Why standards matter
By Michelle Jeandron, science and technology reporter, Institute of Physics Publishing*
Better measurement standards for high-intensity focused-ultrasound (HIFU) are necessary.

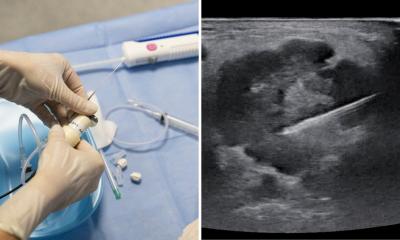
HIFU therapy is a promising, non-invasive cancer treatment that uses ultrasound to destroy deep-seated tumours with pinpoint accuracy. Basically, powerful ultrasound beams are brought to a focus within an area of malignant tissue, the intensity being sufficient to raise the temperature of the cells and kill them. What’s more, the threshold intensity is only reached at the focal point, such that surrounding healthy tissue is left unharmed.
‘HIFU will find its niche clinically,’ explained Gail ter Haar, head of therapeutic ultrasound at ICR and president of the International Society for Therapeutic Ultrasound. ‘It is the only technique that offers trackless tissue destruction, so it is of particular interest in the brain, where it can be carried out under MRI guidance. Other advantages are that it is bloodless, repeatable, has low systemic side-effects compared to chemo- and radiotherapy, and it may not need anaesthetic - although currently anaesthetic is used to suppress patient movement.’
Despite these advantages, HIFU is currently only approved in the UK for the treatment of prostate cancer, with more than 13,000 patients treated worldwide with promising five- and seven-year follow-up. In the USA it has also been approved for the treatment of uterine fibroids. ‘In terms of clinical effectiveness, it compares well with other ablative therapies,’ added ter Haar. Meanwhile, preliminary trials are taking place for the use of HIFU on other cancers (e.g. liver and kidney), though it is still a long way from being a widely available therapy.
Standard logic
HIFU relies on quite different ultrasound fields to those commonly used for medical imaging. The pressures and intensities involved are much higher, for example, and HIFU involves strong focusing and nonlinear field harmonics.
‘There are known limitations with both the measurement devices and procedures, which become particularly important when attempting to deliver the very high energy densities produced by HIFU systems,’ explained Adam Shaw, a senior research scientist within the NPL’s acoustic team. ‘These limitations introduce very substantial uncertainties in attempting to characterise the true acoustic field: for instance, the uncertainty in determining the temporal-average intensity at the focus is typically a factor of two.’
All of which makes life difficult for researchers, clinicians and equipment developers - and makes the case for international standards on HIFU all the more pressing. For starters, standardisation will allow researchers to characterise the exposures in their biological studies with much greater accuracy, and in turn allow proper comparison of results from different groups from around the world.
Standards will also mean that equipment from different manufacturers can be compared fairly and the most appropriate system purchased depending on a hospital’s needs. However, the big benefit to the equipment suppliers ‘is that there will be a recognised and universally accepted method for demonstrating compliance on safety and essential performance’, said Shaw. That should mean reduced time to market for new devices and ‘will lead to patients benefiting from the widespread availability of a safe and effective alternative to radiotherapy, chemotherapy and surgery’.
For their part, NPL and ICR are working on a number of fronts to fast-track the introduction of HIFU measurement standards. Key initiatives range from the development of reference techniques for measuring fundamental quantities like pressure and power to the production of test objects for checking the registration between the imaging system used to locate the target tissue and the therapy field. Other priorities are the development of specialised thin-film temperature sensors, tissue-mimicking materials and rapid qualitative methods for pre-treatment system validation.
Shaw concluded: ‘The first step towards accepted international standards for HIFU has been taken with an agreement to produce an IEC [International Electrotechnical Commission] technical report in the next 12 months.’
* http://medicalphysicsweb.org
17.11.2006