MEDICA 2013
Two sides of the coin
A one-day course on Infection Prevention and Control (20 November. 9.30 a.m. - 6.00 p.m.) will focus on a vital issue at the Medica Education Conference 2013.
In the run-up to the event, in discussion with European Hospital, Professor Franz-Josef Schmitz MD, the Course Chairman and Senior Consultant at the Institute for Laboratory Medicine, Microbiology, Infection Prevention and Control, Environmental Medicine and Transfusion Medicine at the Mühlenkreiskliniken in Minden, Germany, outlined the challenges and potential solutions.
Pointing out two problem areas in infection prevention and control, he said: ‘More and more antibiotics are being administered in out- and in-patient treatment, which puts so-called selective pressure on the bacteria. This means that many pathogens are increasing resistance and a decreasing number can be successfully treated with antibiotics. We also see that these resistant pathogens can spread rapidly if infection prevention and control is inadequate.
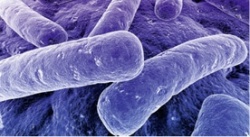
‘So, on the one side we have the spread of nosocomial pathogens when infection prevention and control is inadequate and, on the other, the increasing use of antibiotics, which leads to the pathogens becoming increasingly resistant against certain groups of antibiotics. The problematic pathogens are known – Methicillin-resistant Staphylococcus aureus (MRSA) Vancomycin-resistant Enterococci (VRE), multi-resistant gram-negative bacteria (MRGN) and the toxin-producing Clostridium difficile (CDI).
Improving control in hospitals
‘In Germany, and some other countries, it took a long time to address the problems with the required intensity. The training of more infection and prevention control support staff and specialists in individual hospitals – which is currently being implemented in this country – is a sensible measure which, in the medium and long-term, will lead to increased awareness, and which could possibly prevent the expected, potential increase in nosocomial infections and pathogens. It remains to be seen whether in fact it will also achieve a decline in the number of these infections. At the very least it’s an attempt to tackle the problem and there is a realistic chance that the situation can be improved.’ Although unlikely to solve the problem in the short term, the professor expects those measures to have a successful impact in five to ten years’ time.
Tackling the cause of resistance – by law
‘The Dutch pursue the principle that broad-spectrum antibiotics should only be used after a microbiological consultation. In Germany, doctors have the freedom to prescribe, but even here there are efforts in many hospitals to prescribe these ‘reserve’ antibiotics only after microbiological testing, and only after the respective approval from the local pharmacist.
‘However, hospitals make up only a proportion of where antibiotics are being used, although their use, especially the peri-operative administration of antibiotics, should still be reduced. Antibiotics are used far more commonly in veterinary medicine, and in (human) out-patient care. Reductions in the use of antibiotics in animal husbandry as well as in out-patient care are desirable. In animal husbandry it should certainly be possible to make this a legal requirement, but in out-patient care colleagues would need convincing and respective training provided.
‘For infection prevention and control in hospital, financial aspects are decisive. The more staff is made available, the easier carrying out prophylactic measures will be.’
Of one thing Prof. Schmitz is certain – only if both nurses and doctors on wards are trained in infection prevention and control will awareness be raised and infections contained. ‘More awareness of this topic amongst politicians is therefore extremely desirable,’ he concludes.
20.11.2013