Article • Non-pulmonary aspects
The cardiovascular impact of Covid-19
The increased Covid-19 risk to cardiac patients was discussed during an online presentation at ECR 2020.
Report: Mark Nicholls

The increased Covid-19 risk to cardiac patients was discussed during an online presentation at ECR 2020. Focusing on the prevalence of pulmonary embolism in Covid-19 patients, Dr Karl-Friedrich Kreitner, Professor of Radiology at the Department of Diagnostic and Interventional Radiology at the Johannes-Gutenberg University in Mainz, Germany, discussed hypotheses which can explain cardiac involvement in the course of the disease, and help delegates understand imaging findings of cardiovascular complications.
The ‘Non-pulmonary aspects of Covid-19’ session, which outlined pathology research on Covid-19, described the many clinical manifestations of the infection and introduced the concept of multi-organ involvement. Alongside Dr Kreitner’s presentation on cardiac issues, other contributors will spoke of neurologic manifestations, and the disease in paediatric patients.
Speaking to Healthcare in Europe ahead of his presentation, Dr Kreitner stressed that although the virus uses the ACE-2 receptor predominantly located in lung tissue to enter a human, this receptor is also present elsewhere in the body. ‘It’s also in up to 10% of myocardial cells and in endothelial cells of arteries and veins,’ he explained. ‘If you are aware of this then you come to the conclusion that the infection is not exclusively localised in the lungs, but can affect other organs as well, including the heart and pulmonary vasculature.’
Recommended article

Article • Coronavirus disease research
Seeking a COVID-19 antidote: the potential of ACE2
As coronavirus disease COVID-19 continues to jet and alight invisibly around the globe, scientists now report that the virus has mutated to become two strains: the older ‘S-type’ appears milder and less infectious, while the later-emerging ‘L-type’, is more aggressive, spreads more quickly, and currently accounts for about 70 per cent of cases. Worldwide, medical researchers are exploring…
Among in-patients who die of the disease, Kreitner said there is evidence that not all died due to lung tissue destruction, but there were also other causes, notably pulmonary. Lab data can help clinicians to assess the risk of Covid-19 patients sustaining thromboembolic disease, he said, in particular checking the D-dimer or fibrin degradation products (FDP) as markedly-elevated D-Dimer and FDP are common in non-survivors of Covid-19.
Recommendations suggest that patients with a D-dimer level below one have a lower risk of thromboembolism than those presenting with a level over one. ‘In these newer recommendations there is some risk stratification; that with a D-dimer between one and two you should think of controlling this value and do pulmonary embolism imaging in the further course of the disease. If presenting with values above two, you should immediately test to see whether the patient suffers from pulmonary embolism or not. Generally, if values are below one, you can treat these patients with a prophylactic dose of low molecular weight heparin and where the value is above two, you should consider a therapeutic dose of low molecular weight heparin.’
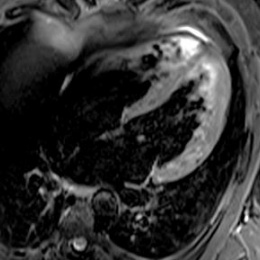
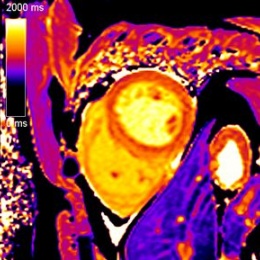
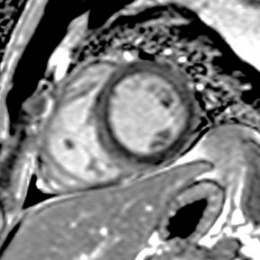
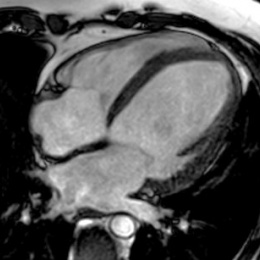
One presented with a typical viral myocarditis and the second with dilated cardiomyopathy-like appearance with signs of inflammation, so the phenotypes of cardiac involvement have a great diversity
Karl-Friedrich Kreitner
The challenge, he pointed out, is to weigh up lowering the risk of thromboembolism against the increased risk of haemorrhage, and it is very important to look at these values when the patient is admitted to hospital. ‘With cardiac involvement, Covid-19 patients suffering a cardiovascular disease have a much higher risk of dying from the condition. This is perhaps because their cardiovascular system is not fit enough to face the challenges of this SARS-CoV-2 infection.’ In such cases, clinicians should turn to cardiac biomarkers, especially high-sensitivity troponin and the NT-pro BNP because, when they are elevated, the individual is at a greater risk.
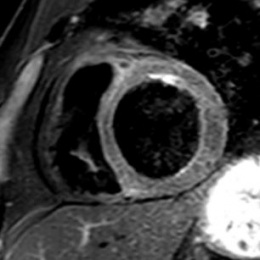
While much of the evidence of this has come from China, Italy and the USA, Dr Kreitner discussed two patients from his department who presented with different forms of Covid-19 myocarditis. ‘One presented with a typical viral myocarditis and the second with dilated cardiomyopathy-like appearance with signs of inflammation, so the phenotypes of cardiac involvement have a great diversity.’
He also spoke of a study conducted in the Institute of Legal Medicine in Hamburg following autopsies on the first 80 patients who died from Covid-19 in that city: 40% had thromboembolisms. Kreitner advised that, in the cases of suspected thromboembolism, timely imaging should be initiated. ‘The main points are that cardiovascular involvement has a significant impact on prognosis for in-patients and it is absolutely necessary to control for D-dimer, fibrin degradation products, hi-sensitivity troponin and the NT-pro BNP during admission and the course of the hospital stay. This, especially for D-dimer and FDP; when they are elevated an anti-coagulative therapy should be considered and the amount – or whether it is a prophylactic or therapeutic dose - depends on the D-dimer value.’
Profile:
Dr Karl-Friedrich Kreitner is Professor of Radiology at the Department of Diagnostic and Interventional Radiology of Johannes-Gutenberg University in Mainz, Germany. He has published more than 200 articles in peer reviewed journals and 29 contributions to books. He is co-editor of the books Cardiac Imaging: A Multimodality Approach and Radiological Differential Diagnosis and Great Vessels.
15.09.2020