Interview • Diffuse liver diseases
The liver is a master of deception
Professor Dr Thomas Kröncke, Medical Director of Diagnostic and Interventional Radiology at Klinikum Augsburg, has been dealing with liver diseases for 17 years. Talking to European Hospital he explains which diseases the liver tends to mask and why fatty liver has become a public health issue.
Interview: Daniela Zimmermann
Why is diffuse liver disease so difficult to diagnose?
Thomas Kröncke: Diffuse diseases, unlike focal liver diseases where lesion can be characterized with diagnostic imaging, do not necessarily show unambiguous signs. Thus they are not obvious in contrast imaging, particularly if the entire liver tissue is involved.
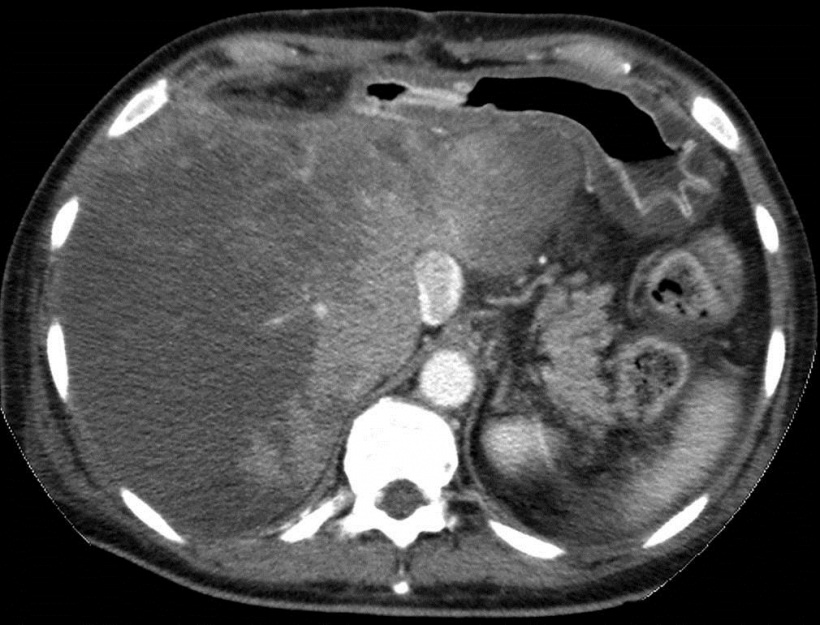
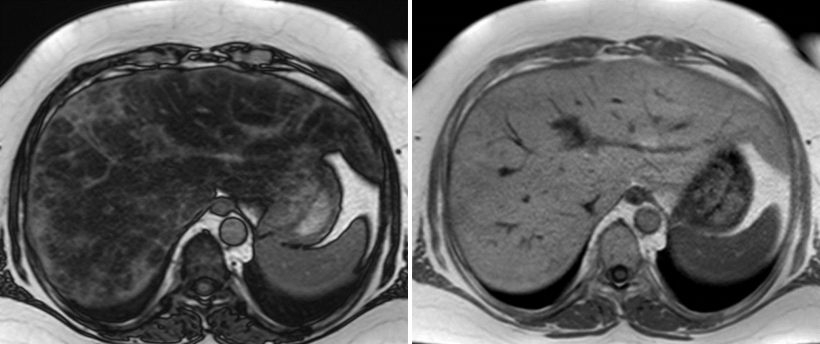
Heterogeneous but typical perfusion pattern with low peripheral and high central perfusion of the liver.
So how can they be diagnosed?
Firstly, information provided by the referring physician can be of great help. In addition it is crucial to look for minute differences such as density in the CT scan or anomalies in contrast media uptake or wash-out. A scan that might look unsuspicious at first glance may well show a problem upon close scrutiny. Experience and different perspectives can make or break a diagnosis.
Which imaging modalities do you use?

