Article • Zincmolybdat
The sustainable pathogen killer
Professor Peter Guggenbichler is only too aware of infection prevention and control issues in hospitals. Prior to his retirement in 2013, from the Children’s Hospital at Erlangen University Hospital, in Germany, he led the Infectiology and Preventive Medicine Department, for 25 years. ‘After countless nights on the intensive care ward I realised that the staff does not adhere to infection prevention and control guidelines because, realistically, these cannot be adhered to,’ Guggenbichler explains.

MEDICA EDUCATION CONFERENCE
Thursday, 17 November, 02.10 p.m. – 03.30 p.m.
Room: 16
Hygiene: Groundbreaking approaches for infection control in healthcare
Chairman: Prof. Dr. J. Peter Guggenbichler, Kössen, Austria
According to the guidelines, nurses and doctors are supposed to disinfect their hands between 50 to 80 times during just one shift. After each fifth to sixth application of a disinfection agent they should also wash their hands because otherwise the hand disinfection agent merely spreads the dirt. According to the infection specialist this is not achievable: ‘Staff would spend more than an hour per shift on hand disinfection, and in case of emergencies there is no time for this, anyway. This prompted me to think about alternatives and to precisely analyse the workflows in the hospital and on the intensive care ward.’
Every year around 5% of in-patients in Europe develop hospital acquired infections (HAIs). Of the 1.75 million patients affected, at least 10%, i.e. around 175,000 people, do not survive this (source: www.ESCMID 2015). The risk of nosocomial infections is therefore higher than the risk of being involved in a road traffic accident.
The staff’s hands are contaminated but so are hospital surfaces, and pathogens and multi-resistant organisms are transmitted with every touch. Be it hospital furniture, touchpads, control knobs, cables, floors, computer keyboards or telephone receivers – as soon as something is touched it is no longer germfree, even if previously disinfected. Surfaces that can kill pathogens would therefore be ideal – and this is exactly what Guggenbichler has worked on for years, initially with antibiotics and disinfection agents and, since the 1990s, also silver.
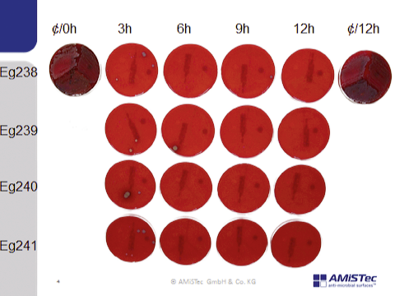
‘In 1999 we developed an outstanding silver technology, which is still effective for external ventricle drainages for intracranial pressure, and is therefore still successful on the market. However, the most silver technologies do not work for the impregnation of surfaces because the pathogen-killing silver ions are used up after 3-5 weeks. As with disinfection agents and antibiotics, silver ions are incorporated into the metabolism of microorganisms, so they must be dissolved out of a hydrophilic surface and are then lost. This means that a number of silver technologies on sale is basically ineffective, and this is not being questioned enough.’
Guggenbichler and his team have now developed a technology which, with the help of various transition metal acids (mostly zinc molybdate in situ, i.e. the polymer itself), can generate H30O+ ions, reactive oxygen species and photocatalytic activity from tiny amounts of water, and this has a strong antibacterial effect on the surface. ‘The basic assumption about the effective mode of action is that hydrating oxonium ions (H3O+)(OH2)n (n=1.3) in contact with micro-organisms initially remove the hydration water and finally also the remaining water molecule. The now naked protons can attack the cell walls of bacteria in an unspecific way by permanently denaturising their protein shells and fimbriae. Additionally, the protons can block the effect of essential enzyme systems inside the cell. The entire process is known as proteolysis (coagulation necrosis),’ the scientist explains.
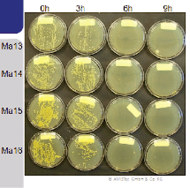
The result is a slightly acidic surface, similar to the acid mantle of the skin, which, with a pH value of 4.2 – 4.5, quickly kills germs. Additionally, there is the positive zeta potential, i.e. a positively charged surface that attracts negatively charged microorganisms, so that overall there is a synergistic effect. Zinc molybdate is neither water nor alcohol soluble, so cannot be removed by disinfectants. It is thermally stable and non-toxic. Both elements, molybdate and zinc, are essential trace elements in the body, which even if they should become dissolved, remain below the permitted threshold level for 24 hours by factor 250.
‘Obviously nurses will have to continue washing and disinfecting their hands, but if they forget to do so once in a while the consequences will be less dramatic. The new technology is a kind of safety valve: instead of disinfecting hands 60 times a day it can be done every 20-30 minutes instead, because the surfaces will remain self-disinfecting for many years.’ To achieve this, there is no need to refurbish the entire hospital because the zinc molybdate can be applied retrospectively as a transparent film to telephone receivers, furniture and fittings etc. like any normal lacquer.
Guggenbichler already discovered this mode of action around ten years ago. But his discoveries really gathered pace since his retirement from the hospital and the foundation of the start-up company AMISTec, and patients will soon benefit from this.
Paints and lacquers for large medical devices are now ready for use. However, the possibilities go way beyond this; airline seats, car air conditioning systems, shower trays and even underwater power cables will soon be self-disinfecting. We can only hope that hospitals will not miss the boat. With the rapid increase of multi-resistant pathogens and talk of the post-antibiotic era, there is an urgent need for action in the prevention of infection.
Details: www.krankenhaushygiene.de/informationen/hygiene-tipp/hygienetipp2015/557
Profile:
Josef-Peter Guggenbichler studied medicine at the University of Innsbruck and qualified as a paediatrician at the Mayo Clinic, Rochester, Minnesota, USA. After his return to Austria he became a professor at the University of Innsbruck (1980-’90) and then he worked as an extraordinary professor at the Department for Infectiology and Preventative Medicine at the Children’s Hospital, University Hospital Erlangen, Germany (1990- 2009). Guggenbichler holds more than 30 patents for the antimicrobial impregnation of surfaces and is cofounder and managing director of the start-up company AMISTec
(www.amistec.at) founded in 2011.
10.11.2016





