Article • The right tool for the task
Vascular insights with MRI and ultrasound
Advances in image post-processing and contrast-enhanced techniques have widened the scope of possibilities for MRI and ultrasound vascular imaging, experts showed in a dedicated course at the ECR Overture.
Report: Mélisande Rouger
CT offers high-resolution images of the vasculature structure at unrivalled speed. However, these are not necessarily the most important aspects for imaging vulnerable patients. For these populations, ultrasound and MRI remain the modalities of choice. With the help of new techniques, they can now help obtain information on vascular structures in unprecedented ways, speakers explained in the session.

Image source: Vogel-Claussen Heart and Lung Imaging Lab
Combined with contrast, a high-resolution 3D magnetic resonance angiography (MRA) allows imaging the arteries anywhere in the body and especially at the periphery, explained Prof Jens Vogel-Claussen, Vice Chair of the Institute of Diagnostic and Interventional Radiology at Hannover Medical School, Germany. ‘Time-resolved MRA enables to depict dynamics in nice details,’ he said. Creating an image every few seconds, the technique allows tracing of the contrast agent through the body, resulting in a dynamic depiction of the vasculature.
Cyclic agents used in MR examinations are considered to be safe in patients with good renal function, but the debate around gadolinium has renewed interest in working with non-contrast techniques that can image the complex interaction between breathing and blood flow. Black and bright blood, time of flight and phase-contrast techniques are well-established non-contrast MRA methods that have been used in clinical routine for over a decade.
PREFUL-MRI: A ‘blockbuster’ lung imaging technique
More recently, Vogel-Claussen and his team pioneered a technique called phase-resolved functional lung (PREFUL) MRI, which depicts dynamic ventilation and perfusion of the lungs without contrast in spectacular detail. ‘It’s a blockbuster,’ he said. ‘Before, you had to undergo a nuclear medicine test to obtain the ventilation on top of the perfusion information. Now you can have all that information without radiation, without contrast agents and in free breathing.’
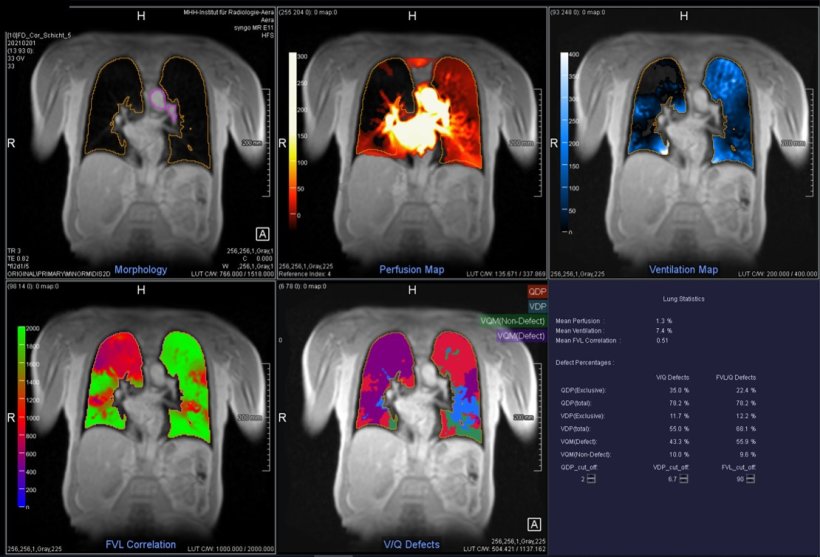
Image courtesy of Prof Vogel-Claussen
The technique traces the pulse wave and reconstructs the cardiac cycle using post-processing imaging, allowing for the dynamic measurement of the vasculature structure. ‘We can show all phases of the ventilation and perfusion cycles,’ Vogel-Claussen explained. While the ventilation results are similar to those obtained with spirometry, the characteristics of the blood flow can be extracted from the same image, due to the interplay of ventilation and perfusion in the lung.
