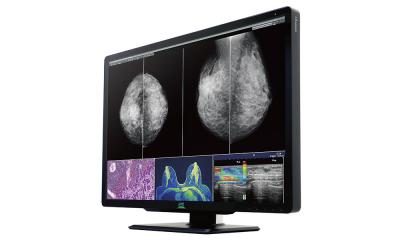
Whole Body MRI for Vascular Screening
Article by Stefan G Ruehm MD, Associate Professor of Radiology, Director, Cardiovascular CT, at the David Geffen School of Medicine, UCLA.
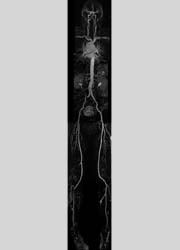
Atherosclerosis is a serious health problem in developed countries and will likely emerge as the main cause of worldwide morbidity and mortality. Treatment strategies such as surgical procedures, percutaneous catheter based interventions or pharmacological options depend on the accurate classification of atherosclerotic disease with respect to location, extent, and severity of arterial involvement. For this purpose several imaging techniques, including conventional catheter angiography, duplex ultrasound, computed tomography-angiography (CTA) as well as magnetic resonance angiography (MRA) are in clinical use. It is well known that atherosclerotic disease is a systemic disease, usually affecting the entire arterial system. However, vascular imaging techniques commonly use a segmental approach, yielding diagnostic information limited to a single vascular territory. This largely results from inherent limitations of the established imaging techniques, such as risks associated with invasiveness, restrictions concerning contrast and radiation-dose as well as cost and time constraints. 90% of atherosclerotic lesions are identified below the aortic bifurcation. Thus the lower limbs are the most frequently affected vascular territory. Presently, peripheral vascular disease (PVD) accounts for 50,000-60,000 percutaneous transluminal angioplasties, implantation of 110,000 vascular prostheses and 100,000 amputations annually in the USA alone.
PVD is frequently associated with carotid, coronary, and renal arterial disease reflecting the systemic nature of atherosclerosis.
A comprehensive assessment of the underlying vascular pathology is required to manage atherosclerotic disease adequately. Lack of ionising radiation and non-nephrotoxic contrast agents in combination with a high diagnostic accuracy have prompted the rapid implementation and acceptance of MR angiography as the modality of choice for evaluating arterial disease in many institutions worldwide.
Associated tissue enhancement outside the vascular tree and contrast dose limitations had initially limited contrast-enhanced 3D MRA to the display of an arterial territory contained within a single field-of-view extending over 40-50 cm. The implementation of ‘bolus chase’ techniques allowed extending the coverage to visualise the entire run-off vasculature, including the pelvic, femoral, popliteal and trifurcation arteries. The implementation of faster gradient systems, which have become available on the latest generation MR systems, enabled the extension of the bolus chase technique allowing for whole body coverage extending from the carotid arteries to the trifurcation vessels with acquisition times for up to five three-dimensional (3-D) MR angiographic data sets of less than two minutes.
In a recent study, whole-body MRA was employed in 180 consecutive patients (3,000 vascular segments) with suspected peripheral vascular disease (Ruehm et al., Int J Cardiovasc Imaging. 2004;20(6):587-91). The used dose of contrast agent was comparable to the dose commonly used for peripheral MRA. The examination time of less than 15 minutes per study can be regarded as very short and exceeds the examination time for monostation MR angiography by less than 10%.
The use of whole-body MRA revealed additional and clinically relevant disease in 42 out of 180 patients (48 vascular segments), including renal artery stenosis (27 cases), carotid arterial stenosis (21 cases), subclavian artery stenosis (5 cases), and abdominal aortic aneurysm (7 cases). Confirmatory studies in 20 patients, performed based on the additional vascular pathologies detected by whole body MRA, revealed no false positive or false negative findings.
The high degree of concomitant arterial disease in patients with PVD underscores the systemic nature of atherosclerosis. Patients with intermittent claudication are at particularly high risk for atherosclerotic disease in other parts of the circulation. Studies on the prevalence of coronary artery disease in patients with peripheral vascular disease show that the history, clinical examination, and electrocardiography typically indicate the presence of coronary artery disease in 40-60% of such patients. Coronary artery disease often may be asymptomatic and masked, because patients may be capable of only limited exercise. The link between peripheral vascular disease and cerebrovascular disease seems to be weaker than that between peripheral vascular and coronary artery disease. Duplex ultrasound has revealed carotid disease in 26-50% of patients with peripheral vascular disease and this group of patients is considered at increased risk for cerebrovascular events.
