Article • Tomosynthesis
Ready to take over?
Results from recent trials are promising: an almost 40% increased breast cancer detection rate from digital breast tomosynthesis (DBT) screening compared to conventional mammography.
Report: Bettina Döbereiner
Therefore, is an introduction of DBT to screening already a realistic scenario? The pros and cons will be discussed at this year’s ECR by radiologist and DBT specialist Sophia Zackrisson.
The technology in itself is not new. The principle of tomosynthesis was already invented in the early 1930s. The basic idea: several low dose X-ray projections are made in a limited rotation angle around an object. Afterwards, these projections are reconstructed into three-dimensional images. Even though tomosynthesis has a lower radiation exposure than computed tomography (CT) it was put in the shade for a while and often only named ‘limited angle computed tomography’.
DBT solves overlapping tissue problem
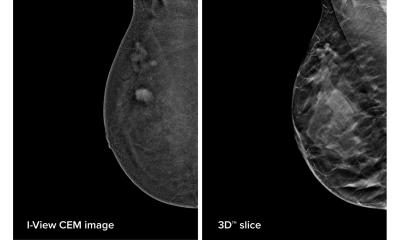
In the late 1990s, tomosynthesis was reborn and continuously improved – above all in breast imaging, then called digital breast tomosynthesis (DBT). The big advantage of 3-D DBT is that it reduces the effect of overlapping breast tissue that may hide or simulate a tumour in standard mammography projection imaging. ‘In the 3-D image where you get 1 mm thin slices, suddenly you can see the tumour very clearly,’ explains Sophia Zackrisson, radiologist at Skåne University Hospital in Malmö, Sweden. It is not a real 3-D image, DBT does expose in a 15° to 60° angle and not in a 360° angle around the breast as in a CT scan.
The Malmö Trial: One view DBT detects 40% more breast cancers
Two recent large-scale and population based trials compared two view digital mammography (DM) and two view DBT in the so-called combo mode with two view DBT. The STORM-trial (Screening with Tomosynthesis OR standard Mammography) and the first results of the Oslo-Trial showed a significantly increased detection rate of breast cancers in screening by using the combination of DM and DBT.
The Malmö Trial (Malmö Breast Tomosynthesis Screening Trial) from Lund University, Sweden, now proved, for the first time, that even one view DTB as an exclusive method is superior in cancer detection than digital mammography. B background: Typically, a screening mammogram contains two projections from different angles - the mediolateral oblique (mlo) and the craniocaudal (cc) view. However, even with one view DBT (mlo) 40 percent more breast cancers can be detected compared to the two view digital mammography, as the findings of the Malmö-Trial now showed. The characteristics of the additionally found cancers using DBT appear to be the same as with conventional mammography screening. Up to now, no statistically relevant differences could be proven - we have to wait for the final publications of the Oslo and Malmö trial in the next two years.
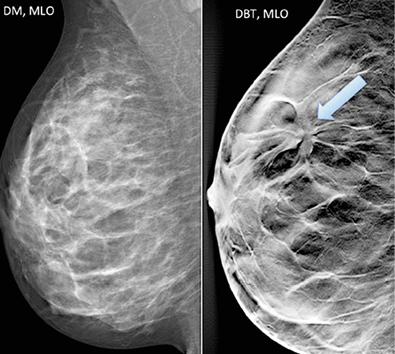
Could DBT replace 2-D mammo screening already?
All these promising results from the recent trials could suggest that DBT is ready to become the future gold standard of mammography screening – for this device not only detects more cancers in women, according to Sophia Zackrisson DBT also makes it easier to stage a cancer and its size-estimation is more accurate. Additionally, another positive effect must be mentioned: if DBT is used in the same way as in the Malmö trial it is more women-friendly than mammography because it reduces procedural discomfort. Zackrisson estimates that, in the trial, the compression force on the breasts in DBT-screening was halved. In 2-D mammography compression is needed to reduce the radiation dose and to separate overlapping tissue; but in DBT the separation effect is already solved by the multi-angle-technique that reduces the overlapping tissue effect per se. Also, if only one view DBT is used, as in the Malmö trial, the radiation exposure is lower. Altogether - what stops us subsequently to introduce this new method of screening – bearing in mind that DBT is widely used in the USA already?
DBT screening: possibly in five to seven years

Sophia Zackrisson believes there are several reasons that should stop us going fast forward. First: we must wait for the final publications of the Oslo and the Malmö trial. Next comes the important and not yet answered question: Does DBT-screening also affect breast cancer mortality in the population? For ethical and economical reasons, Zackrisson does not recommend randomised mortality studies to evaluate whether DBT reduces breast cancer deaths in the long run. Instead, she suggests waiting for the follow-up analyses of the trials to see whether DBT screening has an effect on the interval cancer rates – a term for cancers that are detected within the period up to the following screening. In general the rate of interval cancers is used to assess the efficacy of breast imaging. ‘I’d like to see at least some trend of decreasing interval cancer rates in the trials before we translate tomosynthesis into screening,’ Zackrisson says. According to her this is important to know, because otherwise it could indicate that DBT is over detecting and its additional findings represent just very small, indolent, non-aggressive tumours that never would have appeared clinically later. However, Zackrisson seems to be confident that DBT will replace 2-D mammography in the long run. Not yet, but approximately in the next five to seven years.
ECR 2016 - Don't miss
Sophia Zackrisson will speak during the following dates:
• 2 March. 12:15-13:45, Studio 2016: ‘Is digital breast tomosynthesis ready for mamm-screening?’
• 5 March. 16:00-17:30, Room F2.: ‘Should we abandon 2D mamography?’
• The prof. is also moderator for the Satellite Symposium ‘Digital breast tomosynthesis out of the daily routine.’
2 March. 14:00-15:30, Studio 2016.
01.03.2016