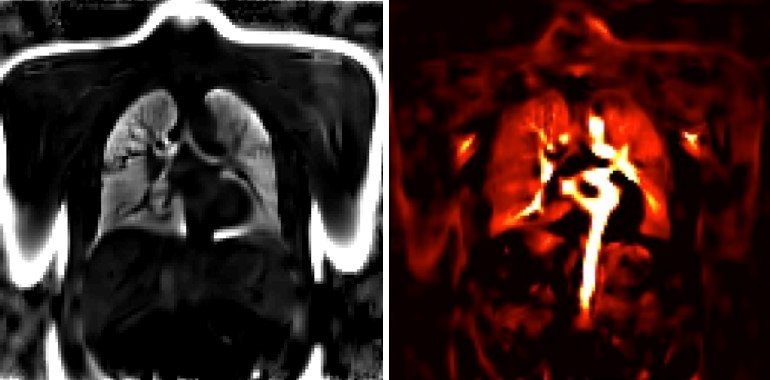
Image courtesy of Prof Vogel-Claussen
Post-processing imaging in PREFUL-MRI improves image quality and reduces scan time on almost any scanner – a significant advance for many vulnerable patients. ‘Imaging preterm babies with cardiac failure now takes five minutes and one slice takes about one minute,’ the expert said. Since the technique relies on echo flash sequences, which are available on any scanner, results are highly reproducible, he pointed out.
An array of ultrasound techniques

Image source: Kelen Kórház
Ultrasound is still the most popular and widely used examination to image the vascular structures, explained Dr Zoltan Harkanyi, a consultant radiologist at the department of radiology, Heim Pal National Pediatric Institute in Budapest, Hungary, in the following talk. ‘It’s the only modality that is totally harmless and easy to tolerate for patients,’ he said, adding its widespread availability to the list of benefits. On the other hand, ultrasound is a highly user-dependent technique, with great differences in quality and performance from one examination site to another.
With conventional methods such as B-mode, colour Doppler and spectral Doppler, ultrasound has helped analyse and measure flow velocity for the past 30 years. ‘Ultrasound is very useful to assess certain diseases like carotid artery stenosis, when the brain blood flow needs to be checked,’ he gave an example. The stenosis is typically caused by plaque or calcification in the internal carotid artery – a tell-tale sign that is easy to detect with ultrasound.
Hypertension is another common application for ultrasound, especially in patients who suffer from renal disease and can’t undergo a CT or MRI scan. Different software solutions are available today that also enable assessment of the microvascular structure and exploration of tiny vessels with high resolution without contrast injection (Fig.1).
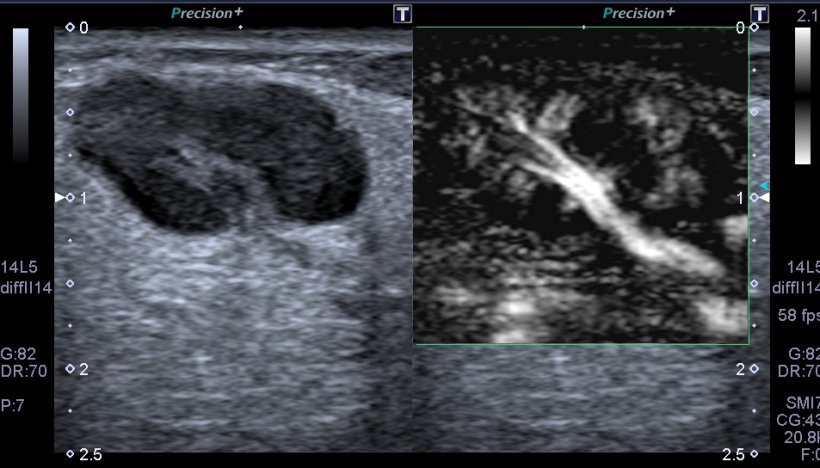
Image courtesy of Dr Harkanyi
CEUS: The benefits (and challenges) of adding contrast
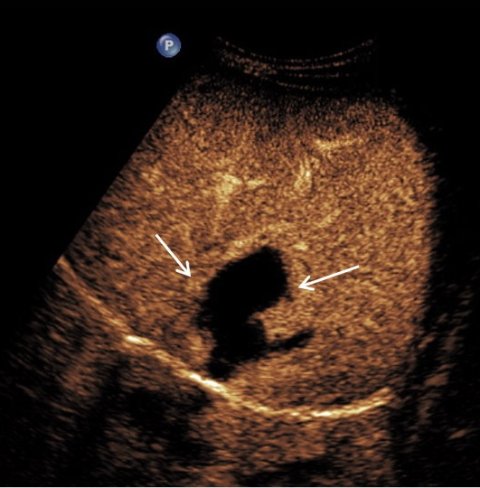
Image courtesy of Dr Harkanyi
To explore vascular structures in complex organs such as the liver, contrast enhanced ultrasound (CEUS) presents with significant benefits. ‘CEUS enables to assess the vascular structure of the liver and behind the malignant and benign masses in the organ,’ Dr Harkanyi said. ‘It’s very useful to visualise tumours, but it can also be used in liver or spleen trauma, to check the extent of the parenchymal injury’ (Fig.2).