Approximately one-fourth of patients with peripheral vascular disease have hypertension. The possibility of renal artery stenosis should be considered in these cases. In the examined study population 22 patients (12%) had renal artery disease with a degree of stenosis exceeding 50%.
Globally, expert panels have advocated targeting high-risk individuals for primary prevention. Risk factors, which are known to predict cardiovascular events, include systemic hypertension, cigarette smoking, elevated levels of cholesterols and triglycerides as well as low levels of LDL, and diabetes mellitus. All these risk factors are readily identifiable by a combination of physical examination, laboratory analysis, and patient history. Whole-body MRA offers a unique opportunity to assess what damage, if any, has already been inflicted on the vascular system. It might serve as an adjunct to further stratify the risk of a patient with a certain constellation of laboratory and clinical findings.
Arguments are ongoing about the value of screening all patients with peripheral vascular disease, symptomatic or not, particularly for carotid disease and aortic aneurysms. Patients with claudication are undoubtedly more likely to have significant asymptomatic disease in these vascular areas than the general population. Nevertheless the treatment of asymptomatic carotid disease remains controversial. Whereas findings in more recent studies appear to indicate an unequivocal benefit associated with the treatment of advanced carotid artery disease, the issue of the yield versus the cost of such screening tests is significant.
When discussing the value of screening patients for abdominal aortic aneurysms (AAA) several points must be considered. For unknown reason, the prevalence of abdominal aortic aneurysm has been increasing steadily over the past 40 years. Furthermore, AAAs are rarely symptomatic until they rupture, by which time the opportunity to intervene has usually been lost. In addition, the mortality rate of aneurysm rupture generally exceeds 80%.
Selecting asymptomatic patients to screen for AAA remains a controversial topic with a wide range of recommendations. In random screening groups, the incidence of AAA is reported to be 2-3%, with 75% of the aneurysms found in individuals over 60 years old. The likelihood of having AAA is increased in smokers, older individuals, males, and individuals who have CAD, PVD, or a first-order relative with aortic aneurysm.
Therefore screening for AAA in patients with PVD may be an important way to eliminate a preventable source of mortality, because an abdominal aortic aneurysm is asymptomatic, life threatening, treatable and amendable to detection by noninvasive tests.
In summary, whole-body MRA allows for a quick, risk-free, and comprehensive evaluation of the arterial system. Whole-body MRA is characterised by its noninvasiveness, three-dimensionality, extended coverage and high contrast conspicuity. The technique is well suited for the assessment of the peripheral vasculature with comparable diagnostic accuracy compared to MRA studies focused on the lower extremity vessels only. In addition, it yields accurate data regarding the remainder of the arterial system.
However, it is noteworthy that the outlined technique, although referred to as whole-body MRA, does not include the intracranial or coronary arteries. For both vascular territories a dedicated approach is still required. Nevertheless, whole-body MRA offers the opportunity to integrate dedicated imaging protocols for the cerebral vasculature and cardiac imaging. Time-of-flight (TOF) MR angiography, a flow dependent imaging modality that does not require the additional administration of contrast agent, can easily be added for imaging of the intracranial vessels. This technique is sufficient to detect small intracerebral aneurysms.
MR display of the coronary arteries remains challenging. Encouraging results have recently been demonstrated based on the combined availability of navigator-techniques and intravascular contrast agents. However, at present the latest generation of 64-slice multidetector computed tomography (MDCT) systems appear to provide more reliable results in patients with suspected coronary artery disease.
Conversely, MR imaging offers the opportunity to most accurately assess right and left ventricular ejection fractions, cardiac mass, and valve function. Furthermore the evaluation of myocardial contractility, both under rest and stress conditions, is feasible, as well as the identification of transmural and nontransmural subendocardial infarcts. The additional incorporation of a cardiac imaging algorithm would prolong the vascular screening protocol based on whole-body MRA by approx. 30 minutes.
Ongoing hard and software improvements, including dedicated surface coil designs, automated table motion techniques, parallel imaging protocols, particularly in combination with high field scanners (3T) and the recently introduced 32-channel MR systems, as well as the development of new MR contrast agents, promise to further add to the practicability and diagnostic accuracy of whole-body MRA.
Contact: sruehm@mednet.ucla.edu
01.03.2006