CTLM Seeing through the dense breast
Optical imaging stands on the threshold of a vast array of imaging uses, writes Professor Eric N C Milne MD FRCR FRCP, Professor Emeritus of Radiology and Medicine, University of California Irvine, and Director of Clinical Research, Imaging Diagnostic Systems Inc. `Presently, its greatest worth lies in higher sensitivity for the dense breast. It detects many more occult cancers than conventional mammography´
“The overall sensitivity of diagnostic mammography in expert hands is about 70%. However, 40% of all breasts are dense, which means the mean sensitivity of mammography is only 45%, and probably the true sensitivity is lower than that. Many dense breast cases are classified BIRADS 0 and are called ‘true positives’ for audit purposes, although in the majority of these cases diagnosis was made using ultrasound or MRI. Without knowing in what percentage of these BIRADS 0 cases diagnosis was made using other imaging procedures, it is impossible to know the true sensitivity of mammography in dense breasts. Compounding the low sensitivity problem, the incidence of cancers in dense breasts is 4-6 times higher than in non-dense breasts, the type of cancer is usually rapid-growing and dense breasts occur more commonly in young patients, for whom ionising radiation should not be used.
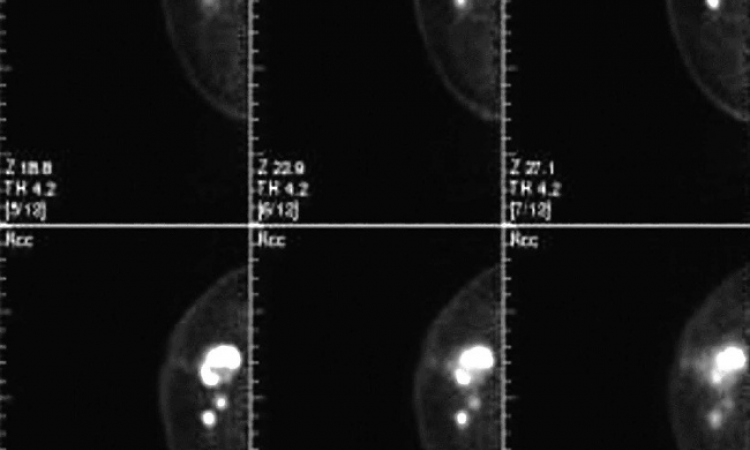
For all these reasons a new form of imaging is needed that can detect malignancies by revealing some of their functional characteristic, e.g. the presence of angiogenesis. This is the basis of Computed Tomographic Laser Mammography, which utilises a laser beam at 808 nm, matched to the light absorption characteristics of haemoglobin. At this wavelength water and fat have virtually no absorption. As a result the laser beam, (unlike X-irradiation), passes easily through the densest breast, but is absorbed by haemoglobin, which acts as a natural contrast medium, thus providing a haemoglobin angiogram of the breast.
Other than replacing the X-ray tube with a laser diode the system is similar to conventional X-ray CT, but the gantry is placed horizontally beneath the examination table, on which patients lie face-down with breast accessible through an opening in the table, and it is surrounded by the gantry ring. Nothing touches the breast and compression is not needed, nor is the breast surrounded by liquid or gel.
The gantry rotates around the breast 360 degrees, creating one tomographic slice. Then it descends 1-4 mm (operator’s choice), creates another, and progressively descends automatically until the whole breast is imaged, from chest wall to nipple. Scan time for each breast takes 5-15 minutes, according to breast size. Unlike ultrasound, production of an excellent CTLM image is not dependent on operator skills and usually a technician, not physician, undertakes the procedure.
Laser imaging is non-ionising and there is no X-ray generator, so no radiation protection is needed. The CTLM system can be installed in any room, using the standard electricity supply.
CTLM has few contraindications other than congenital protoporphyria, a recent tattoo on the breast, or surgery (including biopsy) within the previous three months.
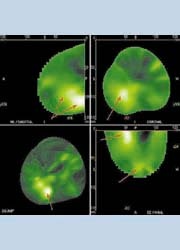
Reconstruction is in real time and the image is immediately available. Images are displayed on the physicians reading station as sagittal, coronal, axial and 3-D projections. The built-in software permits zooming the 3-D image to any size and display in several different formats, including Maximum Intensity Projection, (MIP) front-to-back (FTB) or surface-rendered, and window and level can be altered for optimal contrast.
Other built-in software permits animation, simultaneous synchronised comparison of images with different reconstruction displays, and the ability to ‘cut-away’ overlying normal anatomic structures to reveal angiogenesis optimally.
Due to intense scattering of light within the breast, reconstructing a CT light image is much more difficult than with an X-ray CT image and the resultant spatial resolution is not as high (1.0 mm resolution on surface), but this is not a clinical problem because the volume of angiogenesis associated with a malignancy is always much larger than the tumour itself... a 3.0 mm tumour can have angiogenesis 3-6 cms wide. This also helps in displaying tumours close to the chest wall, in which the associated angiogenesis extends much further into a breast than the tumour itself.
Results - Over 7,000 CTLM examinations have been performed to date at centres within the USA and throughout Europe, the Arab Emirates, Turkey and China. The most important point from these trials is that CTLM sensitivity, when used as an adjunct to mammography in the dense breast, is considerably higher than mammography sensitivity alone While mammography sensitivity drops progressively as breast density increases, CTLM sensitivity remains unchanged. So, as a breast gets denser, CTLM sensitivity, relative to mammography, increases progressively. CTLM therefore has the ability to find occult cancers missed by mammography in dense breasts
Future Uses
After breast cancer treatment: Since successful treatment with chemotherapy and/or radiation is accompanied by a progressive reduction in (and eventually complete disappearance of) angiogenesis, CTLM is an obvious candidate for following treatment, enabling rapid treatment alterations if angiogenesis is not reducing.
The CTLM system is adapted to image either by light absorption from the incident laser beam, or by recording fluorescence from the breast (from a fluorescent contrast medium) or by attaching a fluorophore to a tumour-seeking proteome. Presently under development, this will permit CTLM to become a unique imaging method to follow processes at the molecular level.
01.05.2006