Article • Virtual Brain
Computer model simulates epileptic events
Approximately one percent of the world population are epileptic; in France alone, an estimated 600,000 people regularly experience seizures.
Report: Brigitte Dinkloh

During an epileptic event cortical neurons suddenly discharge, forcing their rhythm onto other nerve cells. This unusual and always temporary activity differs from person to person: it may manifest itself in a wide range of symptoms, from slight jerking of some muscle groups to serious convulsions and impediments of speech, memory, movement and behaviour.
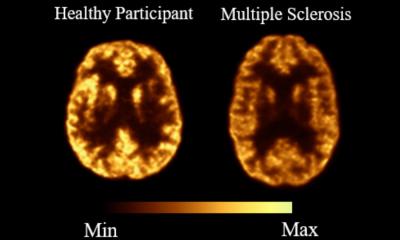
In the past, research instruments that could gather knowledge on epilepsy were limited because, in about 50 percent of those affected, neither MRI nor electroencephalography (EEG) show any visible brain anomalies. However, now researchers at the Centre National de la Recherche Scientifique (CNRS), the national institute of health and medical research (Inserm), Aix-Marseille University and the General Hospital Marseille (AP-HM), have succeeded in creating a virtual brain that not only allows modelling the originating sites and trajectory of abnormal brain activity but which can also optimise the planning of surgical interventions.
In 70 percent of epileptic patients the seizures can be managed by medication. ‘When medication is not sufficient, however, surgery has to be considered,’ says Dr Fabrice Bartolomei, Medical Director of the Department of Neurophysiology at Hôpital de la Timone in Marseille, France. ‘In a first step the epileptogenic area is identified and, in a second step, it is removed or neutralised.’
An MRI head scan is performed to localise the abnormal brain activity. MRI offers both an anatomy snapshot and – helped by the 3-D modelling technique tractography – the reconstruction of the course of larger neural tracts. A second source of information is EEG. ‘Brain activity is recorded by electrodes which, under general anaesthetic, were implanted into the brain by the neurosurgeon,’ Bartolomei explains. ‘The electrodes are placed in areas the surgeon considers important to understand the origin of an epileptic event and its propagation in the brain,’
Innovative and less invasive techniques are currently being tested, such as magneto-encephalography (MEG), which discovers and maps changes in the magnetic fields on the surface of the skull. An entirely new approach is the ‘virtual brain’, which ‘…allows us to personalise a mathematical model for each individual patient,’ explains Dr Viktor Jirsa, Director of Neuroscience Systems at CNRS, ‘and provides a visualisation that enables individual simulations.’
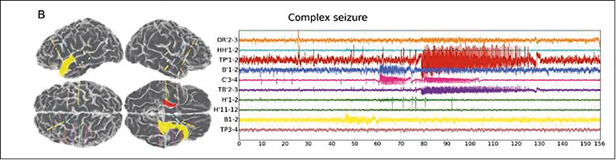
By visualising brain activity and detecting the origins of an epileptic event and its spread in the brain, the virtual brain technology offers a more precise diagnosis. Surgeons can mark the surgery regions of interest and plan and even test the most effective and least invasive surgical cuts. Thus different scenarios and their effects on the brain can be simulated. Bartolomei explains: ‘In a first step the MRI and EEG data are transferred to the model. In a second step, electrical impulses are applied to nodes in the model, particularly in the areas that are most likely epileptogenic. Thus epileptic events can be triggered and visualised in the virtual brain and the source, as well as spread of abnormal activity, can be reconstructed.’
In each patient the interaction of nodes in the brain is different. The virtual model allows prediction of the effects of a given surgical intervention at a given node. The surgeon can remove certain areas of the virtual brain and see whether the epileptic events continue to develop, or whether cutting the connections, so to speak, has stopped the event. This technology increases plan-ability and efficacy of epilepsy surgery. The model, however, cannot predict any surgical side effects.
In Marseille, the virtual brain is almost already used to plan interventions. An evaluation of the patients who underwent surgery remains to be done. There is a long way to go for researchers: they need to assess whether the virtual brain indeed provides an accurate picture of the epileptic event. Bartolomei estimates another 18 to 24 months before the model can be used in a clinical setting. Since, in epilepsy, electrical biomarkers are very specific, transfer of the model to other neurodegenerative diseases will not be easy.
Profile:
Neurologist Fabrice Bartolomei, specialist in epilepsy, is a professor at the Aix-Marseille University (http://edu.univ-amu.fr/en) in France, leading the neurophysiology service clinic. He is also medical director of the Centre Saint-Paul at the Henri Gastaut Hospital (http://www.hopital-gastaut.com), one of Europe‘s oldest hospitals to manage epilepsy, after a few pioneeers established epileptology following WWII. Today the hospital treats 3,000 adults and children annually. Bartolomei has published numerous epilepsy studies, particularly on the concept of Epileptogenic Networks and on the relationship between stress, emotions and epilepsy. He has largely contributed to the promotion of EEG/SEEG analysis in focal epilepsies and is the co-inventor of the Epileptogenicity Index, a method to assess epileptogenicity of brain regions.
30.03.2017