Sponsored • Artificial lungs
Easing ARDS and AECOPD
Innovative ‘artificial lungs’, which help the patients to breathe, offer less traumatic treatment for severe diseases such as acute respiratory distress syndrome (ARDS) or chronic obstructive pulmonary disease (COPD/AECOPD).
Respiratory failure is one of the most frequent causes of ICU admission. It may occur inter alia in patients with ARDS, a dangerous condition when the respiratory system can no longer provide the important exchange of carbon dioxide and oxygen.
Mechanical ventilation
Conventional therapy for ARDS patients, and also for patients with exacerbation of chronic obstructive pulmonary disease (AECOPD), relied on invasive mechanical ventilation. However, mechanical ventilation has several major drawbacks: sedation has to be induced and the air being pressed into the lungs with positive pressure can damage the pulmonary alveoli or the diaphragm. Moreover, even maximum ventilation frequently does not provide adequate gas exchange.
The extracorporeal ‘artificial lung’
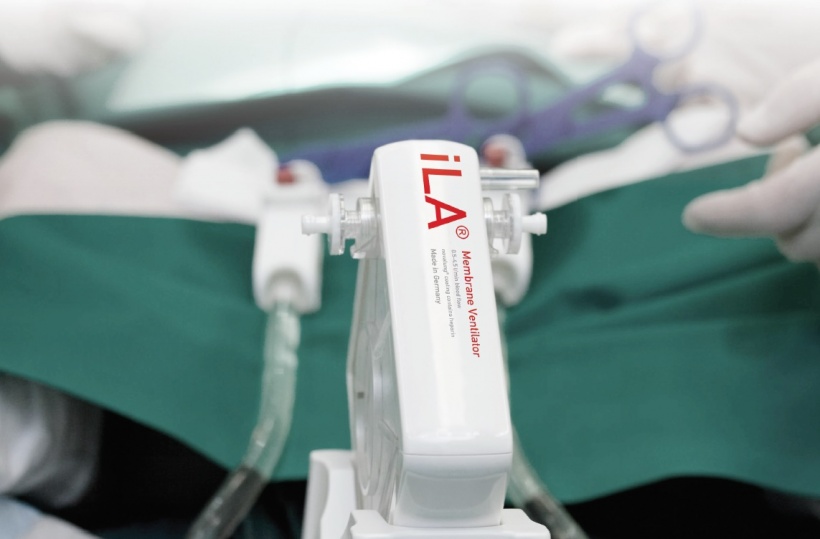
An advanced and easy-to-use alternative to such a trauma-associated invasive procedure is an extracorporeal ‘artificial lung’. It usually comprises a pump-driven pulmonary support system that removes carbon dioxide from the blood and adds oxygen. A key component of such a device is the so-called membrane ventilator which ‘breathes’ outside the body for the patient and carries out some of the gas exchange work of the native lung and at the same time relieves the respiratory muscles. A plasma-tight diffusion membrane is, for example, connected femorally to the body via a vascular access. It is supported by a blood pump that can be adjusted precisely, and instruments to control blood flow. The membrane ventilator can be used on the patient for up to 29 days.
Many advantages
The ‘artificial lung’ offers a broad range of support tasks – from efficient removal of carbon dioxide to full oxygen supply. The approach offers many benefits to patient and healthcare staff alike. Reduced stress on the patient’s respiratory system gives the lungs time to heal and the treatment is significantly less traumatic and more effective than conventional invasive procedures. The lung assist system does not require sedation, which means the patient is actively involved in the therapy and can eat and communicate. The entire hardware fits on a trolley, providing patient mobility during therapy.
Easy to use
Physicians and nurses can quickly height-adjust the membrane ventilator as needed in any particular situation, e.g. when the patient wants to lie down, sit up or be moved around. Subsequent therapies can follow sooner which translates into reduced length of stay and thus reduced costs.
Source: Xenios AG, Heilbronn, Germany.
05.03.2018