Ultrasound remains the first line modality as it does provide a lot of information. Nevertheless, it is not suited for all issues. When we are dealing with diffuse liver disease, CT and MRI are essential, with the advantage of MRI being able to “measure” the entire organ rather than providing isolated values. In addition, more recent developments such as MRI elastography can prove helpful for diagnostic purposes. Before, the only way to determine elasticity of liver tissue, or rather lack of elasticity caused by fibrotic changes in the liver tissue, was by palpation or invasive biopsy. Elastography allows us to quantify tissue characteristics for the entire organ which is particularly beneficial for patients with reversible pre-stages of cirrhosis.
Which types of diffuse liver disease do you encounter most frequently?
Fatty liver has undergone a dramatic change in the way we perceive its significance. We used to treat fatty liver as an irrelevant incidental finding which we tended to ignore. Today it is not only diagnosed more often but it is also considered a risk factor for other diseases as it can easily lead to steatohepatitis and thus cirrhosis. In recent years, steatohepatitis has moved into the focus due to increasing obesity, particularly among children and adolescents. Thus fatty live disease, which in extreme cases leads to cirrhosis and even requires a liver transplant, has become a very real problem.
Fatty liver disease has thus evolved from secondary importance to a bona fide problem?
Indeed. The problem with fatty liver disease is the fact that it can either conceal other diseases or look like other diseases. On the one hand, liver fat compromises contrast in imaging procedures making the detection of lesions and tumours more difficult. On the other hand, tissue changes associated with fatty liver can look like lesions – but they aren’t. In order to be able to differentiate between the two it is important to understand where exactly fat tends to accumulate in the liver and perform additional exams. Certain MRI frequencies, for example, precisely tell you what type of tissue we are dealing with. An exact diagnosis, however, requires a lot of experience.
Is diffuse liver disease a potential field of application for Big Data and artificial intelligence?
Diffuse liver disease presents in many variations and not only can pathological tissue changes have many different causes they can also provide valuable information
Thomas Kröncke
Not more than any other area where diagnostic imaging plays an important role. Going forward, we will no doubt see many changes brought about by technological progress, after all the computer is superior to human beings in terms of stamina but that applies to radiology at large, not only to certain areas. It is much more important to crack conventional ways of thinking. Liver does not equal cirrhosis. Diffuse liver disease presents in many variations and not only can pathological tissue changes have many different causes they can also provide valuable information. This means we have to take a closer look.
Does that mean what looks like cirrhosis might in fact be a completely different disease?
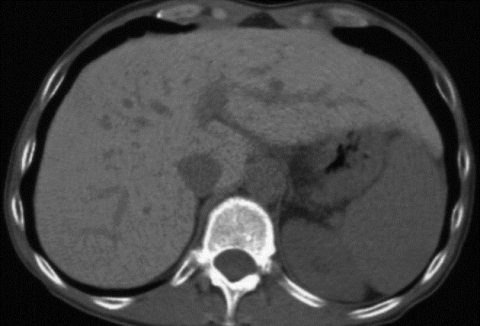
Yes. There are liver conditions, so-called pseudocirrhoses that have structures and a bumpy surface that are very similar to real cirrhosis. Chemotherapy, for example, can cause the characteristics of cirrhosis. Another phenomenon is obliterative portal venopathy meaning the obliteration of the intrahepatic portal vein branches. Moreover, there are certain metabolic conditions that manifest in the liver such as a hereditary impaired copper metabolism. In view of these possibilities it is crucial to remain open and don’t get sidetracked by red herrings. The liver is a master of deception – a phenomenon that fascinated me when I did my first research on atypical fatty liver – and still fascinates me today.
Profile:
Professor Dr Thomas Kröncke is Medical Director of the Clinic for Diagnostic and Interventional Radiology and Neuroradiology at Klinikum Augsburg, Germany. In 2016 he was appointed Extraordinary Professor at the Medical Faculty of Charité Berlin. His specialisations are interventional radiology (image-guided minimally invasive interventions), liver imaging, oncological imaging and cardiac and vascular imaging.
29.11.2017