation and fibrosis (i.e. tissue scarring), which are caused by oxidative stress and several other destructive processes. It’s known that oxidative stress can lead to the production of lipofuscin, a “wear-and-tear” pigment in the liver among other organs and cells. Dr. Jain and co-senior author Moungi Bawendi, PhD, the Lester Wolfe Professor of Chemistry at MIT, wondered whether visualizing this pigment through a technique called autofluorescence imaging might help to detect early and late stages of liver disease, NAFLD in particular.
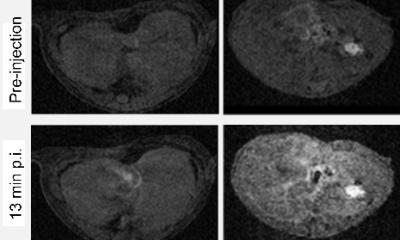
Using near-infrared and shortwave infrared technologies developed by the Bawendi laboratory in combination with animal models widely used in the Jain laboratory to mimic NAFLD, these teams were able to pinpoint areas of liver injury, with clear discrimination between diseased and normal tissues. Detecting lipofuscin in this way also allowed the scientists to non-invasively monitor the progression and regression of liver inflammation and scarring in mouse models of NAFLD, without the need to obtain liver tissue through biopsies.
Also, in biopsied samples of human liver tissue, the imaging modalities could distinguish more severe cases of NAFLD from milder cases. “Preclinically, these methods can be used in animal studies to prevent the need for sacrificing animals at multiple time points. And with further investigations, we hope this research can be translated into the clinic for diagnosing and monitoring chronic liver disease noninvasively,” said Dr. Jain. "Furthermore, this research opens up the potential of non-invasive autofluorescence imaging of lipofuscin in diseases that affect other organs."
Source: Massachusetts General Hospital
24.06.2020