Article • MRgFUS
Successful therapy for uterine fibroids using MRgFUS
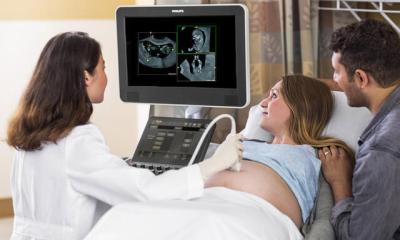
Magnetic Resonance Guided Focused Ultrasound (MRgFUS) therapy was introduced in June at the Amperklinikum in Dachau, near Munich, the third German site, after Berlin and Bochum for this new technology.

Dr Matthias Matzko, Head of Radiology at the Dachau Clinic and Professor Gerlinde Debus, Head of its Gynaecology Department, presented the advantages of this non-invasive ablation procedure for uterine fibroids. Bernd von Polheim, President of GE Healthcare Germany and Dr Dov Maor, Vice President Clinical Marketing InSightec, representing the two companies involved in the technical development, were also at the press presentation. 'The surrounding tissue is not damaged by heat and the fibroid is literally melted off through the release of energy. Moreover, the procedure replaces surgery, the patient is not exposed to radiation, there is no need for anaesthetic and the patient can be discharged the same day. In addition the therapy is painless. Fibroids are benign and therefore non-hazardous muscle tumours; however, depending on size and location they can cause substantial problems, or prevent pregnancy. Current studies show that patients undergoing MRgFUS have the best chances to have fibroids removed without impairing fertility. As many women want fibroids removed, because they hope to become pregnant, the Dachau Clinic has decided to offer MRgFUS as an alternative to minimally invasive surgery, such as fibroid embolisation. The procedure is really fascinating and has great potential,’ said Dr Matzko. ‘Fibroid therapy is only the beginning. We’d like to be to the fore with this application and further developments from the start. We also hope to treat other diseases, e.g. breast cancer, for which there are already some phase II therapy studies in other hospitals, which have shown malignant breast tumours up to 1.5cm can be melted off with focused ultrasound.’
Is fibroid size significant using MRgFUS?
‘Unlike malignant breast tumours, in the uterus we can treat fibroids of any size, but this must be done over several sessions. Two factors are decisive for the success of non-invasive fibroid therapy: location and number of vessels in the fibroid.’ He continued. ‘If the growth is too saturated with vessels, the blood vessels act as cooling aggregates and heat around our focus point is absorbed. In this case, we can offer a patient hormone therapy prior to ultrasound therapy, to decrease the vessels in the fibroid. We combine the procedures because fibroids only decrease while hormone therapy is given, then they grow back. ‘The second factor: We cannot ablate if the position of a fibroid means that the ultrasound beam goes through critical structures, such as the intestine. The danger of burning is too great, as temperatures of 60-80 degrees are reached after only a few seconds.
Therapy for a medium-size fibroid takes 2-3 hours. What of the strain on a patient who must not move in the MR machine? The patient has a light sedation and pain killers, making lying more comfortable. As long as she doesn’t move much, nothing can happen. The MR image shows us with a delay of only three seconds what is happening in the body at any given time. Both systems are fine-tuned to each other so precisely that we can repeatedly redirect the US energy right on the fibroid. Moreover, during the planning stage we put land markers within the fibroid and exclude the critical structures prior to commencing treatment. However, it is not a problem to interrupt a therapy session, and then carry on in a second session if there is a lot of fibroid tissue, or if the patient requests it.'
The future of MRgFUS
‘We’ll be better than surgery’ Dr Dov Maor is one of the founders of InSightec, a subsidiary of GE Healthcare. AsVice President for Clinical Marketing, he develops and presents the new MRgFUS and its clinical applications to European medical and academic communities. Seeing that MRgFUS is already successful in the treatment of fibroids, we asked him what other use he foresees for this technology. ‘Initially, we began our work with breast cancer research. As physicists and engineers, we assumed that the breast would be easy to treat because the tissue is soft and easily accessible. Then it transpired that this is not the case. Moreover, it was very difficult to carry out studies in this field, which would confirm that malignant tumours can be removed non-invasively. Surgical treatment procedures for breast cancer in its early stages have already been established. It’s a long way tocertification of our procedure. However, we remain convinced that we will be able not only to avoid surgery but also be better than surgery. Whereas a surgeon cannot differentiate between tumour tissue and healthy tissue during an intervention, we can trace a tumour’s outline very precisely using MRI during a procedure. This saves time and drawn-out follow-up treatment.
‘Our next big project will be the therapeutic treatment of metastasising or primary liver cancer. Here we face completely new technological challenges – first, the liver moves position during breathing and second, it is largely obscured by the ribs. In most patients, the liver cancer is situated under the bone. That’s why we are working on the development of a special applicator that can aim between the ribs. We hope to start clinical trials for this in about 18 months. We also hope to use the same method for the treatment of kidney tumours, or maybe even pancreatic tumours. We have already gathered promising results from our procedure for the palliative treatment of bone metastases, and received the European licence last year. Although bones are not made of soft tissue, which can be focused on as precisely as our other targets, we have been working on a strategy for years to replace radiation with MRgFUS. Radiation is only successful in around 70% of cancer patients in advanced stages of cancer and has strong side effects. We’d like to offer procedures for the palliative treatment of pain that put less strain on the body, particularly for patients with advanced stage cancer. Additionally, we are currently researching the use of MRgFUS to treat brain problems. This not only focuses on oncological treatment, but also on central nervous system problems, e.g. epilepsy. Sometimes it suffices to destroy just the smallest pieces of brain tissue to rectify malfunctions. This is why we’ve developed equipment that allows us to focus on the brain through the intact skull. We are working in cooperation with the Neurosurgery and Neuroradiology Departments of the Brigham and Women’s Hospital, Harvard University, and University Hospital Zurich, wheredoctors have already identified centres in the brain responsible for certain functions. Last month they received clearance from the Ethics Commission to treat the first patients. The potential of MRI guided Focused Ultrasound is far from exhausted,’ he concluded. ‘However, the development processes for these systems are long and it’s a long way from a technological concept to clinical application!’
01.07.2008