Three tiny grills deliver high contrast X-rays
Mammography scans with lower dose and higher contrast – that’s the declared goal of Dr Nik Hauser, Medical Director of the Women‘s Clinic and Director of the Interdisciplinary Breast Centre at Kantonsspital Baden, Switzerland, and Professor Marco Stampanoni of Paul Scherrer Institute in Villigen, Switzerland.

By building upon a procedure used in materials research to cull more information from X-rays the added significant value to mammography for breast cancer diagnosis. When passing through tissue, X-rays are not only absorbed but also refracted and scattered. The researchers used this additional information to generate breast scans with more detail and higher contrast that show even minute tissue changes.
‘While this principle is theoretically suited for any anatomy, it presented itself for breast scans, because of the high proportion of soft tissue in the breast, which means the effects are particularly well visible,’ Dr Hauser explained.
Core components of this innovative procedure are three tiny grills, one being placed directly behind the X-ray source, the two others behind the tissue sample. ‘By slightly moving these grills we can see which X-rays pass through the tissue and which are attenuated. Since these effects happen at the molecular level, the grills have to be of nano dimensions to be able to register the minute angle scattering of the X-rays,’ the Director of the breast centre explained. The detector records this information, which is transferred onto separate images.
In a next step the conventional absorption image of the mammography and the new scatter images are fused. Alternatively, the grills can be used to generate the usual image quality at lower dose.
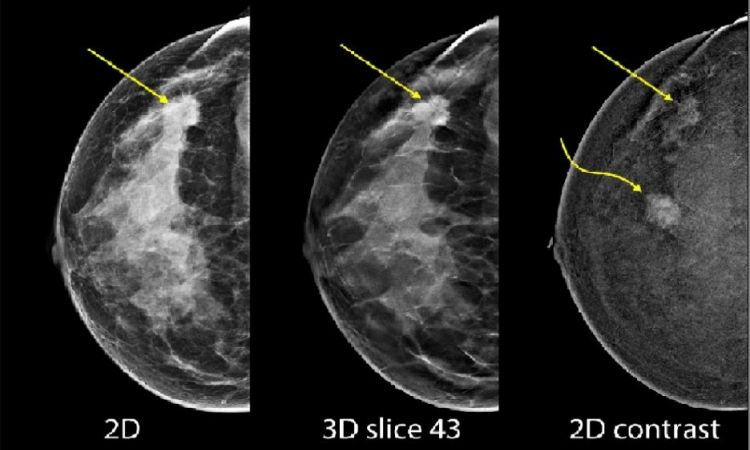
The fusion image allows a better evaluation of breast tissue. Minute structures are visualised in enhanced sharpness, which enables more precise evaluation of microcalcifications and tissue changes. Even the fine extensions of the growth are distinctly recognisable.
The fusion images themselves can be presented in different ways, e.g. with colour codes. However, the radiologists who evaluated the images in the Hauser/Stampanoni study stuck to familiarity – black and white.
Whilst Dr Hauser is sure this technique can also be used in 3-D, in vivo studies come next. He hopes to present data next year. So far, the researchers have performed their tests on mastectomy samples. To be able to use the technique for human patients the mammography systems will have to be equipped with the grills. ‘Currently,’ he explained, ‘we are working with a prototype that is not suitable for clinical routine use. Right now, we are fitting the grills and make sure that the system remains stable and precise and that the results are reproducible. The foundation has been laid.’
The research project aims to achieve enhanced quality, resolution and diagnosis using the same radiation dose as conventional digital mammography to be able to detect and treat tumours earlier. ‘If this method turns out to improve tumour detection and delineation and thus pre-surgery evaluation,’ Dr Hauser confirms, ‘I’m sure it will prevail.’
Thanks to increased sharpness cancer could be detected at a very early pre-stage.
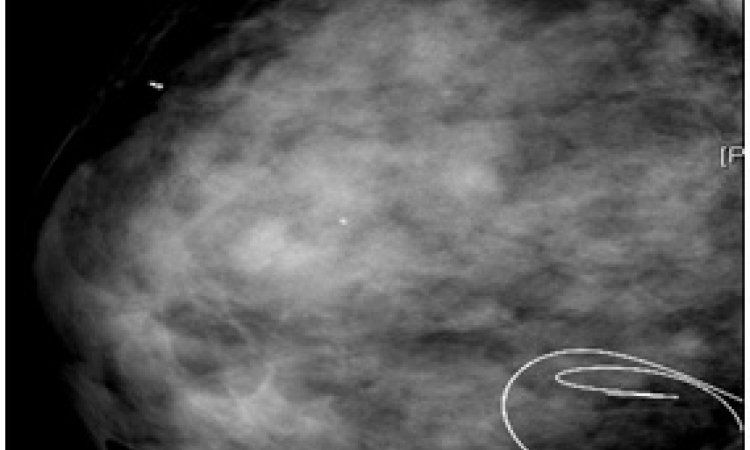
X-ray images of breast tissue generated with conventional mammography and with the new mammography procedure. The latter show a significant improvement in image sharpness and visibility of the tumour extensions (right). Image: Paul Scherrer Institute/Kantonsspital Baden
Profile:
Chemistry graduate Nik Hauser MD worked at domestic and foreign university hospitals before studying medicine at the University of Basle. Specialising in gynaecology and obstetrics, he gained five years’ clinical experience at the renowned Women’s Clinic in Ulm University Hospital, Germany.
10.03.2014