The examination only takes 10 minutes from the moment the contrast media is injected into the arm vein. Acknowledging the increasing prevalence of CEUS in Europe for both paediatric and adult patients, the expert also pointed out some limitations of the technique: For one, a special software must be installed, which bars middle- and low-end systems from using CEUS. And even if the system does support said software, users still have to learn how to use it, Harkanyi said.
The expert suggested that CEUS should be used in well-designed indications, for example differential diagnosis between a focal nodular hyperplasia or haemangioma (Fig.3). Dr Harkanyi recently helped explore this clinical situation, by contributing to a book on how and when to use the technique in paediatric imaging.1 ‘For microvasculature structures in a liver or kidney tumour, ultrasound can add further clinical evidence to establish diagnosis. Ultrasound is also an ideal tool to follow-up oncology patients once they’ve been treated,’ he concluded.
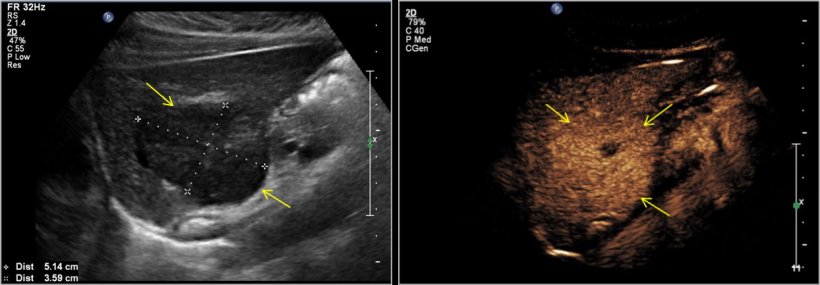
Image courtesy of Dr Harkanyi
1 Contrast-Enhanced Ultrasound in Pediatric Imaging Eds. Sidhu P /Sellars M /Deganello,AM. Springer 2020
Profiles:
Zoltan Harkanyi, MD, PhD, is a consultant radiologist at the Department of Radiology of Heim Pal National Pediatric Institute, Budapest. He has worked as a radiologist and researcher at Thomas Jefferson University, Philadelphia, USA, and has been recognised as an adjunct assistant professor of the University since 1991.
Prof Dr Jens Vogel-Claussen is Vice Chair of the Institute of Diagnostic and Interventional Radiology at Hannover Medical School, Germany. He is also Head of the Section for Cardiopulmonary Radiology at the Institute of Diagnostic and Interventional Radiology, Hannover Medical School. Dr Vogel-Claussen previously worked as an Assistant Professor of Radiology on the Faculty Body Imaging at Johns Hopkins University School of Medicine Department of Radiology in Baltimore, USA, where he completed his residency under the leadership of Prof Stanley Siegelman. He is principal investigator at the German Centre for Lung Research (DZL) and has written 118 peer-reviewed journal articles.
19.05.2022