CTLM for cancer detection in dense breasts
Paolo Belli MD, Carmen Malaspina MD and Professor Lorenzo Bonomo, of the Department of Radiology, UCSC, Policlinico A. Gemelli, Rome, discuss results from using computed tomographic laser mammography (CTLM) to detect cancers occult to mammography in dense breasts, and their comparison of CTLM with MRI to follow results of neo-adjunctive chemotherapy
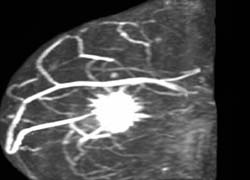
1a: MRI prior to neo-adjuvant chemotherapy in a 52-year-old patient with locally advanced breast cancer. A large volume of angiogenesis is present
Methodology - In a study involving four different investigational sites in the USA (University of Virginia, Elizabeth Wende Breast Clinic, Rochester and the Women’s Imaging Centre, Orlando, Florida,) and Mexico (National Cancer Institute, Mexico City) CTLM was used as an adjunct to mammography in 705 breasts of 515 subjects. Biopsy results were available in 451 cases. 40% of these patients were characterised as having breasts of mammographic density 3, ACR category ‘heterogeneously dense’, and 43% as ACR category 4, extremely dense. 34% of the patients had a family history of breast cancer. 115 patients had nodules alone, 108 had calcifications alone, and 15 patients had both.
Results – In these dense breast cases, sensitivity, specificity, NPV, and PPV were as shown in the table on page 11.
We believe the difference between the two sets of results is due to the fact that the pathologically ‘benign’ form of DCIS shows angiogenesis in only 30% of cases, whereas comedocarcinoma shows angiogenesis in 75% of cases, an observation that might prove useful for stratifying DCIS for treatment purposes.
One of the more remarkable results of using CTLM as an adjunct was that specificity also improved along with sensitivity, reducing the negative biopsy rate. Using mammography alone, specificity invariably drops as sensitivity increases.
Using imaging to follow the success of neo-adjuvant therapy for breast cancer. Is CTLM more sensitive than MRI?
MRI is being used increasingly to determine whether a particular treatment for breast cancer is succeeding and, for this purpose, has been considered the ‘imaging gold standard’. However, false negatives occur and residual tumour may be present, even when the MRI study has reverted to apparent normality (Yeh E, Slanetz P, Kopans DB, Rafferty E et al. ‚Prospective Comparison of Mammography, Sonography and MRI in Patients Undergoing Neo-adjuvant Chemotherapy for Palpable Breast Cancer’. Am. J Roentgenol. 2005; 184:868-8773).
Like MRI, CTLM images tumour angiogenesis in the intact breast, but it does not require ionising radiation or contrast medium. CTLM performs computed tomography with the same engineering approach, gantry and rotate/translate, as conventional X-ray CT, but replaces the X-ray tube with a laser diode tuned to 808nM, at which frequency the laser beam is selectively absorbed by both oxyhaemoglobin and deoxyhaemoglobin. CTLM utilises the body’s own haemoglobin as a natural contrast medium and therefore visualises both normal blood-containing structures in the breast, veins and lobes, and abnormal vascular structures, particularly angiogenesis. CTLM, therefore, provides both morphologic and functional information. (Helbich T. ‘Computed Tomography Laser Mammography’. European Hospital Vol. 13. issue 3/2004; 4-5.4)
Because of its ability to visualise angiogenesis, CTLM is being tested as an imaging method for following the success, or otherwise, of neo-adjuvant chemotherapy for breast cancer.
Comparison between CTLM and MRI
Figure 1a and b demonstrate, using MRI, what appears to be complete resolution of a cancer of the breast following neo-adjuvant treatment. However, a CTLM study made at the same time after treatment reveals definite residual angiogenesis (Fig 1c). Biopsy confirmed that residual tumour was present. These studies are in their initial phase but, from the preliminary data, it appears that CTLM may be better able to detect residual tumour following treatment than MRI. This might be because gadolinium preferentially images areas supplied by abnormally permeable vessels, whereas CTLM, by its mode of action, images every vessel supplying the tumour, whether normally or abnormally permeable.
Other advantages of using CTLM to follow changes in angiogenesis include the speed, comfort, and low cost of an examination, the ease and speed of interpretation, and the fact that CTLM is non-interventional.
20.06.2007
More on the subject:





